Lower limb neurological examination
Click the button to download our free OSCE Book
Key Message
In a neurological exam, the key aspect of the exam is to work out where the nerve lesion is occuring. There are mainly 4 locations of lesion, each which give a particular pattern of clinical signs. Understanding these patterns will help you ace the exam each time and help to understand why the patient has particular symptoms. The 4 main types of presentations you are likely to see in your exams are:
| UMN | LMN | Parkinson’s | Cerebellar | |
| Tone | Up | Down | Up | Normal |
| Power | Low | Low | Normal/Low | Low |
| Reflexes | Brisk | Reduced | Normal | Normal |
| Coordination | Normal | Normal | Normal | Poor |
| Sensation | Variable | Variable | Normal | Normal |
Introduction
- Wash Your hands
- Introduce yourself by name and Role
- Check the patient’s identity – name and Date of Birth
- Explain the procedure – why you need to do it and what does it involve
- Ask for consent
- Expose the patient appropriately
- Check if the patient is currently in any pain
- Ask if they are right or left-handed
How to Introduce Yourself
“Good morning, my name is .. and I am a medical student. Can I just check your name and date of birth?
I have been asked to do an examination of the nerves in your legs today. This will involve asking you to walk and then testing the movement and sensation of your legs. Is that ok?
– For the purposes of this examination would you mind removing your gown but keeping your underwear on?
– Before I start, can I just check whether you are in any pain?
– And can I ask, are you right or left handed?”
Bedside Inspection
- Observe the patient: Patient is A – Alert B – (normal) Body habitus C – Comfortable at rest
- Observe the surroundings: mobility aids (wheelchair, walking stick), NG tube
Gait and Screening Tests
Action: Ask patient to stand up with arms folded
Assess for:
–> Proximal Muscle Weakness. This could be due to a myopathy which leads to weakness of the main extensors of the trunk, leading to an inability to stand from a seated position.
Action: Ask the patient to walk to the end of the room, turn around and then walk back.
Assess for:
–> Smoothness: Is there any disruption to the normal gait cycle such as abnormalities in toe-off or heel strike?
–> Symmetry: Is the gait symmetrical on both sides? Asymmetry of the gait could be caused by problems such as leg-length discrepancy, fixed flexion deformity, or pain on one side which reduces full extension and weight bearing on that side.
–> Step Height: A damage to the common fibular nerve for example leads to a foot-drop on the affected side. This means the patient will not be able to dorsiflex which gives them a high step height to compensate.

Types of Gait
The gait cycle is made up of 6 phases.
- Heel-strike: this is when the heel first touches the floor.
- Foot flat: here the weight is transferred onto the leg as the foot is all in contact with the floor.
- Mid-stance: the weight is aligned and balanced on this leg.
- Heel-off: Here the heel lifts off as you start to transfer weight onto the other leg.
- Toe-off: this is when the toes finally lift off the floor
- Swing: the foot swings forward until the heel comes back in contact with the ground restarting the cycle.
a) Antalgic gait – A type of gait where the stance phase is abnormally shortened to reduce time on that foot. It looks like a limp –> Implies pain in that leg
b) Waddling gait – This is due to weakness of the proximal muscles of pelvis which causes weakness of gluteus muscles. Patient moves upper body forwards and drags lower leg forward.
c) Spastic gait – this is described as a swinging gait where the patient swings his leg round as it is hyperextended. This is seen in UMN lesions such as stroke
d) High-stepping gait – This is due to damage of the deep branch of the common fibular nerve which leads to foot-drop due to loss of dorsiflexion. This means the patient has a high step in order to compensate.
e) Trendelenburg Gait – this leads to dropping of the pelvis on the contralateral side when you are walking. It is due to damage to the gluteus medius on the supported side –> indicates a lesion of the superior gluteal nerve
f) Parkinson gait – shuffling steps with a stooped over posture. The patient will shuffle forward with lack of arm swing. They will need many small steps to turn around. The gait can appear rushed, and then also freeze.
g) Ataxic gait – this is a gait that looks like someone has just learnt how to walk. The person will watch their feet and walk like a spaceman with a wise stance so that they do not fall over. It is associated with an ataxia, usually due to cerebellar dysfunction.
