Cerebellar Examination
Click the button to download our free OSCE Book
Key Message
The cerebellum is the part of the brain which is needed for the coordination of smooth purposeful movements. In order to remember the key symptoms in cerebellar dysfunction you can use the acronym DANISH. This summarises the main features to look out for in the cerebellar exam.
| D – dysdiadochokinesia | I – intention tremor |
| A – ataxia | S – slurred speech |
| N – nystagmus | H – hypotonia |
Introduction
- Wash Your hands
- Introduce yourself by name and role
- Check the patient’s identity – name and Date of Birth
- Explain the procedure – why you need to do it and what does it involve
- Ask for consent
- Expose the patient appropriately
- Check if the patient is currently in any pain
How to Introduce Yourself
“Good morning, my name is .. and I am a medical student. Can I just check your name and date of birth?
I have been asked to do a neurological examination. This will involve testing your eye movements, speech, coordination and assessing your walking. Is that ok?
Can I first check whether you are in any pain?”
Bedside Inspection
- Observe the patient by standing at the end of the bed.
- Comment on whether the patient is ABC:
A – Alert B – (normal) Body habitus C – Comfortable at rest
- Assess for abnormal posture and scars.
- Observe the surroundings and comment of whether you can see any “paraphernalia of neurological disease”:
This is a description of the objects or items around a patient’s bedside that will give you an idea into the condition that they might have. It is important to highlight this to the examiner as this can give you many clues about the patient’s underlying diagnosis. Things to look for include:
- Mobility and hearing aids – gives an idea about the functional status of the patient.
- Medications– iatrogenic causes of cerebellar signs eg phenytoin or medications related to ischaemic vascular disease or thyroid disease.
- Test results – are there any investigation results around the patient’s bedside.
Gait
Action: Ask patient to stand up from a sitting position with their arms folded
Assess for:
–> Truncal ataxia: This is an instability of the proximal muscles. This will give rise to abnormal posturing and instability when the patient tries to stand up.
Action: Ask the patient to walk to the end of the room, turn around and then walk back.
Assess for:
–> Smoothness: Is there any disruption to the normal gait cycle such as abnormalities in toe-off or heel strike?
–> Symmetry: Is the gait symmetrical on both sides? Asymmetry of the gait could be caused by problems such as leg-length discrepancy, fixed flexion deformity, or pain on one side which reduces full extension and weight bearing on that side.
–> Step Height: A damage to the common fibular nerve for example leads to a foot-drop on the affected side. This means the patient will not be able to dorsiflex which gives them a high step height to compensate.

Types of Gait
The gait cycle is made up of 6 phases.
- Heel-strike: this is when the heel first touches the floor.
- Foot flat: here the weight is transferred onto the leg as the foot is all in contact with the floor.
- Mid-stance: the weight is aligned and balanced on this leg.
- Heel-off: Here the heel lifts off as you start to transfer weight onto the other leg.
- Toe-off: this is when the toes finally lift off the floor
- Swing: the foot swings forward until the heel comes back in contact with the ground restarting the cycle.
a) Ataxic gait – this is a gait that looks like someone has just learnt how to walk. The person will watch their feet and walk like a spaceman with a wise stance so that they do not fall over. It is associated with an ataxia, usually due to cerebellar dysfunction.
b) Antalgic gait – A type of gait where the stance phase is abnormally shortened to reduce time on that foot. It looks like a limp –> Implies pain in that leg
c) Waddling gait – This is due to weakness of the proximal muscles of pelvis which causes weakness of gluteus muscles. Patient moves upper body forwards and drags lower leg forward.
d) Spastic gait – this is described as a swinging gait where the patient swings his leg round as it is hyperextended. This is seen in UMN lesions such as stroke
e) High-stepping gait – This is due to damage of the deep branch of the common fibular nerve which leads to foot-drop due to loss of dorsiflexion. This means the patient has a high step in order to compensate.
f) Trendelenburg Gait – this leads to dropping of the pelvis on the contralateral side when you are walking. It is due to damage to the gluteus medius on the supported side –> indicates a lesion of the superior gluteal nerve
g) Parkinson gait – shuffling steps with a stooped over posture. The patient will shuffle forward with lack of arm swing. They will need many small steps to turn around. The gait can appear rushed, and then also freeze.
