Back to: Gynaecology
Benign Breast Conditions
Mastitis
This is a condition that refers to inflammation of the breast
– It is associated with breastfeeding: milk stasis can cause an inflammatory response -> may then get secondary infection, most commonly with staphylococcus aureus
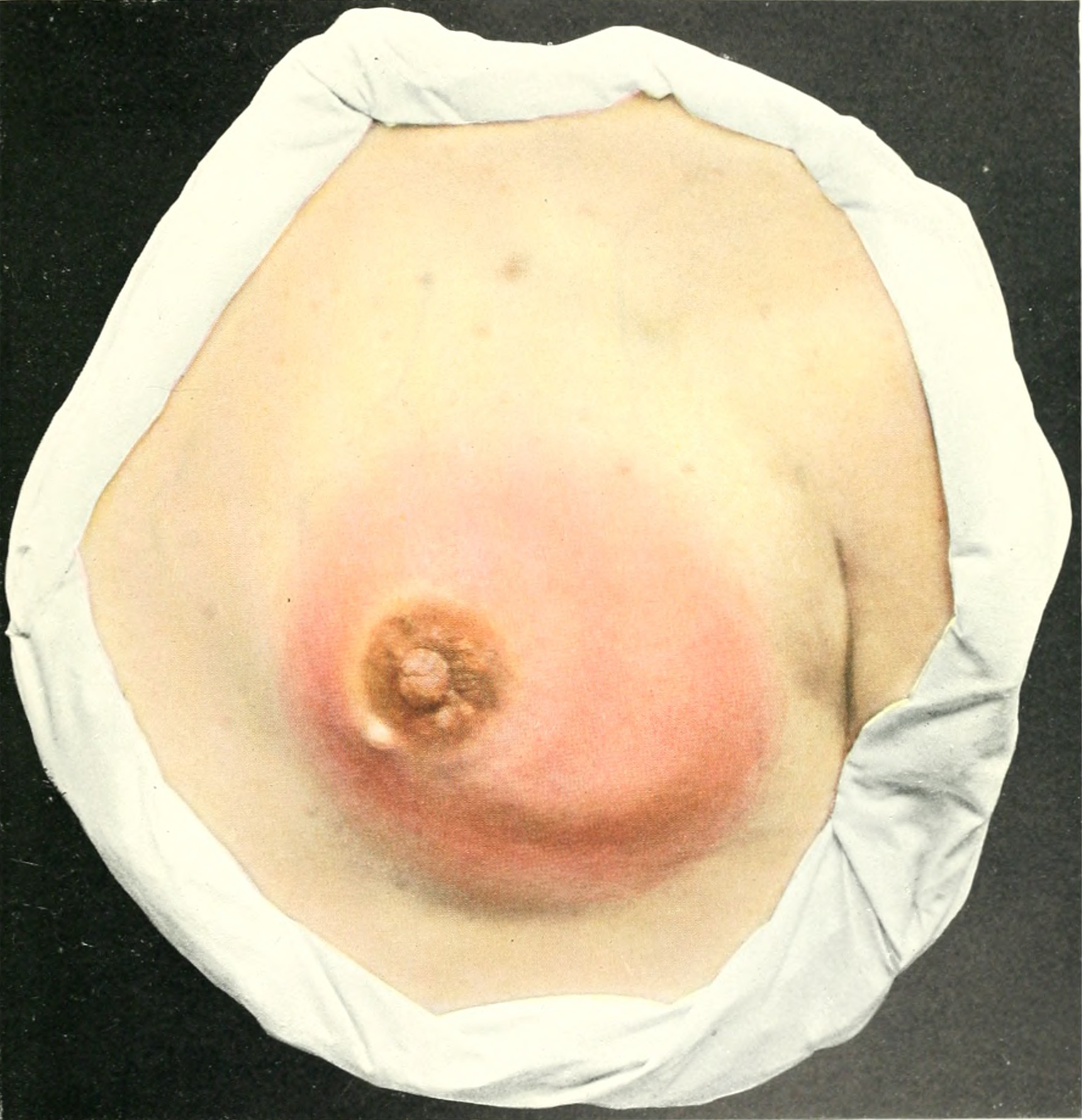
Symptoms:
Erythematous, tender, swollen area of breast
– Systemic upset with fevers, chills and fatigue
Management:
– 1st line is to advise continue breastfeeding, ensuring the breast is fully emptied
– If symptoms do not improve after 24 hours of milk removal –> Flucloxacillin 10-14 days
Breast Abscess
This can occur if mastitis is left untreated
Symptoms:
Gives a tender, red fluctuant mass + associated with history of lactational mastitis
Management:
Urgent referral to surgeon for aspiration/drainage and antibiotics e.g. flucloxacillin
Mammary duct ectasia
This is dilation and shortening of the subareolar ducts. It causes ducts to become blocked and the secretions to stagnate
– Classically arises around menopause in women (>50 years) who have multiple children.