Action: Ask patient to do walk touching their heel to their toe.
Assess for:
–> Lack of coordination. This is a test which requires the individual to be able to coordinate different muscle groups. If impaired, it may signal a cerebellar lesion.
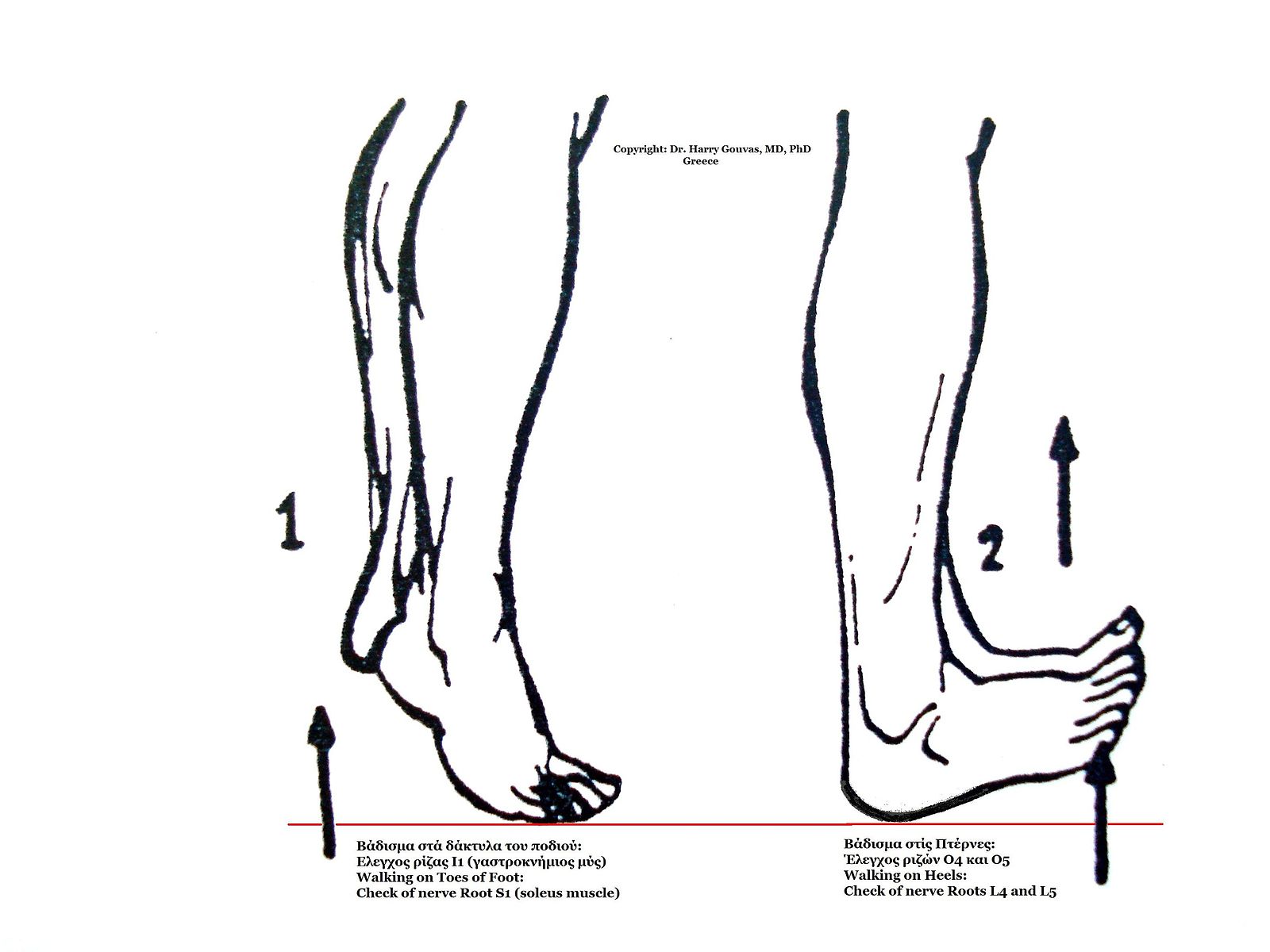
Action: Ask the patient to stand on their toes and hold their position.