Action: Ask patient to do walk touching their heel to their toe.
Assess for:
–> Lack of coordination. This is a test which requires the individual to be able to coordinate different muscle groups, and it is more sensitive in detecting ataxia than assessing the normal gait. If impaired, it may signal a cerebellar lesion. This sign is especially sensitive in identifying lesions of the cerebellar vermis, which is seen in alcohol-induced cerebellar degeneration.
Balance is coordinated by the cerebellum which receives input from 3 places. Proprioception, vestibular system and vision. You need at least 2 to keep balance. Romberg’s test removes vision leaving the other two, so you can identify whether the issue is with one of these, or the cerebellum itself which cannot integrate the various stimuli.
Action – Perform Romberg’s test of balance.
a. Position yourself within arms reach of the patient to allow you to intervene should they begin to fall.
b. Ask the patient to put their feet together and keep their arms by their sides (be aware that patients with truncal ataxia may struggle to do this, however, this type of unsteadiness is not the same as a positive Romberg’s sign).
c. Ask the patient to close their eyes.
Assess for:
–> Balance – this is a test which can be used to assess whether there is a problem with proprioception, vestibular function or the cerebellum.
– If patient feels unsteady with eyes closed – this is a positive Romberg’s sign. This shows problem is due to sensory problem (due to proprioceptive disorder or vestibular dysfunction) as the patient feels unsteady when the visual stimulus is removed.
– If patient feels unsteady with eyes open – this is a negative Romberg’s sign. This shows problem is in the cerebellum, due to an issues with coordinating the different sensory inputs.
Eye Movements
After you have tested the gait, you can tell the patient to sit down on the bed so you can assess their eyes.The main thing to assess for in the eyes is nystagmus.
Action: Perform the H-test to assess the eye movements.
a. Sit opposite the patient and hold your finger up in front of the patient’s eyes. Ask the patient to focus on your finger.
b. You can use your other hand to support the top of the patient’s head to ensure that the head stays still.
c. Ask the patient to follow your finger with their eyes, ensuring they keep their head still.
d. Move your finger from side to side, then up and down creating a big “H” pattern.
e. Once you have created the “H” do one final movement where you move your hand horizontally quickly from left to right and observe the patient’s eyes for dysmetric saccades.
Assess for:
–> Double vision: Ask the patient to mention when they get double vision. This could be caused by paralysis of one of the extra-ocular muscles. Find which direction the patient experiences double vision in.
–> Dysmetric saccades: When you move your hand from left to right quickly, the eyes should track your finger quickly and accurately. In cerebellar dysfunction, the patient might miss the target and overshoot – there will then be a corrective movement of they eyes which is called a dysmetric saccade.
–> Impaired smooth pursuit: Normally, the eyes should move smoothly when tracking your finger. If the movements are “jerky” this is a sign of cerebellar dysfunction.
–> Nystagmus: This is an involuntary rhythmic side-to-side, up and down or circular motion of the eyes that occurs with a variety of conditions, which includes cerebellar disease, stroke or vestibular nerve dysfunction.
Speech
Speaking coherently and fluently requires the coordination of the small muscles of the tongue and mouth. Therefore it is a good way of assessing cerebellar function.
Action: Ask the patient to repeat the words “British Constitution” a few times.
Assess for:
–> Slurred speech: This is known as dysarthria which can mimic stroke patients.
–> Staccato speech: This refers to the musical term to describe speech which is short and broken down into small chunks and syllables, with pauses between them. This is because the motor movements in speech are deprived of the regulatory control, which is one of the main functions of the cerebellum.
Upper Limbs
As well as truncal ataxia, it is important to assess the upper and lower limbs for evidence of appendicular ataxia, which is due to damage to the cerebellar hemispheres.
REBOUND PHENOMENON
Action:
a. Ask patient to hold out their arms fully extended with their palms facing upwards and close their eyes.
b. Tell the patient you will push down on one of their arms and ask them to try to keep their arms there against your resistance
c. Push down on one of the patient’s forearms and then quickly let go. Observe the movement of the arm.
