Back to: Gynaecology
Menopause
Menopause refers to the natural halting of the menstrual cycle due to depletion of ovarian follicles.
– It is defined as amenorrhoea for 2 years below the age of 50 or 12 months over the age of 50.
– The average age of menopause in the UK is 51.
– Perimenopause refers to the period before the menopause in which the woman begins to experience symptoms of the approaching menopause
Pathophysiology of Menopause
Each woman is born with a finite number of oocytes and over time the supply in the ovaries depletes:
– In the perimenopausal period, declining follicle numbers leads to fewer available binding sites for LH + FSH
– Reduced binding of LH and FSH results in a reduction in follicular oestrogen production
– Declining levels of oestrogen gives more anovulatory cycles, giving irregular periods + menopausal symptoms
– There is reduced pituitary inhibition, causing erratic secretion of FSH, LH, GnRH
– Eventually follicular development stops altogether and amenorrhoea occurs
– Menopause is characterised by low oestrogen and high FSH/LH
Symptoms:
– Menstrual changes -> change in length, frequency and amount of blood loss
– Hot flushes and night sweats
– Joint and muscle aches
– Atrophic vaginitis -> vaginal dryness/discomfort, superficial dyspareunia, recurrent UTIs
– Mood changes
– Sleep problems
Complications:
– Osteoporosis –> as oestrogen protects bone mass by reducing osteoclast activity
– Increased risk of ischaemic heart disease –> as oestrogen is protective against IHD iii) Increased risk of dementia
Diagnosis:
– Perimenopause –> diagnose if the woman has irregular periods and hot flushes/night sweats
– Menopause –> diagnosis when periods have been absent for at least 12 months
– Can measure FSH levels (tend to be high), which gives you estimate of ovarian reserve
Management (according to NICE Guidelines1):
i) Conservative:
– Exercise, weight loss, sleep and stress reduction
ii) Hormone replacement therapy:
– If vaginal symptoms only –> prescribe oestrogen topical gel
– If no uterus or IUS (coil) –> can prescribe oestrogen only HRT
– If they have a uterus –> combined oestrogen and progesterone HRT
–> if perimenopausal (last period <1 year ago) –> cyclical regime
–> if postmenopausal (last period >1 year ago) –> continuous
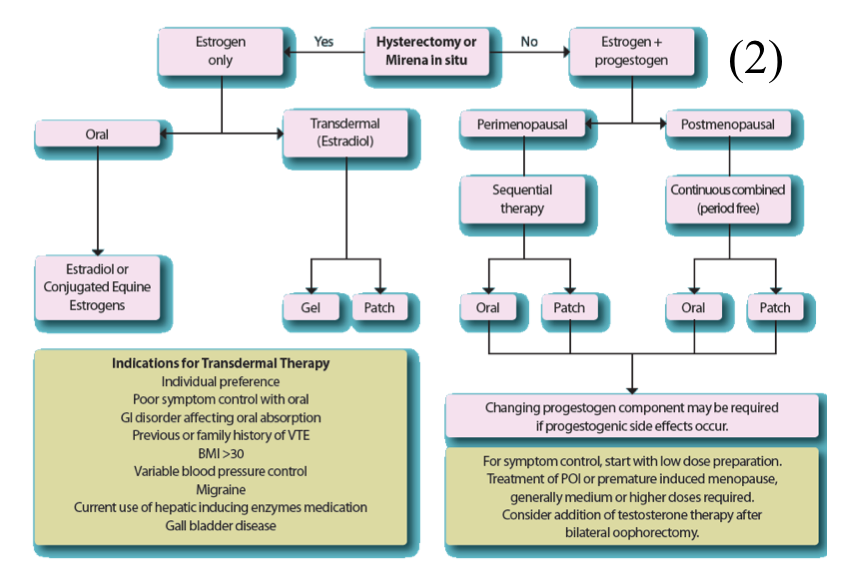
iii) Other medical management: (if HRT declined/contrindicated)
– For Vasomotor symptoms –> fluoxetine, citalopram or venlafaxine
– For Vaginal dryness –> lubricant or moisturiser
– For Mood disturbance –> self-help groups, CBT, antidepressants
N.B. HRT (except the progesterone coil) does not work as a contraceptive. Therefore, to avoid pregnancy, contraception is still required until a woman is no longer considered fertile
Premature Ovarian Failure
This is when menopause occurs before the age of 40yrs
Causes:
Idiopathic, autoimmune, iatrogenic (e.g. chemotherapy, radiotherapy)
Symptoms:
Gives similar symptoms to menopause but at an earlier age
Diagnosis:
Must have menopausal symptoms + High FSH (on 2 blood samples taken 4-6 weeks apart)
– If doubt, AMH (Anti-Mullerian hormone) levels may be used. This provides a direct measure of ovarian reserve
Management:
HRT
Sources
2. https://thebms.org.uk/wp-content/uploads/2020/02/04-BMS-TfC-HRT-Guide-FEB2020.pdf (information on side effects, risks and benefits also from the BMS)