– After this ask them to stand on their heels.
Assess for:
–> Muscular weakness – these are two actions which screen for power in various muscle groups.
– Failure to plantarflex –> suggests damage to sciatic nerve, due to impairment of S1
– Problems with dorsiflex –> this suggests a footdrop due to damage of L4/L5
Balance is coordinated by the cerebellum which receives input from 3 places. Proprioception, vestibular system and vision. You need at least 2 to keep balance. Romberg’s test removes vision leaving the other two, so you can identify whether the issue is with one of these, or the cerebellum itself which cannot integrate the various stimuli.
Action – Perform Romberg’s test of balance.
a. Position yourself within arms reach of the patient to allow you to intervene should they begin to fall.
b. Ask the patient to put their feet together and keep their arms by their sides (be aware that patients with truncal ataxia may struggle to do this, however, this type of unsteadiness is not the same as a positive Romberg’s sign).
c. Ask the patient to close their eyes.
Assess for:
–> Balance – this is a test which can be used to assess whether there is a problem with proprioception, vestibular function or the cerebellum.
– If patient feels unsteady with eyes closed – this is a positive Romberg’s sign. This shows problem is due to sensory problem (due to proprioceptive disorder or vestibular dysfunction) as the patient feels unsteady when the visual stimulus is removed.
– If patient feels unsteady with eyes open – this is a negative Romberg’s sign. This shows problem is in the cerebellum, due to an issues with coordinating the different sensory inputs.
Inspection
Action: Ask the patient to lie down on the couch and keep their legs outstretched. Inspect the legs from all sides.
Assess for: SWIFT-PH
–> Scars: These are indicative of previous surgery or trauma to the legs
–> Wasting: This is what happens to muscles when they lose nervous innervation. It is a clinical sign which is usually associated with a lower motor neurone problem. Look especially for plantar foot wasting or dorsal foot guttering.
–> Involuntary movements: There are a variety of involuntary movements which are associated with specific nervous conditions.
a) Chorea – these are short, unwanted movements which appear in conditions like Huntington’s disease
b) Myoclonus – involuntary twitching of a muscle or a group of muscles, central nervous system disorders
c) Athetosis – slow, involuntary, writhing movements of the fingers, hands, toes. It occurs due to damage of thalamus, basal ganglia, seen in HD and hypoxia infants
d) Pseudoathetosis – abnormal writhing movements, usually of the fingers, caused by a failure proprioception – disruption of the proprioceptive pathway, from nerve to parietal cortex.
–> Fasciculations: These are tiny contractions of skeletal muscle which may look like cramping of the muscle to the naked eye. They are associated with lower motor neuron lesions
–> Tremor: These are defined as fine or course.
–> Posture: Can indicate the curvature of the spine
–> Hypertrophy: This is a clinical sign which is associated with upper motor neuron lesions.
Tone
Testing the tone is an essential part in helping to distinguish whether the nerve lesion is upper or lower. Upper motor neurone lesions typically give hypertonia, whereas lower motor neurone lesions give reduced muscle tone.
There are 3 main actions that we use to assess tone in the legs.
Action: With the patient lying on the examination couch, place one hand above and the second hand below the knee. Roll each leg from side to side whilst asking the patient to fully relax.
Assess for:
–> Tone of the leg muscles. The best way to do this is to see if the foot swings from side to side as you roll the leg. The foot should swing with the momentum – if it is rigid, this indicated hypertonia.
