Abdominal Examination
Click the button to download our free OSCE Book
Introduction
- Wash Your hands
- Introduce yourself by name and Role
- Check the patient’s identity – name and Date of Birth
- Explain the procedure – why you need to do it and what does it involve
- Ask for consent
- Expose the patient appropriately
- Check if the patient is currently in any pain
How to Introduce Yourself
“Good morning, my name is .. and I am a medical student. Can I just check your name and date of birth?
I have been asked to do an abdominal examination on you, which would involve me having a look at your hands, face and chest, and then having a feel and listen to your tummy. Is that ok?
– For the purposes of this examination I’m just going to position the bed at 45 degrees. Later in the exam, I will need to place the bed flat.
– Would you mind removing your shirt for me please?
– And can I just check whether you are in any pain?”
Bedside Inspection
- Observe the patient by standing at the end of the bed.
- Comment on whether the patient is ABC:
A – Alert B – (normal) Body habitus C – Comfortable at rest
- Observe the surroundings and comment of whether you can see any “paraphernalia of cardiovascular disease”:
This is a description of the objects or items around a patient’s bedside that will give you an idea into the condition that they might have. It is important to highlight this to the examiner as this can give you many clues about the patient’s underlying diagnosis. Things to look for include:
- Oxygen – is the patient currently on oxygen or room air, and what is the flow rate?
- Inhalers – does the patient have underlying respiratory disease?
- Medication – can you see any medication on the patient’s bedside e.g. beta-blockers?
- Test results – are there any investigation results like ECGs lying around the patient’s bedside.
- Fluid chart – this gives you an idea if they are fluid overloaded.
- Pillows – this is a useful marker of the level of heart failure as it shows that the patient might be suffering from orthopnea.
- Mobility aids – gives an idea about the functional status of the patient.
Hands
Action:
Ask the Patient to put the nails of their index fingers against each other. You will be looking to see if you can detect a small rhomboid shaped window (Schamroth’s window).
Assess for:
–> Finger clubbing: this is a term which describes swelling of the distal end of the fingers which leads to loss of the angle between the nail bed and the nail. It is associated with Congenital heart disease, Infective endocarditis, Atrial Myxoma, Eisenmenger syndrome.
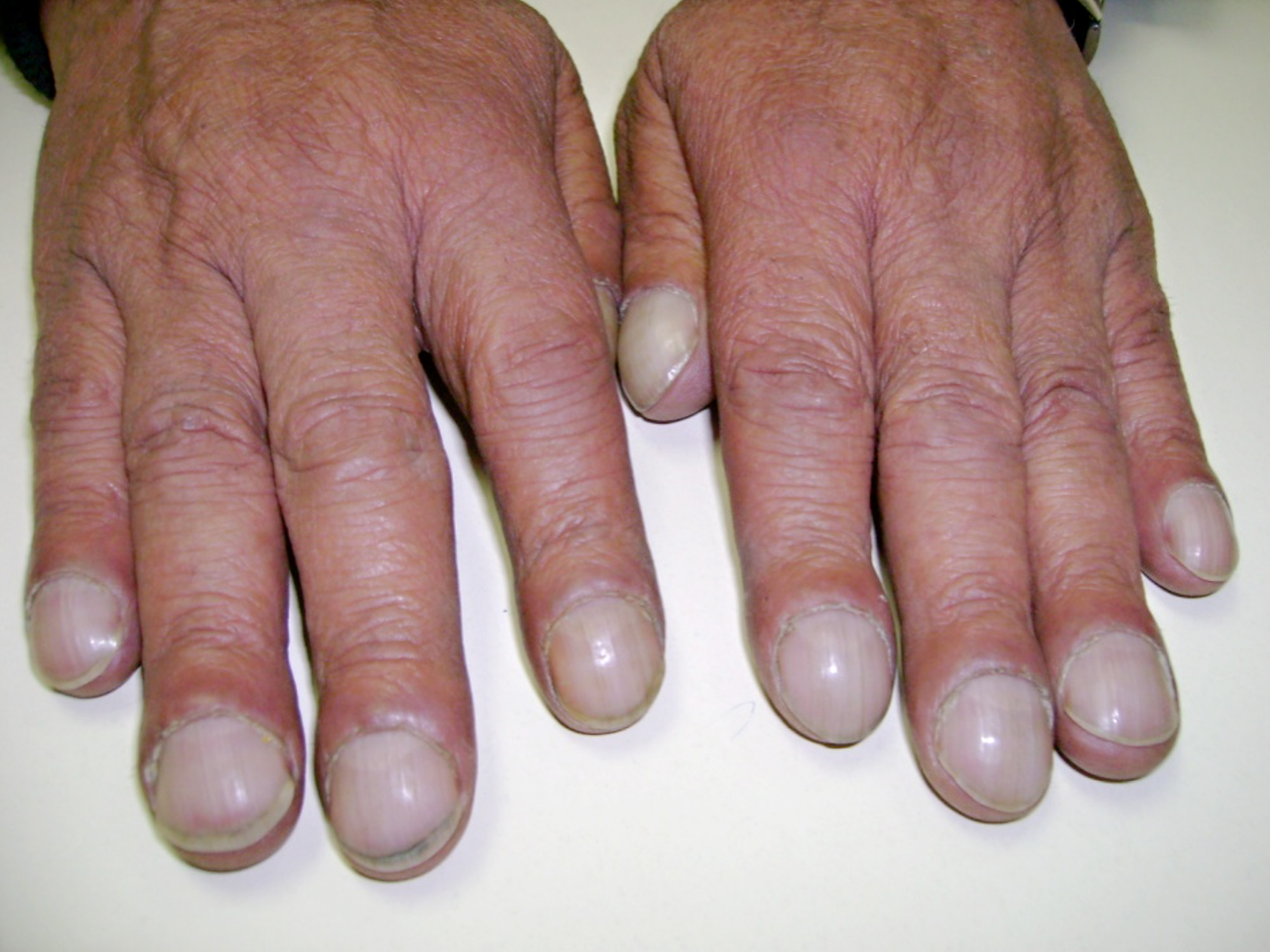
Action:
Ask the Patient to put their hands outstretched. Using the back of your hands, feel down from their forearms to feel the temperature:
Assess for:
–> Cold peripheries: This is a sign of poor peripheral circulation. This is a common sign of shock and so may occur in hypovolaemia when the arterioles are vasoconstricted to reduce blood supply to the extremities.
Action: Look closely at the back of the patient’s hands.
Assess for:
–> Extensor Tendon Xanthomata: These are small non-tender lumps of cholesterol that can be found of the tendons of the extensor muscles of the wrist and palms. They are seen in hyperlipidaemia.
–> Peripheral Cyanosis: This is a blue discolouration of the nails and fingers which is indicative of peripheral ischaemia. It shows the patient is peripherally not perfusing well which can be seen in shock or hypothermia.
