Back to: Gynaecology
Urogynaecology
Urinary Incontinence
This is a very important gynaecological condition which has a huge impact of patients’ lives.
– There are two main types of incontinence in females, each of which have different pathologies and treatments.
– It affects about 4-5% of the population, being more common in elderly females
i) Urge Incontinence
This is the involuntary leakage preceded/accompanied by a sudden desire to pass urine
– It occurs due to an overactive bladder due to increase detrusor muscle overactivity
Causes:
Mostly idiopathic but can be associated with neurological conditions (e.g. MS, PD)
– Can be made worse by diuretics, coffee, alcohol, concurrent UTIs
ii) Stress Incontinence:
This is the involuntary leakage upon increased intra-abdominal pressure (e.g. coughing, sneezing)
– It occurs due to weakening of the pelvic floor muscles, so they do not compress the bladder neck
Causes:
Pregnancy, vaginal delivery, obesity (these all weaken the pelvic floor muscles)
Tests:
These are needed to distinguish between the two main types of incontinence
– Abdominal examination –> to look for palpable, enlarged bladder suggesting retention
– Vaginal examination –> to assess pelvic muscle tone and look for prolapse (a sign of pelvic floor weakness)
– Urine dipstick –> to check for UTI
– Bladder diaries –> Ask to patient to complete a bladder diary for a minimum of 3 days
– It allows you to see if there are any triggers and how much fluids patients drink
If it is still unclear, then urodynamic studies are indicated.
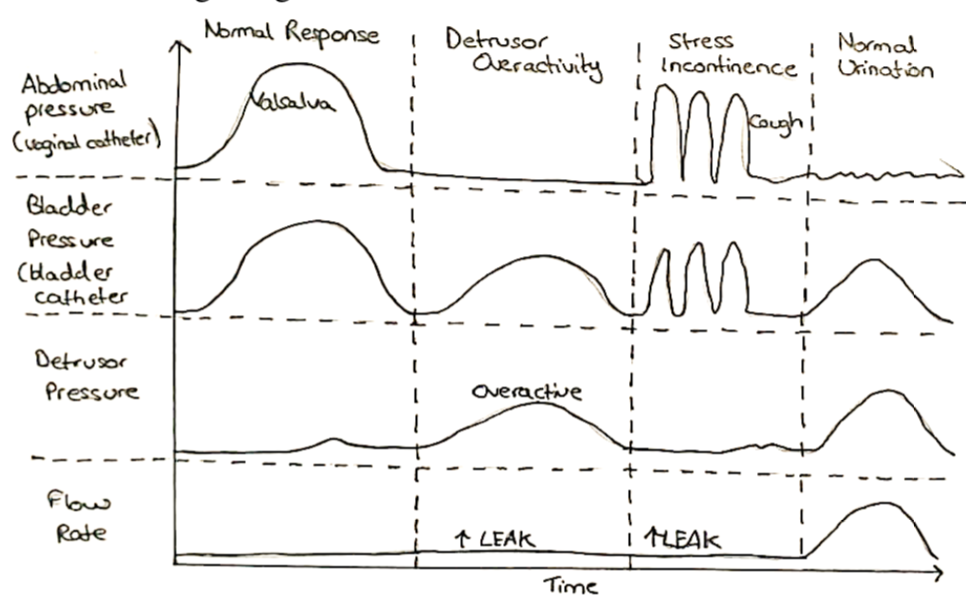
Urodynamic studies
This tests pressure changes of the detrusor muscle with a fluid challenge
– Put one pressure sensor in the bladder to measure intra-bladder pressure
– Put second sensor in the vagina/rectum to measure intra-abdominal pressure
– If you take the difference, then it allows you to work out the true detrusor pressure
a) Urge incontinence:
– You ask the woman at what volume filled in the bladder she feels the first urge to go to the toilet.
