Back to: Gynaecology
Ovarian Conditions
Ovarian Torsion
This is when the ovary twists on its supporting ligaments.
It is a gynaecological emergency as it can cut of the blood supply to the ovary, resulting in ischaemia
Risk factors:
– Ovarian cysts (especially dermoid cyst/PCOS)
– Ovulation induction
Symptoms:
Sudden onset of sharp, colicky, unilateral lower quadrant abdominal pain
– Nausea and Vomiting
– May also be a low-grade pyrexia and sinus tachycardia
Tests:
Pelvic ultrasound is used –> unilateral ovarian enlargement, oedema, ‘whirlpool’ sign
– Laparoscopy is diagnostic
Treatment:
Emergency laparoscopy to uncoil twisted ovary + fixation
Polycystic Ovary Syndrome (PCOS)
This is a syndrome of unknown cause involving hormonal abnormalities and ovarian dysfunction.
The key hormonal abnormalities in PCOS include:
i) Insulin resistance resulting in hyperinsulinemia
ii) Increased androgens –> hyperinsulinemia or increased LH production by the anterior pituitary gland
– This leads to excessive androgen production by theca cells of the ovaries.
– In addition, hyperinsulinemia leads to reduced production of sex-hormone binding globulin in the liver
– This means there are higher levels of free testosterone.
– High androgens stop follicle development and ovulation. Follicles remain in the ovaries as multiple cysts.
Symptoms:
– Due to anovulation –> oligomenorrhoea, subfertility
– Due to excessive circulating androgens –> hirsutism and acne
– Due to insulin resistance –> weight gain/difficulty losing weight
– May also cause psychological problems like depression
Complications:
– Increased risk of T2DM, HTN and cardiovascular disease
– Increased risk of endometrial cancer due to anovulatory cycles:
– If ovulation does not occur, oestrogen production by the ovary remains high. High unopposed oestrogen levels can lead to hyperplasia of the endometrium.
Tests:
– Blood tests –> High testosterone, Low SHBG, High LH, Normal FSH
– Impaired glucose tolerance test
– Ultrasound –> polycystic ovaries are those with 12+ follicles or increased volume >10cm3
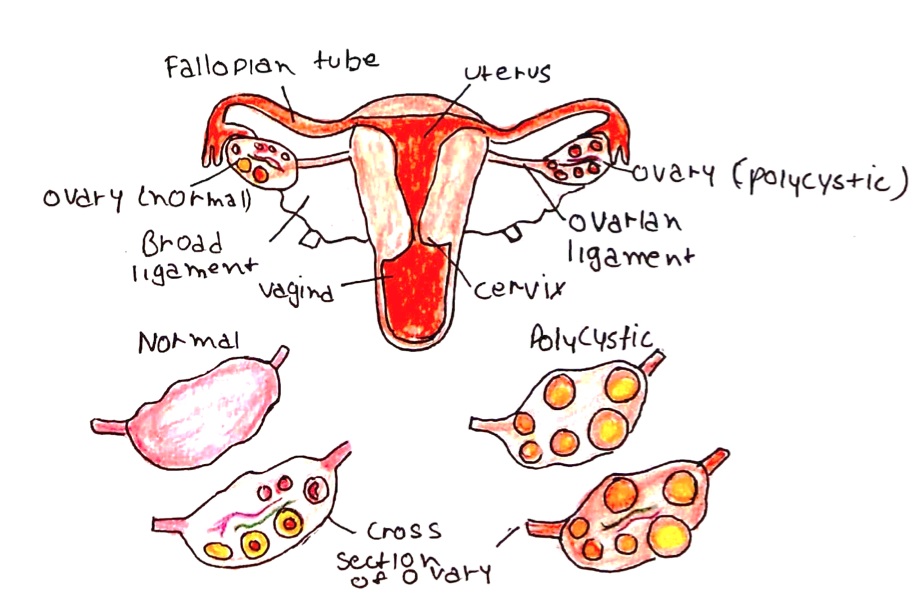
Diagnosis:
PCOS should be diagnosed according to the Rotterdam criteria (4) – diagnosed PCOS if 2/3 of:
i) Polycystic ovaries on USS
ii) Oligo or anovulation
iii) Clinical/biochemical signs of hyperandrogenism
Management (NICE CKS5):
– For all symptoms –> Weight loss reduces hyperinsulinism + hyperandrogenism
– This helps to restore menstrual regularity, improve fertility.
There are also specific treatments you can give to counter particular symptoms in PCOS:
Specific Treatments
For Oligomenorrhea/Amenorrhea:
If <1 period, every 3 months:
– Give medroxyprogesterone for 14d to induce a bleed
– Refer for TVUS to assess endometrial thickness (to check for hyperplasia/cancer)
If the endometrium is normal, give treatment to prevent endometrial hyperplasia. Options include:
– Cyclical progesterone (e.g. medroxyprogesterone for 14d every 1-3 months), COCP, IUS
For Hirsutism:
1st line = COCP (also helps to stop acne) + advice on hair removal methods
– Topical eflornithine is an option for facial hirsutism
For subfertility:
Refer to specialist for subfertility advice
Sources
1. https://www.nice.org.uk/guidance/cg122/chapter/1-Guidance#footnote_11
2. https://www.rcog.org.uk/globalassets/documents/guidelines/gtg_62.pdf
3. https://www.rcog.org.uk/globalassets/documents/guidelines/green-top-guidelines/gtg_34.pdf
4. https://www.fertstert.org/article/S0015-0282(03)02853-X/fulltext
5. https://cks.nice.org.uk/polycystic-ovary-syndrome#!scenarioRecommendation:3