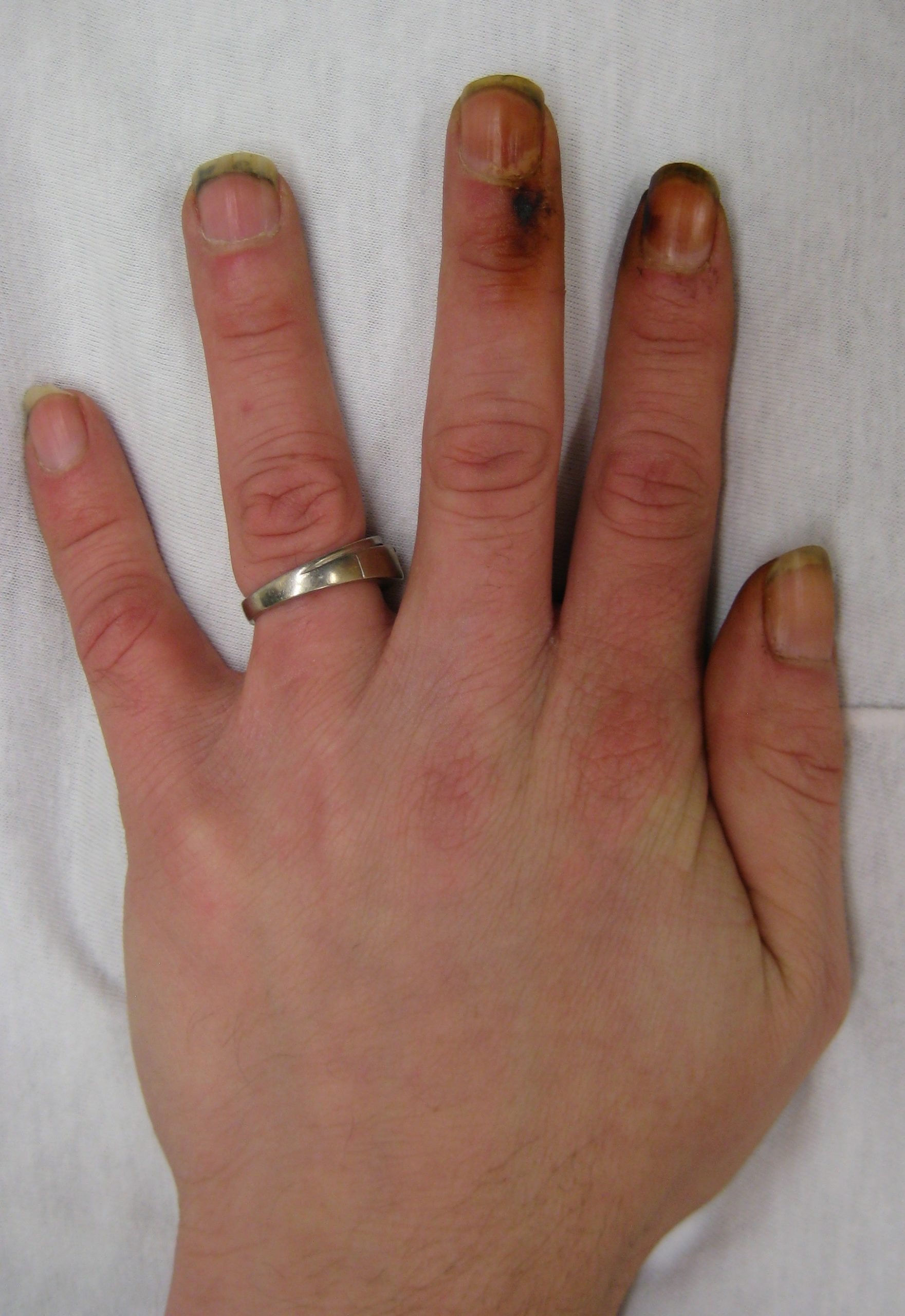
–> Tar staining: This is a black/brown staining of the nails and fingers which is seen in chronic smokers.
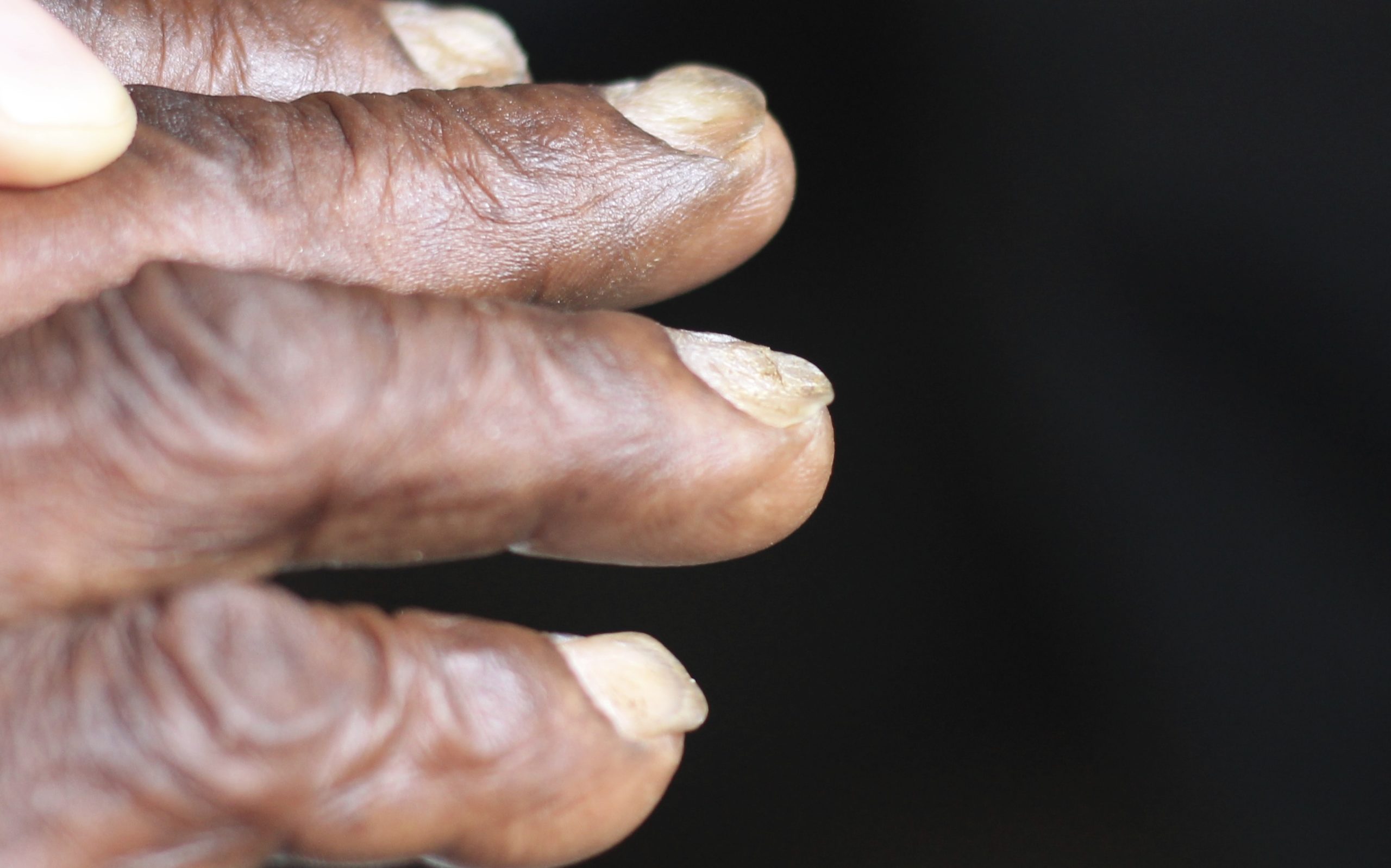
–> Koilonychia: These are spoon-shaped nails which are seen in iron-deficieny anaemia.