Symptoms:
Presents with thick green-brown nipple discharge + lump behind the nipple
Management:
Refer to gynaecology and advise to stop smoking. The condition is usually self-limiting
Periductal mastitis
This refers to an inflammatory condition of the subareolar ducts.
– Unlike mammary duct ectasia, it tends to occur in younger women
– The cause of this inflammatory condition is unknown, but smoking is a major risk factor
– It can lead to mastitis, abscess formation and development of fistulae between subareolar ducts and the skin
Fat necrosis
This is the necrosis of breast fat. It usually occurs following injury to the fatty breast tissue (e.g. by minor trauma or breast biopsy, radiotherapy or surgery)
Symptoms:
Firm, round breast lump
– May be accompanied by changes of the overlying skin (e.g. red, bruised)
Tests:
Triple Assessment to rule out breast cancer
Management:
No treatment is needed once the diagnosis is confirmed
Fibrocystic change/Fibroadenosis
This is the development of fibrosis and cystic changes in the breast
– Most commonly occurs in women in their 40s.
Symptoms:
Lumpy, nodular breasts –> fibrosis is firm/rubbery, cysts are soft + fluctuant
– May be accompanied by breast pain
– Symptoms may fluctuate throughout the menstrual cycle, getting worse just before the time of menstruation
Tests:
Triple assessment to rule out breast cancer if suspected
Intraductal Papilloma
This is the growth of a benign wart-like lump that develops in large mammary ducts
– It is completely benign but the most common cause of bloody nipple discharge in women ages 20-40
Symptoms:
Clear or blood-stained nipple discharge, but they are too small to be palpated
Tests:
Can be detected on ultrasound. Galactogram is definitive test
Management:
Surgical excision if symptomatic
Fibroadenoma
This is a benign tumour that forms from a breast lobule and is composed of both fibrous and glandular tissue
– It is commonly seen in premenopausal women (<30 years), but there is no increase in the risk of malignancy
Symptoms:
Well circumscribed, non-tender highly mobile marble-like mass
– 1/3 get larger, 1/3 reduce, 1/3 stay the same
Tests:
Triple assessment to rule out breast cancer
Treatment:
Usually none needed, surgical excision if large or complex
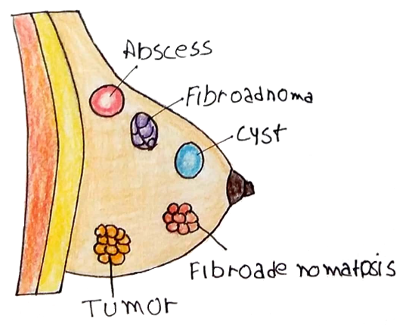
Sources
1. Atlas of clinical surgery; with special reference to diagnosis and treatment for practitioners and students (1908). Bockenheimer, Ph. (Philipp), b. 1875
2. Wellcome Images/ CC BY (https://creativecommons.org/licenses/by/4.0)
3. https://cks.nice.org.uk/breast-cancer-recognition-and-referral#!scenario