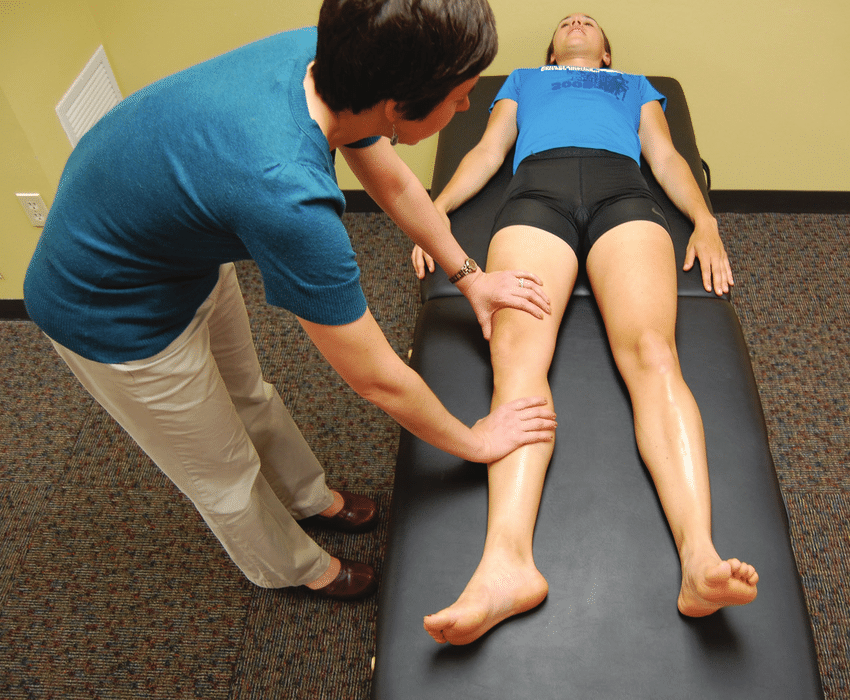
Action: Lift each knee briskly off the bed (warning the patient first) and observe the movement of the leg.
Assess for:
–> Spasticity: This is when the muscle jerks back when it is stimulated. In patients with normal tone, the knee should rise whilst the heel remains in contact with the bed. However in hypertonia, after raising the knee, the patient might involuntary kick their heel up due to increased tone.
Action: With the patient’s leg extended, hold the sole of their foot with your right hand whilst supporting the leg with your left hand.
– Rapidly dorsiflex and partially evert the foot to stretch the gastrocnemius muscle.
– Hold the foot in this position and see if you can feel the muscle contracting and relaxing in a rhythmic fashion.
Assess for:
–> Clonus: This is a series of involuntary rhythmic muscular contractions and relaxations that occurs when a muscle is stimulated. It occurs in upper motor neurone lesions. If you detect >5 clonus beats then this is a pathological finding.

Power
Many nerve conditions lead to muscular weakness. This can be tested by assessing the power of the muscles. You want to see if the weakness is widespread or has a specific pattern. This can help localise where the nerve lesion is. To test power, it is important that you stabilise and isolate the relevant joint and compare side to side.
For each joint, compare each side to ensure you are testing like for like. You will test the power by providing resistance and asking the patient to push against you.
We measure the power using the MRC scale (0-5):
MRC Power Scale
0= No contraction at all
1 = Flicker of muscle contraction
2 = Can move muscle but not against gravity
3 = Can move muscle against gravity
4 = Movement against gravity and some resistance, but a little weakness remains
5 = Normal power, full movement against gravity and resistance
Hip
Action: Ask patient to lift their legs straight up off the bed. Hold the contralateral hip to stablise the hip joint. Test one leg at a time
Assess for:
–> Hip Flexion: Once the leg is off the bed, see if they can keep it up as you try to push their leg down.
– Tests ileopsoas muscle.