–> Leuconychia: This is a medical term for white discolouration appearing on nails. It is associated with liver disease.
Action: Pinch the patient’s fingernail for 5 seconds and then release. Measure the capillary refill time.
Assess for:
–> Capillary refill time: This is the time taken for the capillaries to refill after a sustained period of pressure. Apply 5 seconds of pressure to the distal phalanx of the index finger and then release. Count how many seconds it taken to go red (re-vascularise). If >2 seconds, this shows poor peripheral circulation which could be a sign of shock.
Action: Ask the patient to turn their hands over and then look at the palmar surface of their hands:
Assess for:
–> Dupuytren’s contracture: This is an abnormal thickening of the skin in the palm of your hand at the base of your fingers. In Dupuytren’s disease, the fascia overlying the tendon becomes thicker and forms cords and bumps. It is associated with excessive alcohol use, increasing age, male gender and diabetes.
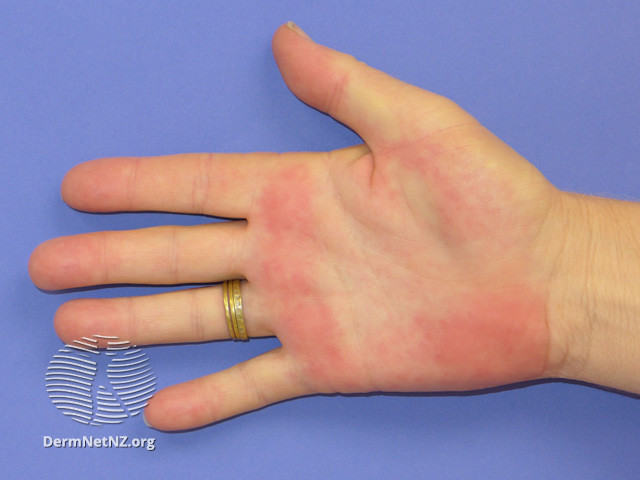
–> Palmar erythema: This is a redness involving the heel of the palm that can be associated with chronic liver disease (it can also be a normal finding in pregnancy).
–> Pigmentation of palmar creases: This is darkening of the creases in the palm of the hand, which is associated with Addison’s disease.
Action: Ask the patient to hold both their arms out and cock their wrists back. Ask them to keep their eyes closed and see if they can keep their hands in this position.
Assess for:
–> Asterixis: This is in ability of the patient to keep their hands cocked back. You will notice a course tremor where the hands may flap forward. This is a sign of hepatic encephalopathy and is seen in liver failure.
Wrists
Action: Feel for the Radial Pulse on one side and measure the radial pulse for 15 seconds
Assess for:
–> Rate (bpm), rhythm (regular, regularly irregular, irregularly irregular) and character (thready, bounding):
What the Radial Pulse Tells You
The radial pulse gives you a lot of information about the state of the cardiovascular system. There are 3 main variables to talk about when measuring the radial pulse:
1. Rate:
– A rate of <60bpm is considered bradycardia
– A rate of >100bpm is considered tachycardia
2. Rhythm: There are 3 main rythms to talk about:
– Regular – this will most likely be due to sinus rhythm, however you can get this in ventricular tachycardia
– Regularly irregular – this will most likely be due to a form of heart block
– Irregularly irregular – this is one not to miss and is most likely due to atrial fibrillation.
3. Character – this is gives you an indication of the strength of the impulse. It can be:
– Thready – can be seen if the BP is low such as in shock if the patient is peripherally shutting down
– Bounding – seen in CO2 retention.
Action: Closely inspect the arms for a variety of features.
Assess for:
–> Renal Fistulae: This is an arteriovenous connection which is used for dialysis. If you spot this, it is likely the patient has end stage renal failure.
–> Track Marks: This is a sign of IV drug use and is a risk factor for developing blood transmitted conditions like Hepatitis B and C
Action: At this point, state that you would mention the blood pressure in both arms.
Head
Action: Ask the patient to pull their eyelid down with their finger and look up.
Assess for:
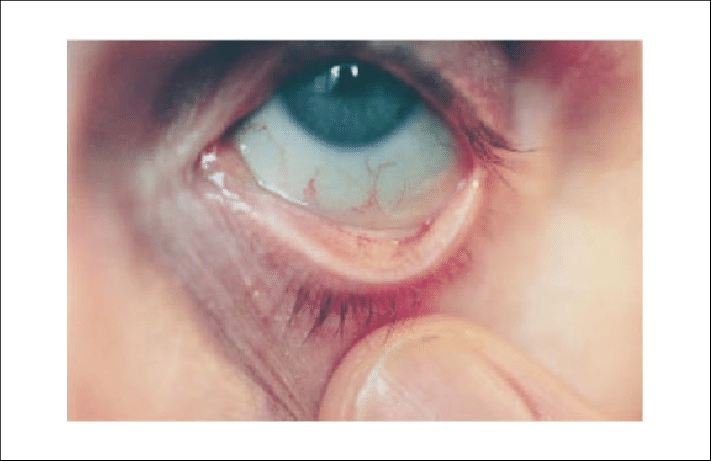
–> Conjunctival Pallor: This is a paleness of the conjunctiva which is a sign of anaemia
Action: Ask the patient to relax and look at their eyes.
Assess for:
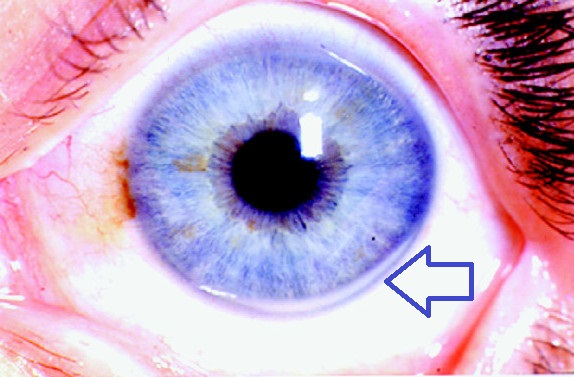
–> Corneal Arcus: This is a deposit of cholesterol, phospholipids, and triglycerides in an “arc” on either the top or bottom side of the iris, which is a sign of hypercholesterolaemia. This is a risk factor for cardiovascular disease.
–> Jaundice: This is yellowing of the sclera of the eye due to raised bilirubin in the blood. This can be due to liver disease, biliary problems or haemolytic anaemias.
–> Xanthelasma: These are yellowish-white lumps of fatty material accumulated under the skin on the inner parts of your upper and lower eyelids, which are associated with hyperlipidaemia.
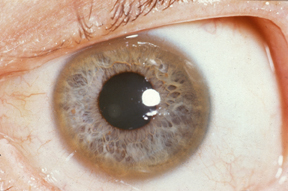
–> Keyser-Fleischer Rings: These are dark brown rings around the iris which are caused by copper deposition. This sign is characteristic of Wilson’s disease.
Action: Ask the patient to open their mouth and stick their tongue out.