– If overactive bladder, the bladder and detrusor pressure will
increase at a low filling volume and cause leakage, without
any increase in abdominal pressure.
b) Stress incontinence:
– A cough or Valsalva will cause a rise in abdominal pressure
– This is transmitted so that intra-bladder pressure also rises
– The true detrusor pressure stays zero as it is not contracting – Usually there should be no leakage of urine from the bladder
– However, in stress incontinence a cough causes leakage without causing a rise in detrusor pressure
– This therefore shows that that the leakage is due to weakness of the pelvic muscles, rather than detrusor muscle overactivity
Management (NICE1):
– Common to both types, reduce caffeine, regulating fluid intake, weight loss (if BMI 30+) and stop smoking
For Urge Incontinence:
1st line = Bladder retraining (at least 6 weeks)
2nd line = Antimuscarinics: Oxybutynin, Tolterodine, or Darifenacin
3rd line = Mirabegron (B3 agonist) if antimuscarinics are contraindicated
Secondary care treatments:
• Botox —> Dangerous side effect is urine retention, so patients must be willing to self-catheterize
• Sacral nerve stimulation —> used for women who refuse to have catheters with Botox
For Stress Incontinence:
1st line is Pelvic floor muscle exercises (3-month trial of 8 contractions, 3 times a day)
2nd line = Surgery -> options include:
• Autologous rectal fascial sling: abdominal wall fascia is used to form a sling around the urethra
• Retropubic mid-urethral mesh sling: procedure in which mesh is used as a urethral sling
• Intramural bulking agents: silicone injection which adds bulk to urethral sphincter (wears off)
• Colposuspension: procedure in which the bladder neck is tethered to the surrounding tissues
3rd line = if the patient does not want surgery, offer duloxetine
Urogenital Prolapse
This refers to a descent of one of the pelvic organs resulting in protrusion on the vaginal walls
– It is most often due to childbirth
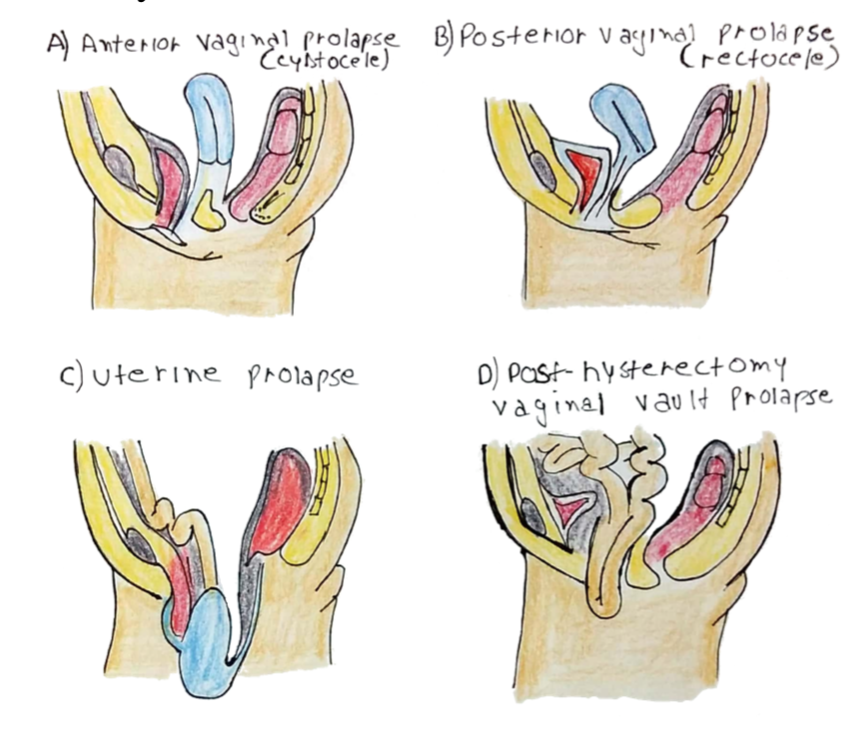
– It is defined by the organ which protrudes on/out of the vagina.