Assess for:
–> Rebound phenomenon: In healthy people, the arm should rebound back to its original position. In cerebellar disease, there is no rebound phenomenon

TONE
There are 3 main actions that we use to assess tone in the arms.
Action: Ask the patient to fully relax their muscles so you can passively move them. Support their elbow with one hand and with the other hand hold their hand like you are giving them a handshake.
– Shoulder: Extend and flex the shoulder moving the arm towards you and away.
– Elbow: Support the elbow and holding the hand, carry out passive flexion and extension of the elbow.
– Forearm: In same position, with the elbow at 90-degree flexion, pronate and supinate. Repeat this movement again supinating the forearm very quickly to assess for supinator catch.
– Wrist: Ask the patient to make a fist. Hold their fist and use it to flex/extend and rotate the wrist.
Assess for:
–> Hypo/hypertonia: Hypotonia is associated with ipsilateral cerebellar dysfunction.
COORDINATION
Coordination is an important test as it assess the ability of the brain to synchronise the movement of multiple muscle groups. This is usually controlled by the cerebellum. Therefore, an inability to coordinate the muscles usually points to cerebellar ataxia.
N.B. Do keep in mind that patients may not be able to do these movements due to weakness, pain, or an inability to understand your instructions.
Action: Get the patient to perform the finger nose test
a. Tell the patient to touch their nose with their index finger
b. Now place your finger in front of the patient in a position whether they could stretch their arm to touch it
c. Ask the patient to now touch your finger
d. Ask the patient to touch their nose again and repeat the cycle 3 times. Each time, move your own finger to a new position.
Assess for:
–> Dysmetria: This word means a lack of coordination of muscle groups. Whilst the patient may be able to do the movement really slowly, the key is to assess whether they can do it in a smooth manner or whether they miss the target.
–> Intention Tremor: This is a type of tremor which will get more intense as the patient nears the target (your finger). It is a sign of cerebellar dysfunction.

Disdiadochokinesia
Action: Test for the patient’s ability to make rapid, repetitive movements.
a. Ask the patient to place their right palm out and then put their left palm on top
b. Now ask the patient to turn their left hand over so that back of their left hand is touching their right palm
c. Then ask them to turn it back over to the original position.
d. Ask the patient to repeat these movements as fast as they can.
e. After 10s, repeat the test on the other hand.
Assess for:
–> Disdiadochokinesia: This means an inability to do rapid repetitive movements. In this test, the patient will have slow irregular movements and may stop or get frustrated very quickly. This is a sign of cerebellar dysfunction.

Lower Limbs
TONE
If you have comprehensively assessed the tone in the upper limb, you may not have to repeat this in the legs. But you should still offer to assess for hypotonia.
Action:
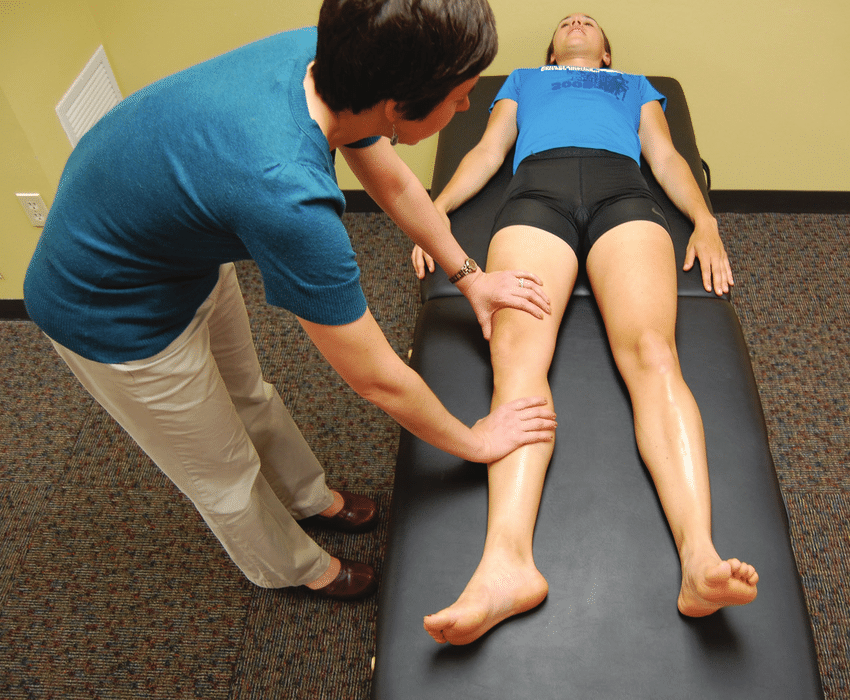
a. With the patient lying on the examination couch, place one hand above and the second hand below the knee. Roll each leg from side to side whilst asking the patient to fully relax.