Assess for:
–> High arched palate: This is associated with Marfan syndrome. You may also detect aortic regurgitation or mitral valve prolapse with this syndrome.
–> Poor dentition: This is a risk factor for infective endocarditis, especially due to streptococcus viridans.
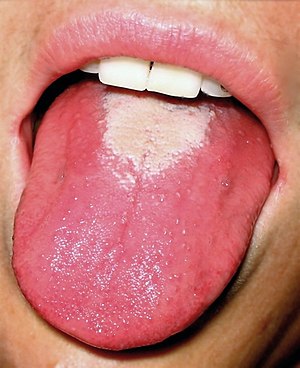
–> Glossitis: This is a beefy atrophic tongue which is seen in iron deficiency anaemia
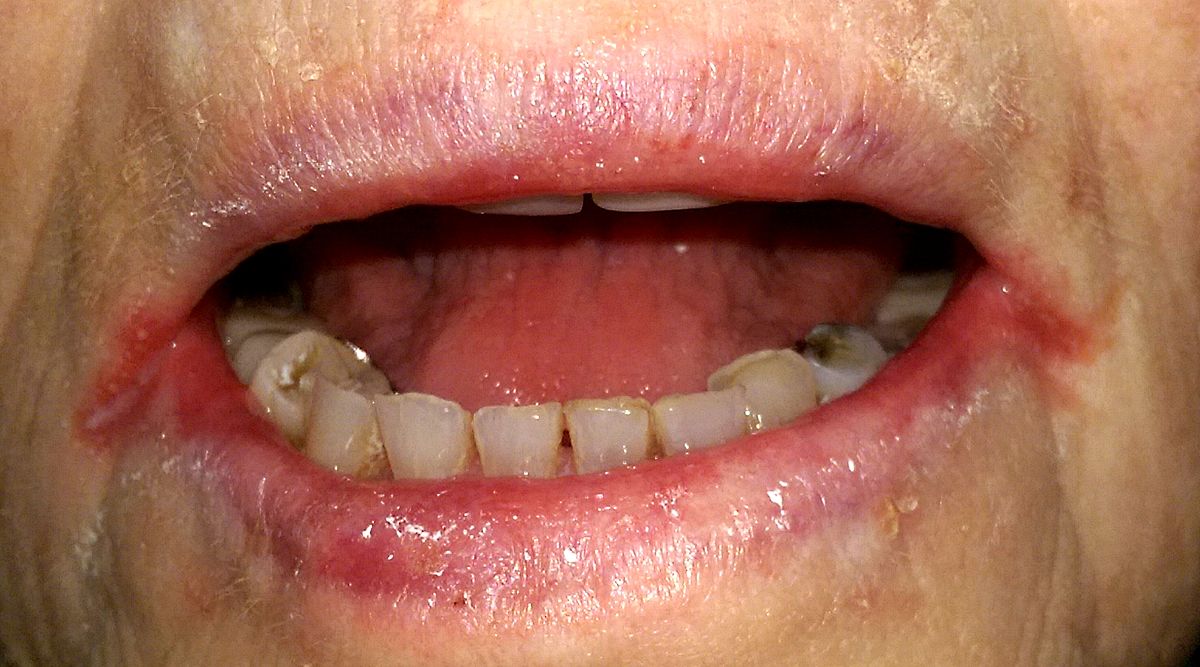
–> Angular stomatitis: This is a condition that causes red, swollen patches in the corners of your mouth where your lips meet which is associated with anaemia.
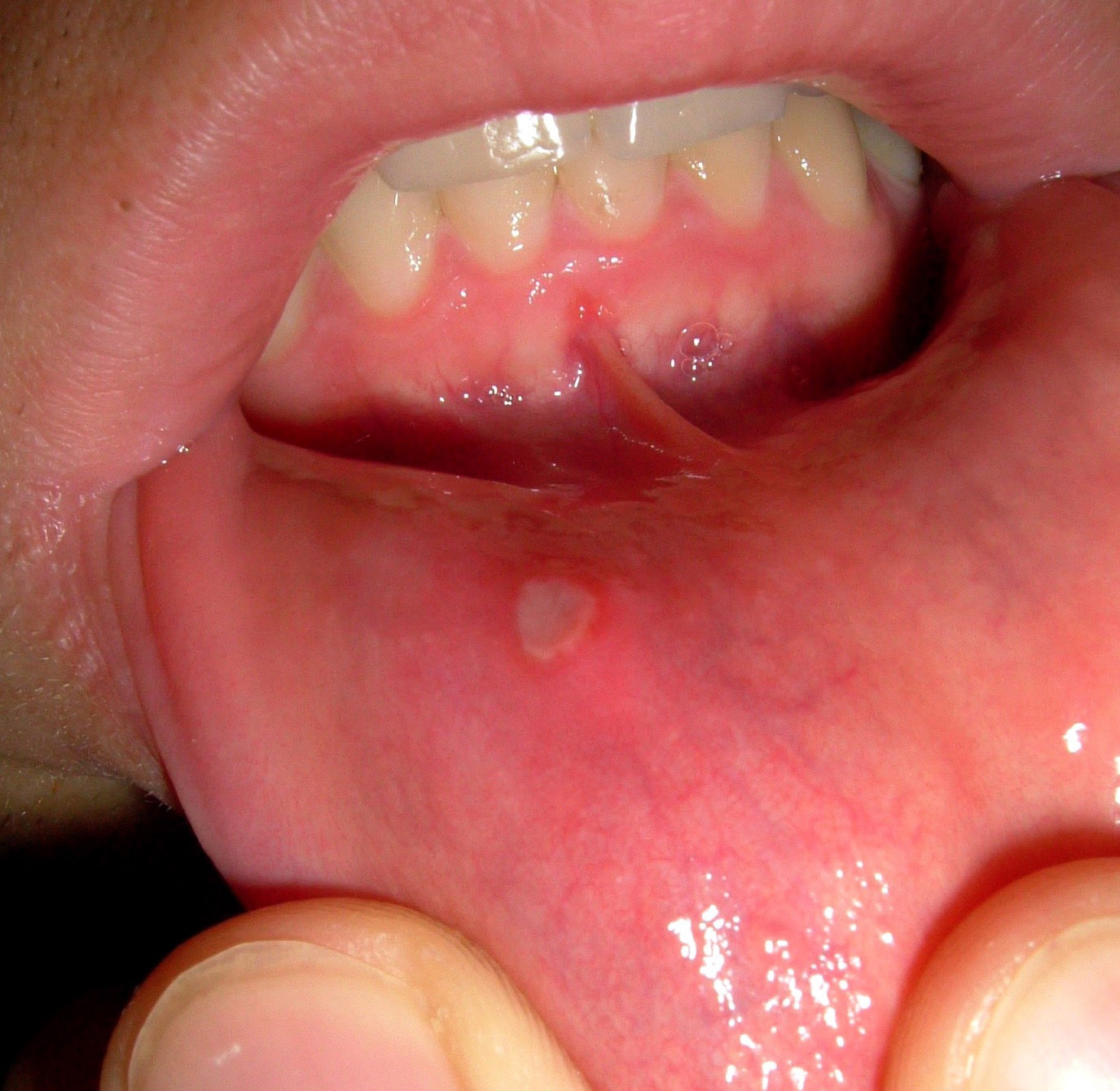
–> Mouth ulcers: Ulceration of the gums and buccal mucosa is associated with inflammatory bowel disease e.g. Crohns and ulcerative colitis.