– Bladder = Cystocele
– Uterus = Uterine prolapse
– Rectum = Rectocele
– Procidentia = Whole uterus + Cervix
Risk factors:
Weakening of the pelvic floor -> older age, pregnancy and vaginal delivery, obesity
Symptoms:
– Dragging discomfort/sensation of heaviness in the vagina
– Feeling that something is coming out of the vagina –> patient may be able to feel a protruding bulge
– Urinary symptoms –> increased frequency, incomplete emptying, stress incontinence
Staging:
It is staged according to the distance the organs reach from the hymenal ring
– Stage 1 = when you can displace the uterus but not up to 1cm of the vaginal opening
– Stage 2 = when the prolapse reaches the hymenal ring
– Stage 3 = when the prolapse reaches 1cm out of the hymenal ring
– Stage 4 = When the whole organ prolapses out of the vagina
Tests:
– Speculum examination –> Ask the patient to adopt the left lateral position and insert a Simms speculum
– After insertion, ask the patient to cough raising abdominal pressure
– Bimanual examination –> Uterus is more mobile and moveable
Management:
1st line is pelvic floor exercises (8 contractions, 3 times/day for 3 months)
2nd line is pessary –> This must be changed every 6 months and gives small risk of urinary retention
– If rectal or bladder prolapse –> use ring pessary
– If uterine –> use shelf pessary
3rd line is surgical repair:
– Cystocele –> Anterior repair
– Rectocele –> Posterior repair
– Uterine –> Laparoscopic hysteropexy
4th line is Hysterectomy
If stage 4 prolapse an option is sacral-spinous fixation (SSF)
–> Organs are fixed to the sacrum and spinous processes completely immobilising them
–> Risk of bleeding due to damage to pudendal venous plexus + bad buttock pain due to irritation to the pudendal nerve
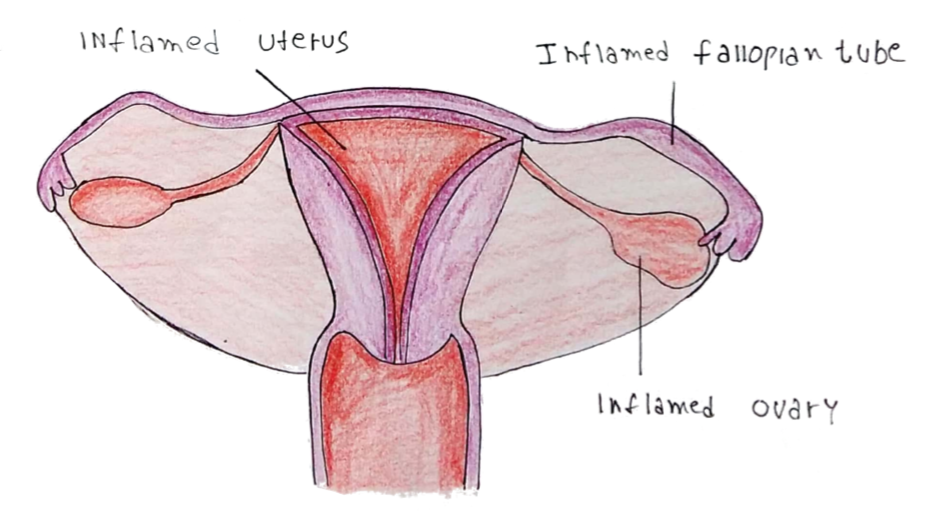
Pelvic Inflammatory Disease (PID)
An inflammatory condition affecting the pelvic organs like the uterus, oviducts, ovaries and peritoneum
– It is usually caused by ascending sexually transmitted infections which arise from the endocervix
– Chronic inflammation gives scarring and fibrosis which leads to pain and menstrual problems
Causes:
Chlamydia trachomatis (most common), Neisseria Gonorrhoea, Mycoplasma genitalium
Symptoms:
– Fever
– Pelvic + lower abdominal pain
– Deep dyspareunia (different to the superficial dyspareunia experienced in menopause)
– Vaginal/cervical discharge
– Abnormal vaginal bleeding
– On bimanual examination -> adnexal tenderness, cervical excitation (pain elicited when two fingers used to move cervix), abnormal discharge
N.B. If untreated, can lead to Fitz-Hugh Curtis syndrome ➔ RUQ pain
– Other complications of PID include increased risk of infertility, chronic pain and ectopic pregnancy
Diagnosis:
Clinical diagnosis is made, and treatment started before test results
– 1st do pregnancy test to exclude ectopic pregnancy
– High vaginal swab and Chlamydia and Gonorrhoea tests
– Blood tests –> show raised WBC and high CRP/ESR
Management:
Doxycycline + metronidazole + single-dose IM ceftriaxone or Ofloxacin + metronidazole
– If severe –> start with doxycycline + IV metronidazole + IV ceftriaxone
Sources
2. https://cks.nice.org.uk/incontinence-urinary-in-women#!management