– Nerve roots = L2, L3
–> Hip extension: Place your hand under their thigh, and say push against my hand.
– Tests by Gluteal muscles.
– Nerve roots = L4,L5

KNEE
Action: Ask the patient to bend both their knees so their feet are on the bed flat. Test one side at a time.
Assess for:
–> Knee Extension: Ask the patient to try straighten their leg against your hand.
– Tests quadriceps
– Nerve roots = L3, L4 (femoral nerve)
–> Knee Flexion: Ask the patient to stop you from pulling their leg straight.
– Tests hamstrings
– Nerve roots = L5,S1 (sciatic nerve)

ANKLE
Action: Ask the patient to keep their legs outstretched so you can assess their ankles.
Assess for:
–> Plantarflexion: Place your hand on the sole of the patient’s foot and ask them to push down against this.
– Tests soleus and gastrocnemius
– Nerve roots = S1, S2 (sciatic nerve)
–-> Dorsiflexion: Place your hand on the dorsal aspect of their patient’s foot and ask them to push up against your hand.
– Tests tibialis anterior
– Nerve roots = L4, L5
Hallux
Action: Ask the patient to keep their legs outstretched so you can assess their big toe.
Assess for:
–> Toe extension: Ask the patient to extend their big toe as you apply resistance from the top
– Tests extensor hallucis longus
– Nerve root = L5, S1 (common peroneal nerve)
–-> Toe flexion: Ask the patient to push down with their big toe against your thumb below
– Tests Flexor hallucis longus
– Nerve root = S2,S3 (tibial nerve)
Reflexes
This is a good way to distinguish between upper and lower motor neurone lesions. Remember, UMN give hyperreflexia whereas LMN will produce hyporeflexia. If you cannot elicit a reflex you can ask the patient to clench their teeth. This is known as a Jendrassik manouveure and it helps to accentuate the reflex.
Knee Jerk Reflex
Action: Test the knee jerk reflex in both legs:
a. Place your left arm under the patient’s knee so you are supporting their legs weight on your arm.
b. Ask the patient to completely relax their leg.
c. Using a tendon hammer, tap the patella tendon just above the tibial tuberosity
d. You should find that the knee extends and kicks out causing a knee-jerk
Assess for:
–> Knee-Jerk: This is caused by a reflex pathway due to stretch of the muscle. Look for absence or excessive amplitude of this reflex.
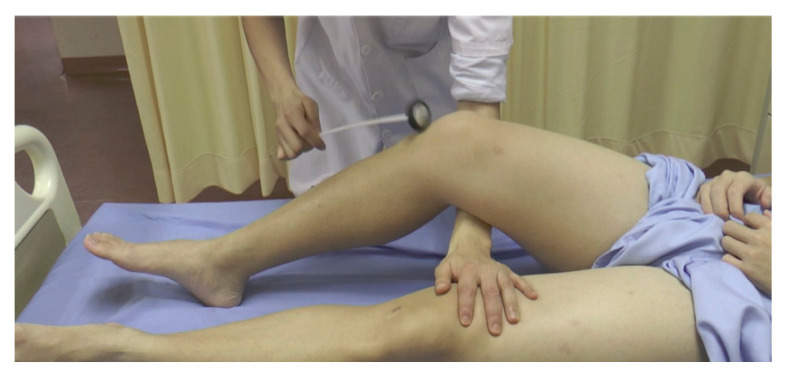
Ankle Reflex
Action: Test for the ankle-jerk reflex (S1) in both of the patient’s legs, one by one
a. Ask the patient to bring their knee up and then drop their leg to the side. This will bend their leg as if they are making a frog’s leg on that side. The hip is abducted, knee flexed and the ankle held in dorsiflexion.
b. Keep the ankle slightly dorsiflexed so their achilles tendon is stretched
c. Using the tendon hammer, tap the Achille’s tendon
d. See if you can feel a reflex contraction in the gastrocnemius muscle causing the foot to plantarflex.