Action: Ask the patient to touch the tip of their tongue to the roof of their palate. Observe the area under the tongue for blue discolouration.
Assess for:
–> Central cyanosis: This is a blue tinge of the mucosa in the mouth. This is a sign of hypoxia and will indicate that your patient is very unwell and needs urgent management.
Neck
Action: Ask the patient to relax back on the couch at 45 degrees and turn their head so they are looking left.
Assess for:
–> JVP: A raised JVP is suggestive of right heart failure, cardiac tamponade, tricuscpid regurgitation
How to Measure the JVP and Hepatojugular reflux
The internal jugular vein is runs from the middle part of the clavicle to the ear lobe. Its height above the sternal angle is a good indicate of jugular venous pressure, which indirectly measures central venous pressure.
– Usually the IJV should not be seen as right atrial pressure should be low. However in conditions like heart failure, this raises the pressure in the venous system so the internal jugular vein may become visible.
– Measure the height of the JVP by measuring the veritcle distance between the angle of the sternum and the pulsation point of the jugular vein. It should be less than 3cm
– If >3cm, this indicates that the JVP is raised and is due to conditions which stress right side of the heart
The hepatojugular reflux test
This is a test that you can do to make the IJV more visible by applying pressure to the liver. Pressing on the liver increases venous return to the heart as it is a very vascular organ. As it can cause pain, your examiner might not want you to perform this test but you should mention it to them anyways. To perform the test:
– Warn the patient that you will press on their liver quite firmly
– Apply pressure to the RUQ over their liver and observe the IJV for a rise
– A positive result is if there is a sustained rise in jugular venous pressure for more than 3cm.
Action: Get the patient to lean forward. Stand beside them and feel the lymph nodes around their head and neck.
– Start with the submental lymph nodes –> submandibular –> pre-auricular –> posterior auricular
– Then feel the occipital lymph nodes –> supraclavicular –> infraclavicular
Assess for:
–> Lymphadenopathy: This is tender or swollen lymph nodes. This could be a sign of cancer or a respiratory tract infection. In particular feel the left supraclavicular node. This is known as Virchow’s node and it is important as many gastric cancers metastasise here.
Chest and Back
Action: Get the patient to learn forward and make the arms like a chicken so you can view their axilla. Closely inspect the patient from all angles looking for key features of systemic disease.
Assess for:
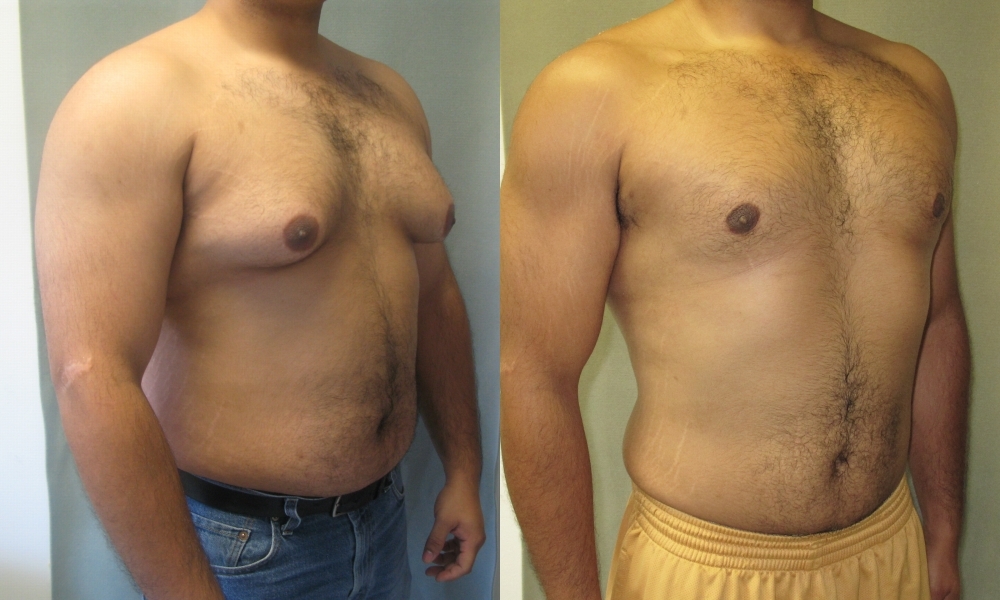
–> Gynaecomastia: This is the enlargement of male breast tissue. This is caused by raised levels of oestrogen and associated with chronic liver failure.
–> Loss of axillary hair: This is caused by raised levels of oestrogen and associated with chronic liver failure.
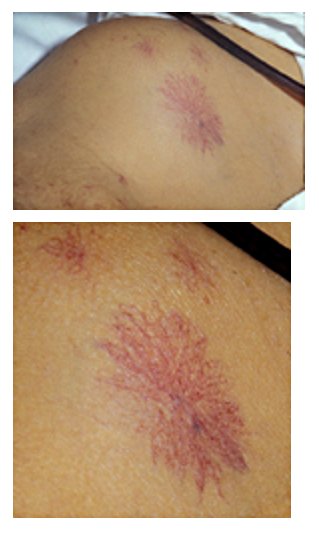
—> Spider Naevi: These are a type of telangiectasis (swollen blood vessels) found slightly beneath the skin surface, often containing a central red spot and deep reddish extensions which radiate outwards like a spider’s web or a spider’s legs. They are associated with raised oestrogen due to the COCP but also liver cirrhosis. Likely to be pathological if you can count >5.
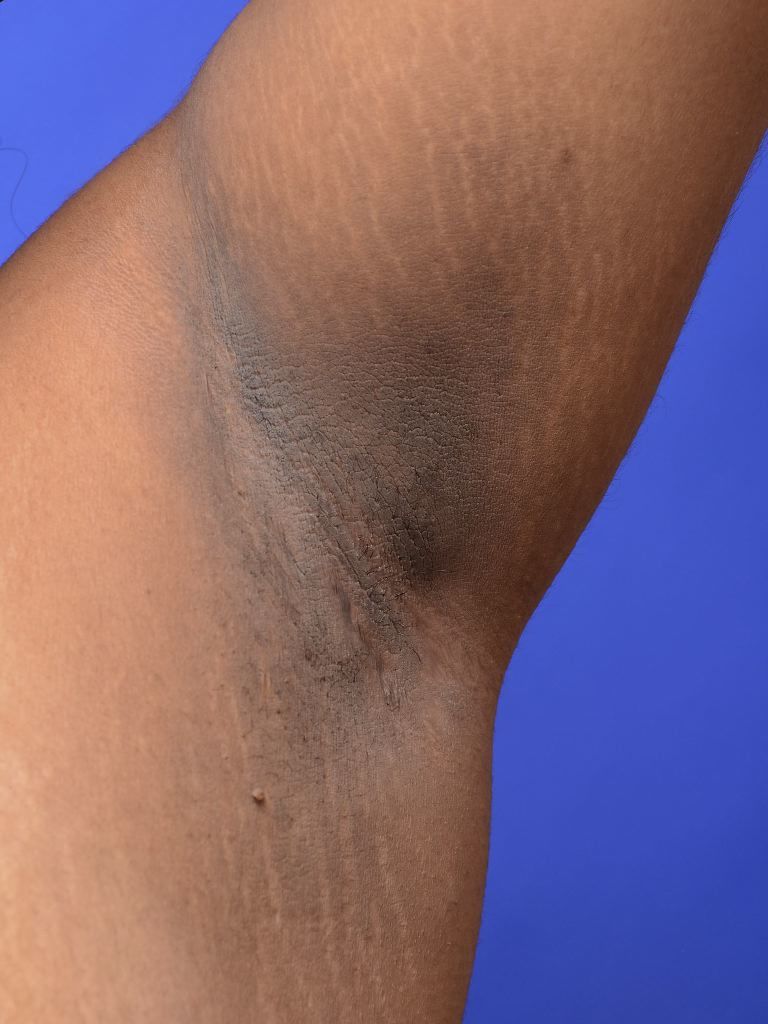
–> Acanthosis nigricans: This is darkening and thickening of the skin in the axilla. It can occur due to a variety of features but most commonly seen in diabetes but also associated with GI Malignancies.
