Back to: Gynaecology
Menstrual Conditions
Premenstrual syndrome (PMS)
This describes the distressing physical, psychological and behavioural symptoms in the absence of organic disease that regularly occur during the luteal phase of the menstrual cycle
– This occurs in most women and encompasses a whole spectrum of severity from minor to debilitating.
– Cause unknown but associated with change in levels of oestrogen + 5-HT levels at the beginning of cycle
Symptoms:
– Psychological –> depression, anxiety, irritability
– Physical –> fatigue, bloating, mastalgia, acne
Management:
– If mild, then reduce salt, caffeine and stress
– 1st line is Combined oral contraceptive pill
– 2nd line is SSRIs
Menorrhagia
This is excessive menstrual blood loss that occurs regularly and interferes with a woman’s quality of life.
– In 50% of women no underlying cause if found – this is known as dysfunctional uterine bleeding
Menorrhagia can also occur secondary to underlying disease:
Secondary Causes of Menorrhagia
Uterine:
– Endometriosis
– Adenomyosis
– Fibroids
– PID
– Endometrial hyperplasia and cancer
Endocrine:
– PCOS
– Hypothyroidism
– Hyperprolactinaemia
Iatrogenic:
– Copper IUD
Haematological:
– Anticoagulants
– Coagulopathy
Tests:
– For all women, carry out FBC to check for iron-deficiency anaemia as a result of excessive bleeding
– NICE1 advises that the need for investigation into the cause depends on the woman’s presentation:
i) If menorrhagia with no other symptoms:
–> Can start treatment without further investigation
ii) If menorrhagia + intermenstrual bleeding, pelvic pain, pressure symptoms, suggests underlying pathology:
– First perform an abdominal and bimanual examination
– Then do investigation for the particular cause:
– Structural uterine cause suspected (e.g. fibroids/endometrial pathology) -> refer for USS/hysteroscopy
– Hypothyroidism suspected -> TFTs
– Coagulation disorder suspected (suspect if menorrhagia since menarche + family/personal history suggesting coagulation disorder) -> coagulation screen
– Infection suspected -> vaginal or cervical swab
Management:
If underlying cause found, follow management for that condition, else:
1st line is Mirena progesterone coil
2nd line options:
– Hormonal = COCP or cyclical oral progestogen
– Non-hormonal = tranexamic acid or NSAID (mefenamic acid)
– If menorrhagia persists, refer to gynaecology for further investigation, endometrial ablation or hysterectomy
Dysmenorrhoea
A condition which is defined by excessive amount of pain during the menstrual cycle, divided into 2 types:
i) Primary Dysmenorrhoea:
This is where there is excessive pain without underlying pelvic pathology
– It usually occurs 6-12 months after menarche
– Thought to be related to excessive endometrial prostaglandin synthesis during menstruation
Symptoms:
– Pain starts just before/within a few hours of the period starting and improves later in the period
– Cramping lower abdominal pain which can radiate to the back or down the thigh
– May be accompanied by nausea, vomiting, fatigue, headache and emotional symptoms
Management:
– Stop smoking (clear link between smoking and dysmenorrhoea)
– 1st line is NSAIDs (these inhibit prostaglandin synthesis) +/- paracetamol
– 2nd line is combined oral contraceptive pill
ii) Secondary Dysmenorrhoea:
This is where there is excessive pain as a result of underlying pathology
– It usually starts many years after menarche, after years of normal painless periods
Causes:
Endometriosis, adenomyosis, pelvic inflammatory disease, fibroids, IUD
Symptoms:
– Pain that is not consistently related to menstruation
– Pain may continue after period has ended or may be constantly present but worse during menstruation
– Accompanied by symptoms of the underlying pathology
Management:
– Identify underlying cause and treat accordingly
Amenorrhoea
This is defined as the lack of a normal period. It is typically divided into two types:
i) Primary Amenorrhea
This is the failure to start menstruation for a girl by the age of 16. It can be due to a number of potential causes
Causes:
– Constitutional Delay
– Chromosomal conditions – Turner’s syndrome, Kallman’s syndrome
– Endocrine conditions – congenital adrenal hyperplasia
– Structural conditions – Imperforate hymen, Mayer-Rokitansky-Küster-Hauser syndrome
Types of Aphasias
Constitutional delay:
This is a a general delay in pubertal development.- Not pathological and normal maturation usually occurs spontaneously by 18 years of age.- Often a family history of late puberty/menarche.