b. Lift each knee briskly off the bed (warning the patient first) and observe the movement of the leg.
Assess for:
–> Hypotonia of hip, knee and ankle. The best way to do this is to see if the foot swings from side to side as you roll the leg. The foot should swing with the momentum – hypotonia is seen in an ipsilateral cerebellar lesion.
REFLEXES
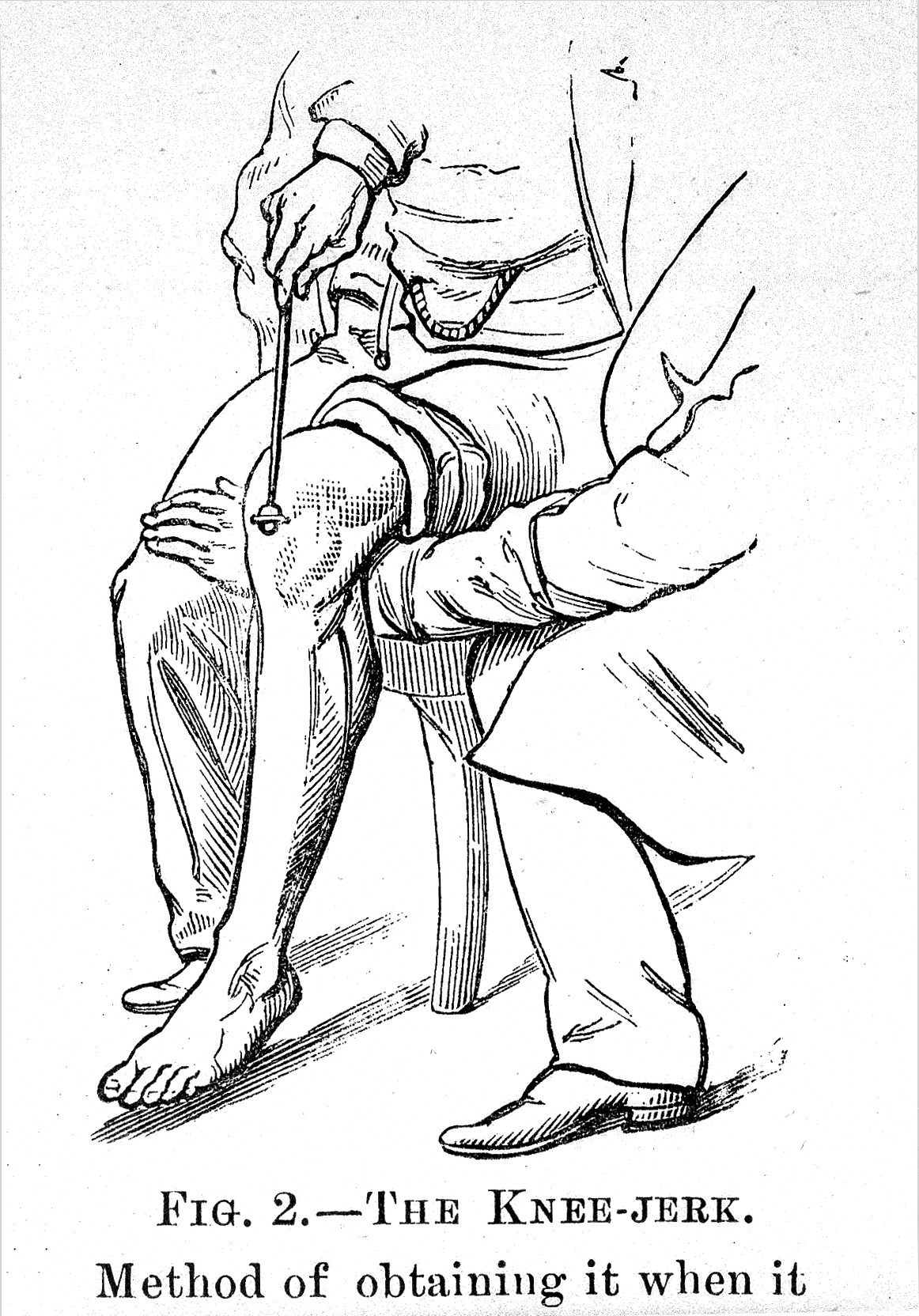
Action: Test the knee jerk reflex in both legs:
a. Ask the patient to hang their legs of the side of the bed and to completely relax their legs.