Abdomen
INSPECTION:
Action: Lie the patient flat an expose the abdomen from the subcostal margin to just above the pubis. Closely inspect the patient for a variety of features associated with abdominal disease.
Assess for:
–> Scars: This is indicative of previous abdominal surgery.
–> Stomas: This is indicative of previous surgery to the bowel. If a stoma is present you need to comment on its site, contents, type of spout and how the skin looks around the stoma site.
–> Striaea: These are stretch marks which occur due to the over-stretching of skin.
–> Shape: Assess the abdomen to see if it is distended. This could be due to air, fat or fluid.
–> Hernias: Look for any obvious swellings. You should also formally assess this by placing your hands over the patient’s groin and asking them to cough to see if you can feel a positive cough impulse.
–> Bruising: This is a sign of intra-abdominal bleeding. Grey-Turner’s sign is bruising in the flanks (due to pancreatitis causing retroperitoneal bleeding). Cullen’s sign is bruising over umbilicus.

PALPATE
1) Action: Bend over or learn down so that you are level with the patient’s abdomen. Using one hand, lightly press over the 9 regions of the abdomen and see if you can detect any tenderness in the patient.
– It is important to look at the patient’s face so subtle clues of discomfort e.g. grimace.
Assess for:
–> Tenderness: Assess whether this is localised in a particular point or generalised across the abdomen.
–> Rebound tenderness: This is sharp pain which occurs when you press and then suddenly release pressure of the abdomen. This sign is suggestive of peritonitis.
–> Guarding: This is when the patient involuntarily tenses up their abdominal muscles as you are about to press in anticipation of pain. This clinical sign is associated with peritonitis.
–> Murphy Sign: This is when you place 2 fingers in the RUQ and pain is elicited when the patient breathes in. This is seen in cholecystitis as the inflamed gallbladder hurts when touching your fingers.
–> Rovsing sign: This is palpation of the left iliac fossa gives pain in the right iliac fossa. It is seen in acute appendicitis.
2) Action: Once you have palpated superifically, use both hands and press harder over the 9 regions. You will want to use a rolling motion with your hands so that you can feel any organs or masses underneath the skin.
Assess for:
–> Masses: Comment on the location, size, whether it is fixed or movable and the consistency.
LIVER
1) Action: Using your right hand, feel for the liver.
a. Make a L-sign with your right hand.
b. Start in the right iliac fossa. Ask the patient to take a deep breath in and push down into the RIF.
c. Try to feel a liver edge which pushes against the “L” when the patient inspires.
d. Repeat the process moving up 2cm each time until you get to the costal margin until you hit the ribs or you can palpate the liver edge.
Assess for:
–> Hepatomegaly – In healthy individuals it is unlikely you will feel the liver edge. If you do and it is more than 2cm below the costal margin this shows the liver is enlarged.
2) Action: Once you have tried palpating the liver, you can then percuss for the liver margin. Percuss up from the right iliac fossa till it becomes dull. Continue to percuss till the sound becomes resonant again meaning you are in the lungs.
Assess for:
–> Liver margins – Use the percussion to determine the liver margins. This will allow you to see if the liver is enlarged.
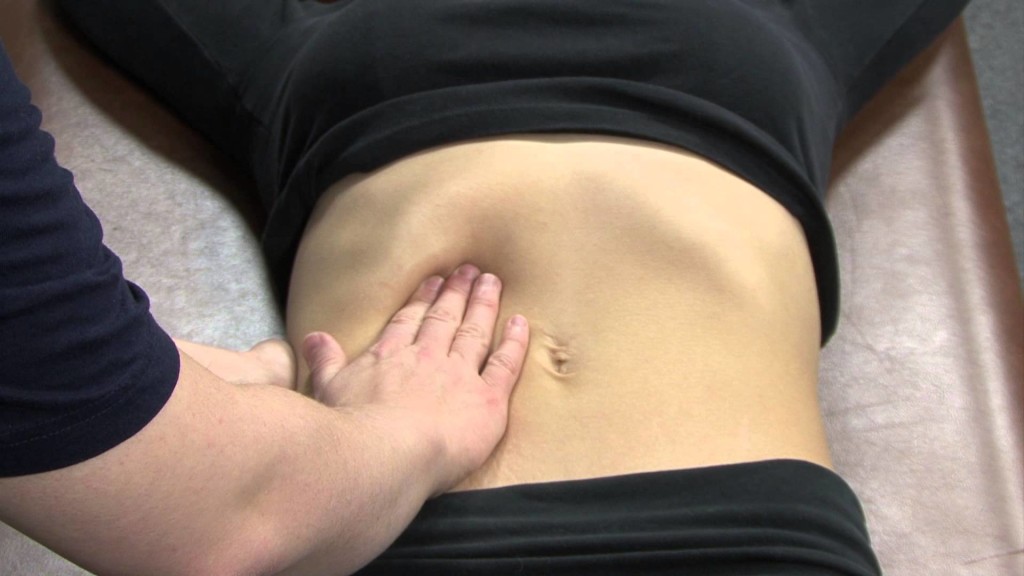
SPLEEN
1) Action: Using a similar method as for the liver, this time feel for the spleen.
a. Make an L shape and start in the Right iliac fossa
b. Move diagonally across the abdomen to the left hypochondrium
Assess for:
–> Splenomegaly – In healthy individuals you should not be able to palpate the spleen. If you can this shows the spleen is enlarged. This is seen in conditions like chronic myeloid leukhaemia, portal hypertension, glandular fever.
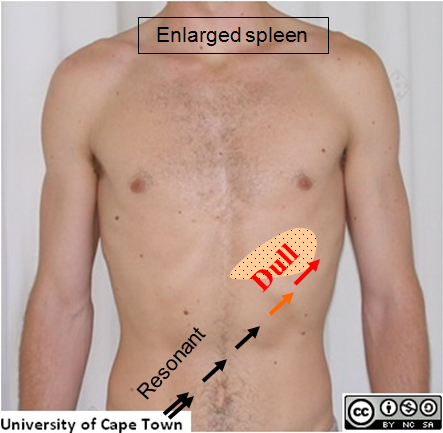
2) Action: Once you have tried palpating the spleen, you can then percuss for the splenic margin
Assess for:
–> Splenomegaly – Again you should not be able to percuss the spleen. Ability to percuss it means that it is enlarged.