Turner’s syndrome (45XO):
This is a condition where individuals possess only one X chromosome.
– In Turner’s syndrome there is gonadal dysgenesis and early loss of ovarian function. The absence of ovarian hormones results in amenorrhoea as well as failure to develop secondary sexual characteristics.
Kallman’s syndrome:
This is an X-linked recessive condition caused by defective development of GnRH neurons.- It is characterised by anosmia + absent puberty/menarche.
Congenital adrenal hyperplasia:
This is a condition, where, in most cases caused by partial deficiency of 21-hydroxylase.
– This enzyme catalyses aldosterone and cortisol synthesis. The deficiency causes build-up of precursors, so they are instead converted into testosterone raising levels.
– The high levels of testoserone in females leads to menstrual problems with poor development of the female genitalia
Imperforate Hymen:
This may cause amenorrhoea with cyclical pelvic pain (as endometrium builds up but cannot shed via the vagina).
Mayer-Rokitansky-Küster-Hauser syndrome:
This is a condition where there is agenesis of the Mullerian duct result in absence of the uterus and upper 2/3 of the vagina
ii) Secondary Amenorrhea
This is the cessation of established, regular menstruation for 6 months or longer
– Many conditions that give secondary amenorrhoea also give primary amenorrhoea if they occur before menarche
Causes:
It can be due to natural phenomena such as pregnancy, lactation and menopause but there are also pathological causes (categorised by organ)
Uterine Conditions:
– Cervical stenosis
– Ashermann’s syndrome
Ovarian Conditions:
– Premature Ovarian Failure
– Polycystic Ovarian Syndrome
Endocrine Conditions:
– Prolactinomas –> prolactin suppresses GnRH secretion
– Sheehan syndrome –> pituitary infarction due to massive obstetric haemorrhage which occurs after a complicated delivery
– Contraception –> COCP taken continuously, progestogen implants/injections
– Hyper or hypothyroidism
– Cushing’s syndrome
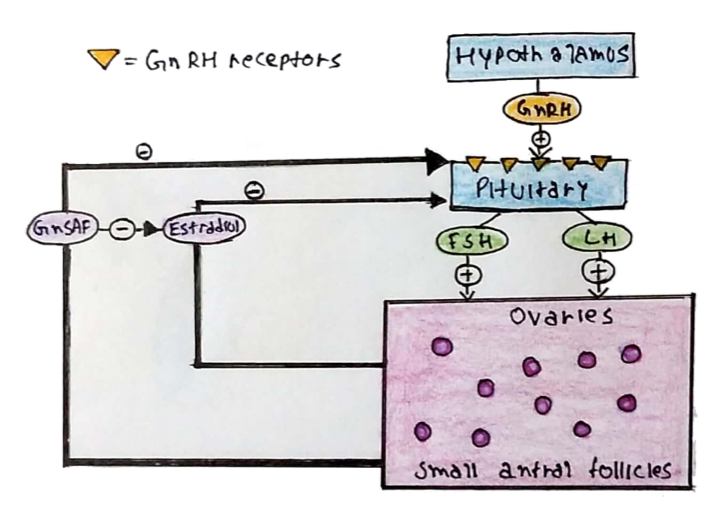
Hypothalamic Conditions:
– Hypothalamic amenorrhoea -> dysfunction of the hypothalamus caused by stress, excessive exercise affecting GnRH secretion
– Eating disorders –> lead to very reduced calorie intake
– Chronic diseases –> e.g. chronic heart/kidney/liver disease, IBD
Tests:
– Pregnancy test
– Blood tests –> FSH/LH, total testosterone levels, TFTs, Prolactin
– Transvaginal ultrasound –> used to assess for structural causes
– Genetic tests and karyotyping –> used to assess for genetic/chromosomal causes
Management:
Treat the underlying cause