Assess for:
–> Hypo/hyperreflexia: LMN associated with hypo and UMN associated with hyper.

Babinski Reflex
The plantar reflex is a reflex elicited when the sole of the foot is stimulated with a blunt instrument. The reflex can take one of two forms. In healthy adults, the plantar reflex causes a downward response of the hallux. However, in upper motor neurone lesions, the opposite happens and your toe will curl upwards.
Action: Test the the plantar reflex (L5, S1) in each of the patient’s feet.
a. Explain to the patient that you will use a pointed end to press along the sole of their foot and it may feel uncomfortable.
b. Hold the foot with your left hand
c. Start at the base and then run the pointed end of the object along the lateral aspect of the foot to just under the toes and then across medially
d. Observe for the motion of the hallux.
Assess for:
–> Babinski Sign:
– If the hallux and other toes flex downwards, this is a normal result
– If the hallux extends up, this is known as a positive Babinksi sign. It is associated with upper motor neurone lesions.

Coordination
Coordination is an important test as it assess the ability of the brain to synchronise the movement of multiple muscle groups. This is usually controlled by the cerebellum. Therefore, an inability to coordinate the muscles usually points to cerebellar ataxia.
N.B. Do keep in mind that patients may not be able to do these movements due to weakness, pain, or an inability to understand your instructions.
Action: Perform the heel skin test:
a. Ask the patient to place their right heel on their left knee and then slide it down their left leg
b. Then ask them to touch their foot to your hand which you are holding above their foot.
c. Then ask them to touch their right heel to their left knee again restarting the cycle.
d. Now ask them to repeat this sequence of movements in a smooth motion up to 5 times.
e. Repeat the assessment with the other side.
Assess for:
–> Dysmetria: This word means a lack of coordination of muscle groups. Whilst the patient may be able to do the movement really slowly, the key is to assess whether they can do it in a smooth manner, else they may have cerebellar dysfunction.

Sensation
Testing for sensation is essential as it can help distinguish whether the condition solely affects motor nerves or whether sensation is also affected. This gives you an idea of the underlying diagnosis e.g. motor neurone disease does not affect sensation.
With sensation, you want to characterise the distribution of sensory changes and compare side to side.
You will also want to test different modalities, including light touch, pain and temperature.
LIGHT TOUCH
Action: Test the sense of light touch using a piece of cotton wool (or lightly tapping)
a. Ask the patient to close their eyes and brush the cotton wool on their sternum. Explain that this is what it will feel like
b. Tell the patient that you will tap them lightly. Ask them to say “Yes” when they can feel something.
c. Brush the cotton wool in the following areas, which are supplied by particular nerves. For each dermatome, compare side by side, and ask “Does it feel the same on both sides”
| T12 – ASIS | L4 – medial leg |
| L1 – high pocket | L5 – dorsum of big toe |
| L2 – lateral thigh | S1- sole of foot |
| L3 – medial thigh/patella | S2 – popliteal fossa |

PAIN
Pain is carried by Ad and C fibres in the spinothalamic tract.
Action: Test for the pain sensation in exactly the same way as testing for soft touch. Instead of cotton wool however, use the sharp end of a neuro-tip.
TEMPERATURE
Temperature is also carried by Ad and C fibres in the spinothalamic tract.
Action: Offer to test for the temperature sensation in exactly the same way as testing for soft touch. Instead of cotton wool however, use a cold or hot stimulus.
– It is unlikely you will be required to test for temperature in an OSCE, but you should still offer the test for bonus points.
Vibration
Vibration and pressure are transmitted by large Aa and Ab fibres which travel in the dorsal column of the spinal cord. They are affected by many conditions, including diabetes.
Action: Test for the sense of vibration using a tuning fork.
a. Tap the tuning fork so it vibrates
b. Ask the patient to close their eyes and place the end of the tuning fork on their sternum, to show them what it will feel like.
c. Tell them you will now place it elsewhere and that they need to tell you when they can feel it vibrating and when it stops.
d. Tap the tuning fork and place the end on the distal interphalangeal joint of the big toe.
e. See if the patient can correctly tell you when it vibrates and when the vibration has stopped.