KIDNEYS
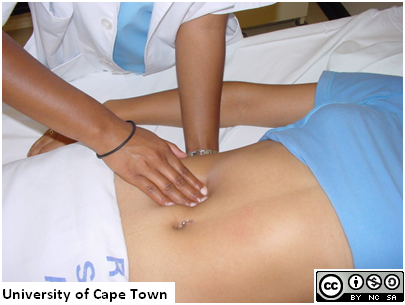
Action: Using your hands, ballot the kidneys.
a. Place your left hand under the patient’s back underneath where their right kidney is
b. Next, put your right hand over the right flank, so you are sandwiching the kidney between your hands.
c. Ask the patient to take a deep breath. As they do, press upwards with your left hand and downwards with your right hand.
d. This procedure is known as balloting the kidneys. Once you have done the right side, repeat for the left kidney.
Assess for:
–> Enlarged kidneys – Normally, you should not be able to ballot the kidneys. If you can this means they are enlarged. This could be due to a tumour, polycystic kidney disease, hydronephrosis etc.
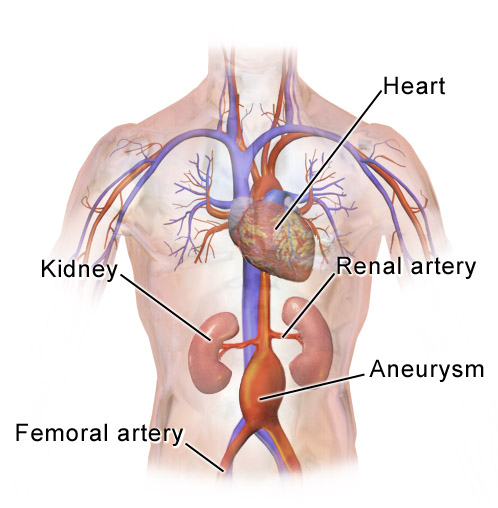
ABDOMINAL AORTIC ANEURYSM
Action: Using two hands, press down on the abdomen just superior to the umbilicus. Place both hands there and see if you can feel a movement in your fingers
Assess for:
–> Abdominal Aneurysm: This is a dilation of the abdominal aorta >50% of its original diameter.
– When feeling a normal aorta will feel pulsatile and you hands should move superiorly with each pulse
– If there is AAA, your hands will move upward and outwards, showing it is a dilated expansile mass.
BLADDER
Action: Percuss downwards from the umbilicus to the suprapubic area. If you notice a change in the resonance this could be due to the bladder.
Assess for:
–> Distended Bladder: A distended bladder which is full of liquid will be dull to percussion. Therefore, if this is heard over the suprapubic area it is likely the patient has a distended bladder. This will need to emptied either by the patient (if they can) or by the insertion of a catheter.
SHIFTING DULLNESS
Action: Perform a test of shifting dullness
a. With the patient supine, percuss over the umbilicus towards their left side. A normal abdomen should be resonant.
b. If there is ascites present, you will note the abdomen becomes dull to percussion, especially in the flank.
c. Ask the patient to roll towards you (onto their right side) and wait their 30s
d. Percuss again over their left side. If there was ascites present, it should have shifted towards the umbilicus due to gravity.
e. This means the area of the left side should be resonant.
Assess for:
–> Ascites: This is detected the presence of dullness which shifts from the flank to the midline due to gravity. This is a sign of liver failure and fluid collecting in the abdomen. It is also seen in right sided heart failure.
AUSCULTATE
Action: Using your stethoscope, have a listen to the bowel as well as the aorta and the renal arteries:
– For Bowel Sounds – Auscultate over at least 2 different areas of the abdomen for bowel sounds. Good areas include around the umbilicus and the ileocaecal valve.
– For renal arteries – place your stethoscope 2cm lateral and superior to the umbilicus
– For aorta, listen 2cm superior to the umbilicus
Assess for:
–-> Bowel sounds: These are gargling sounds that the bowel usually makes due to peristalsis. However they be absent (due to ileus) or tinkling (seen in bowel obstruction).
–> Bruits: This is an audible vascular sound which is associated with turbulent blood flow. This shows that the blood flow is being disrupted either due to a problem with the artery (e.g. aneurysm) or factors which narrow the lumen e.g. atherosclerosis.
Legs
Action: Ask the patient to keep their legs outstretched. Closely inspect their feet and legs for any signs of cardiovascular disease.
Assess for:
–> Scars: Look for vein harvesting scars for a CABG. The great saphenous vein is often used as the graft for a coronary bypass surgery, so this will indicate that the patient has ischaemic disease.
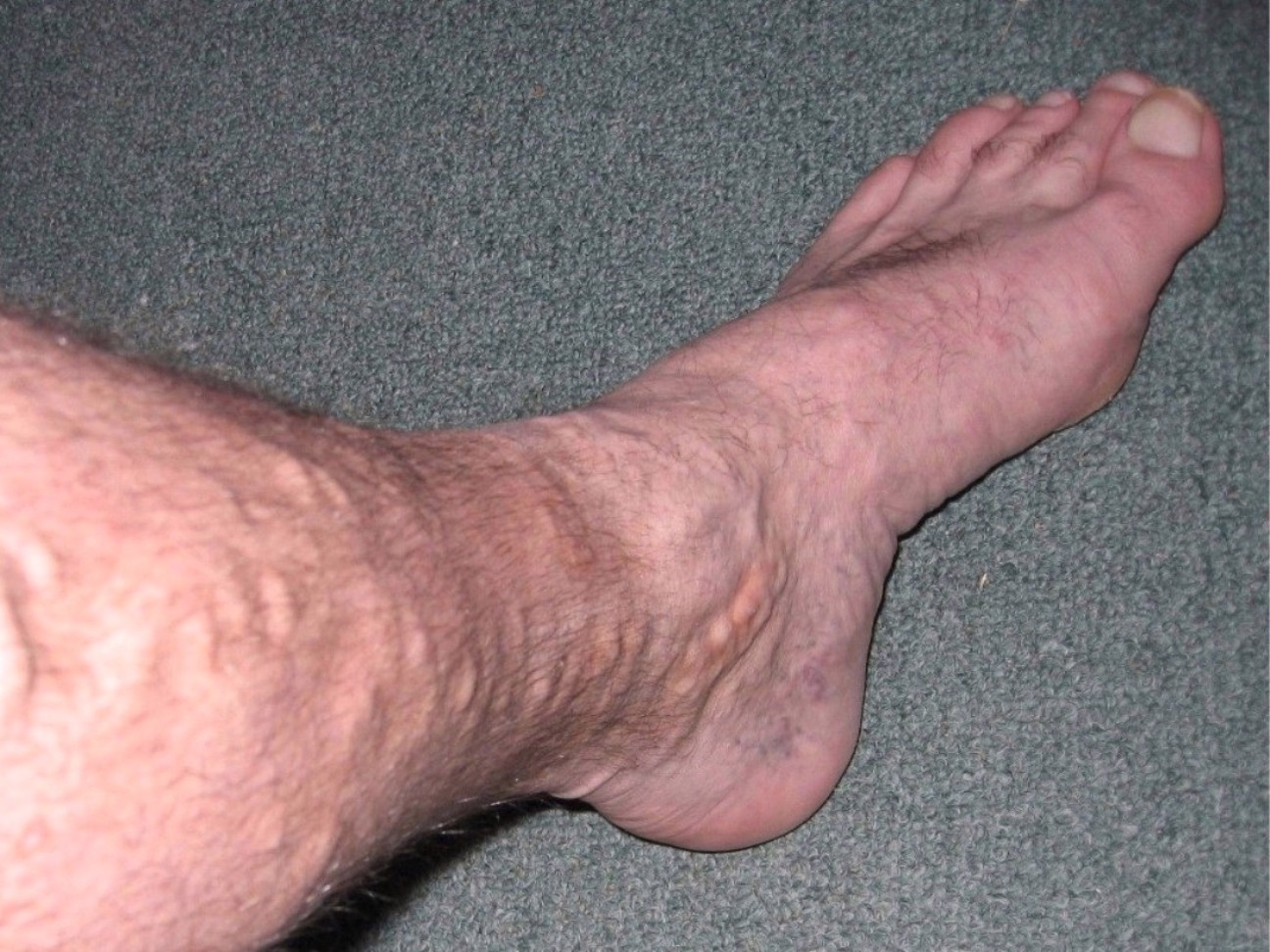
–> Varicose veins: These are dilated and tortuous veins secondary to chronic venous insufficiency
–> Calf Tenderness: A red swollen or tender calf unilaterally is a sign of a deep vein thrombosis. This needs urgent assessment with ultrasound as the patient is at high risk for a pulmonary embolus.