b. Using a tendon hammer, tap the patella tendon just above the tibial tuberosity
c. You should find that the knee extends and kicks out causing a knee-jerk
Assess for:
–> Pendular reflexes: This refers to a reflex which is slower in its rise and fall, like the pendulum of a clock. Normal reflexes should be brisk. Slow, pendular reflexes are associated with cerebellar lesions.
COORDINATION
Similar to the upper limb, it is important to assess coordination in the lower limbs.
N.B. Do keep in mind that patients may not be able to do these movements due to weakness, pain, or an inability to understand your instructions.
Action: Perform the heel skin test:
a. Ask the patient to place their right heel on their left knee and then slide it down their left leg
b. Then ask them to touch their foot to your hand which you are holding above their foot.
c. Then ask them to touch their right heel to their left knee again restarting the cycle.
d. Now ask them to repeat this sequence of movements in a smooth motion up to 5 times.
e. Repeat the assessment with the other side.
Assess for:
–> Dysmetria: This word means a lack of coordination of muscle groups. Whilst the patient may be able to do the movement really slowly, the key is to assess whether they can do it in a smooth manner, else they may have cerebellar dysfunction.
Thank the patient and wash your hands again!

On Completion
“To complete the examination, I would do a number of steps…”
Bedside
- (History) Take a full history including effects on life and functional status
- (Observations) Full set of observations
- (Corresponding examination) Conduct a full body neurological assessment and cranial nerves. Offer a full assessment of cognitive and higher order functions like speech
Bloods – FBC, inflammatory markers, renal profile etc.
Imaging – MRI scan (if indicated)
Sources
Gait Cycle – Ducky2315, CC BY-SA 3.0 <https://creativecommons.org/licenses/by-sa/3.0>, via Wikimedia Commons
Optokinetic Nystagmus – Student BSMU, CC BY-SA 3.0 <http://creativecommons.org/licenses/by-sa/3.0/>, via Wikimedia Commons
Rebound Phenomenon – Use of Machine Leaning Classifiers and Sensor Data to Detect Neurological Deficit in Stroke Patients – Scientific Figure on ResearchGate. Available from: https://www.researchgate.net/figure/The-pronator-drift-test-a-the-degree-of-drift-in-the-weak-arm-and-counter-arm-of-a_fig2_316354616
Finger Nose Test – https://clinicalgate.com/coordination-2/#F0010
Dysdiadochokniesia – Evan-Amos, CC BY-SA 3.0 <https://creativecommons.org/licenses/by-sa/3.0>, via Wikimedia Commons
Knee-Jerk Reflex – Wellcome Collection gallery (2018-04-03): CC BY 4.0 <https://creativecommons.org/licenses/by/4.0>, via Wikimedia Commons
Heel Shin Test – https://www.researchgate.net/profile/Abilo-Tadesse/publication/334697259/figure/fig25/AS:784835681456136@1564130816979/Performing-Heel-to-Shin-test.jpg
Disclaimer