Assess for:
–> Sense of vibration: If they answer you correctly, you do not need to continue.
– If they cannot answer at the big toe, work more proximal repeating the test at the metatarsophalangeal joint, then ankle and then knee.
Proprioception
Proprioception is the sense of where you limbs are in space. It relied on joint fibres which gives sensory input to the brain allowing the brain to form an image of the body in space. It is affected by neuropathies which affect nerve fibres which travel in the dorsal column of the spinal cord.
Action:
a. Hold the patient’s big toe by the distal phalangeal joint on both sides (not compressing the nail bed).
b. With the patient watching , move the toe “up” and then “down” so the patient understands which way is which.
c. Ask the patient to close their eyes
d. Move the toe up and down, each time asking the patient which way you are moving it.
Assess for:
–> Sense of proprioception: If they answer you correctly, you do not need to continue.
– If they cannot answer at the big toe, work more proximal repeating the test at the metatarsophalangeal joint, then ankle and then knee.
Thank the patient and wash your hands again!
On Completion
“To complete the examination, I would do a number of steps…”
Bedside
- (History) Take a full history including effects on life and functional status
- (Observations) Full set of observations
- (Corresponding examination) Conduct a neurological assessment of upper limbs and cranial nerves. Offer a full assessment of cognitive and higher order functions like speech
Bloods – FBC, inflammatory markers, renal profile etc.
Imaging – CT scan/MRI scan (if indicated)
Special Tests – Nerve conduction studies/EMG (if indicated)
Sources
Gait Cycle – Ducky2315, CC BY-SA 3.0 <https://creativecommons.org/licenses/by-sa/3.0>, via Wikimedia Commons
Standing on toes – Σχέδιο: Δρ. Χαράλαμπος Γκούβας (Draw: Dr. Harry Gouvas, MD, PhD) (Harrygouvas), CC BY-SA 3.0 <https://creativecommons.org/licenses/by-sa/3.0>, via Wikimedia Commons
Ankle Clonus – https://healthjade.net/clonus/
Straight Leg Raises – BruceBlaus, CC BY-SA 4.0 <https://creativecommons.org/licenses/by-sa/4.0>, via Wikimedia Commons
Knee Flexion – Fruityfruit, CC BY-SA 3.0 <https://creativecommons.org/licenses/by-sa/3.0>, via Wikimedia Commons
Knee Reflex – Malays J Med Sci. 2021 Apr; 28(2): 48–62. Published online 2021 Apr 21. doi: 10.21315/mjms2021.28.2.5. Copyright © Penerbit Universiti Sains Malaysia, 2021. This work is licensed under the terms of the Creative Commons Attribution (CC BY) (http://creativecommons.org/licenses/by/4.0/).
Ankle Reflex – Malays J Med Sci. 2021 Apr; 28(2): 48–62. Published online 2021 Apr 21. doi: 10.21315/mjms2021.28.2.5. Copyright © Penerbit Universiti Sains Malaysia, 2021. This work is licensed under the terms of the Creative Commons Attribution (CC BY) (http://creativecommons.org/licenses/by/4.0/).
Plantar Reflex – derivative work: Roxbury-de (talk)Objaw_babinskiego.png: The original uploader was Malki at Polish Wikipedia., CC BY-SA 2.5 <https://creativecommons.org/licenses/by-sa/2.5>, via Wikimedia Commons
Heel Shin Test – https://www.researchgate.net/profile/Abilo-Tadesse/publication/334697259/figure/fig25/AS:784835681456136@1564130816979/Performing-Heel-to-Shin-test.jpg
Dermatomes – Anatomy, Skin, Dermatomes Copyright © 2021, StatPearls Publishing LLC. Public Domain
Disclaimer