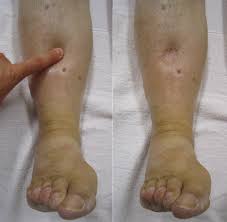
Action: Press on the medial malleolus of the patient ankles and assess if you can see/feel any sinking of the skin and whether it takes long to rise back up. If positive, see how far up the legs this oedema goes.
Assess for:
–> Pitting oedema: This is a sign that the patient is fluid overloaded. It is associated with right sided heart failure but can also be seen in conditions which reduce oncotic pressure e.g. hepatic failure.
Thank the patient and wash your hands to complete the examination!
On Completion
You must remember that the physical examination is only one part of the overall assessment of your patient. Therefore, when completing your exam, state that you would do the following in order to complete your assessment of the patient. Much of this will depend on whether you have discovered any particular findings or have an idea about the overall diagnosis. However, some essential things to talk about are:
“To complete the examination, I would do a number of steps…”
Bedside:
- (History) – Take a full history
- (Observations) Full Obs chart including blood pressure
- (Corresponding examination) Do a rectal examination, examine the hernial orifices and the external genitalia
- (Bedside tests) Take a urine dipstick
Bloods – Would take a full blood count, U&Es, LFTs and inflammatory markers
Imaging – Ultrasound abdomen (if indicated)
Special tests – CT scan (if indicated)
How to Present Your Findings
“I conducted an abdominal examination on … who seemed well and comfortable at rest.
- On inspection there were no peripheral signs or paraphernalia of abdominal disease.
- They had a pulse rate of … and their pulse was regular and character normal
- There was no cervical lymphadenopathy and the JVP was (3)cm so not raised.
- On inspection there were no scars or bruising
- The abdomen was soft and non-tender with no signs of any organomegaly
- Bowel sounds were present and there were no aortic/renal bruits
- The legs were soft with no pitting oedema
In summary, this is a normal examination.”
Sources
Finger Clubbing – Desherinka, CC BY-SA 4.0 <https://creativecommons.org/licenses/by-sa/4.0>, via Wikimedia Commons
Tar Staining – James Heilman, MD, CC BY-SA 3.0 <https://creativecommons.org/licenses/by-sa/3.0>, via Wikimedia Commons
Koilonychia – CHeitz, CC BY 2.0 <https://creativecommons.org/licenses/by/2.0>, via Wikimedia Commons
Leukonychia – Keitei, CC BY-SA 3.0 <http://creativecommons.org/licenses/by-sa/3.0/>, via Wikimedia Commons
Dupuytren’s contracture – Frank C. Müller, CC BY-SA 4.0 <https://creativecommons.org/licenses/by-sa/4.0>, via Wikimedia Commons
Palmar erythema – https://dermnetnz.org/topics/palmar-erythema
Conjunctival Pallor – Sheth TN, Detsky AS. The relation of conjunctival pallor to the presence of anemia. J Gen Intern Med. 1997;12(2):102-106.
Corneal Arcus – Loren A Zech Jr and Jeffery M Hoeg, CC BY 2.0 <https://creativecommons.org/licenses/by/2.0>, via Wikimedia Commons
Kayser-Fleischer Ring – Herbert L. Fred, MD, Hendrik A. van Dijk, CC BY 3.0 <https://creativecommons.org/licenses/by/3.0>, via Wikimedia Commons
Xanthelasma – Klaus D. Peter, Wiehl, Germany, CC BY 3.0 DE <https://creativecommons.org/licenses/by/3.0/de/deed.en>, via Wikimedia Commons
Glossitis – Martin Kronawitter, CC BY-SA 2.5 <https://creativecommons.org/licenses/by-sa/2.5>, via Wikimedia Commons
Angular Stomatitis – Matthew Ferguson 57, CC BY-SA 3.0 <https://creativecommons.org/licenses/by-sa/3.0>, via Wikimedia Commons
Mouth Ulcer – Maksim, CC BY-SA 4.0 <https://creativecommons.org/licenses/by-sa/4.0>, via Wikimedia Commons
Gynaecomastia – JMZ1122, CC BY-SA 3.0 <https://creativecommons.org/licenses/by-sa/3.0>, via Wikimedia Commons
Spider Naevi – Herbert L. Fred, MD and Hendrik A. van Dijk, CC BY 2.0 <https://creativecommons.org/licenses/by/2.0>, via Wikimedia Commons
Acanthosis Nigricans – Mark F. Brady; Prashanth Rawla., CC BY-SA 4.0 <https://creativecommons.org/licenses/by-sa/4.0>, via Wikimedia Commons
Surgical Scars – https://mypaces.yolasite.com/abdominal-scars.php
Liver Examination – https://www.youtube.com/watch?v=InMJRyDjOFQ
Palpating Spleen – Clinical Skills Examination Procedures: Afrikaans & Xhosa by Dept of Family Medicine,UCT is licensed under a Creative Commons Attribution-NonCommercial-ShareAlike 2.5 South Africa License.
Balloting Kidneys – Clinical Skills Examination Procedures: Afrikaans & Xhosa by Dept of Family Medicine,UCT is licensed under a Creative Commons Attribution-NonCommercial-ShareAlike 2.5 South Africa License.
Abdominal Aortic Aneurysm – BruceBlaus, CC BY-SA 4.0 <https://creativecommons.org/licenses/by-sa/4.0>, via Wikimedia Commons
Varicose Veins – self, Public domain, via Wikimedia Commons
Pitting oedema – James Heilman, MD, CC BY-SA 3.0 <https://creativecommons.org/licenses/by-sa/3.0>, via Wikimedia Commons
Disclaimer