Back to: Neurology
Stroke
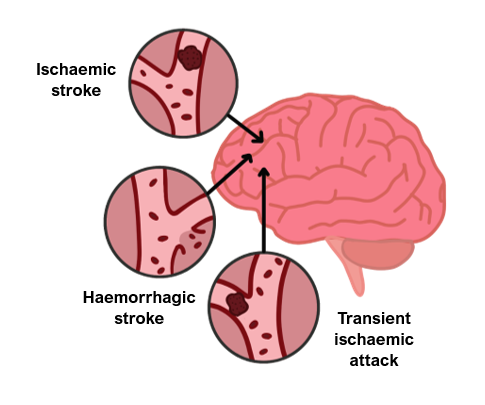
Ischaemic Stroke
This refers to brain ischaemia that results in neurological damage lasting > 24 hours.
It occurs due to occlusion of an artery which reduces blood flow to the brain.
Embolic
This is where a clot breaks off and occludes a part of the cerebral circulation.
The most frequent source of emboli are clots dislodged from the left side of the heart, in patients with atrial fibrillation. These often block the middle cerebral artery (MCA).
Emboli can cause single arterial blockage or ‘showers’ to multiple arteries and arterial distributions.
Thrombotic
This is a stroke due to a rupture of an atherosclerotic plaque, commonly in the MCA.
Lacunar stroke
This is a stroke where there is occlusion of a single small perforating artery supplying subcortical areas.
It is usually secondary to arteriosclerosis from hypertension, causing small areas of infarction.
Risk factors
Hypertension
Smoking
Diabetes
Hyperlipidaemia
Atrial fibrillation
Hypercoagubility states
Symptoms
The Oxfordshire/Bamford stroke classification identifies 3 key features:
Unilateral hemiparesis or hemisensory deficit
Homonymous hemianopia
Higher order cerebral dysfunction, e.g., dysphasia, neglect
Vascular Territories and Associated Symptoms
Anterior circulation
This comprises of the anterior and middle cerebral artery.
A total anterior circulation stroke (TACS) gives all three of the above.
A partial anterior circulation stroke (PACS) gives two out of three of the above.
In an anterior cerebral artery stroke, the legs are affected more than the arms, due to the somatotropic map of the brain.
Posterior cerebral artery
This leads to a contralateral homonymous hemianopia with macular sparing and cerebellar symptoms.
Lacunar stroke
This can cause one of the following: sensory, motor or sensorimotor deficit, or ataxic hemiparesis.
Basilar artery
An occlusion of the basilar artery can give rise to locked-in syndrome.
Posterior cerebral artery branch to midbrain (Weber syndrome)
Ipsilateral oculomotor palsy, with contralateral weakness of arms and legs
Posterior inferior cerebellar artery (Wallenberg syndrome)
Cross-body sensory deficit: ipsilaterally face and contralaterally on the limbs
Key tests
Blood glucose reading to exclude hypoglycaemia as the cause
Non-contrast CT immediately to exclude haemorrhage (this can also identify gross ischaemic changes after a few hours and dense vessels suggestive of a thrombus)
Management
If haemorrhage has been ruled out, then it depends on the timing:
If within 4.5 hours of onset, arrange for thrombolysis (e.g., with alteplase)
Thrombectomy may be available in some cases (e.g., if symptom onset is within 6 hours of presentation and confirmed occlusion of the anterior circulation)
If later/other options unavailable, loading dose of 300 mg aspirin (if on anticoagulation, this is usually held for 14 days while the patient is on aspirin 300 mg).
Secondary prevention
Antiplatelet therapy e.g., clopidogrel; if contraindicated, aspirin and dipyridamole
Atorvastatin started in all regardless of cholesterol levels
Optimise blood pressure
If patient has atrial fibrillation, anticoagulation is started after 2 weeks to reduce the bleeding risk. A 72-hour heart monitor can be performed if no AF is seen on the ECG.
Carotid endarterectomy is recommended if the stroke/TIA is in the anterior circulation area, and there is ipsilateral carotid stenosis > 70% on carotid doppler and angiography
Transient Ischaemic Attack
This is an ischaemic event with the same symptoms as a stroke that last < 24 hours.
Without intervention, patients are at high risk of having a stroke.
Driving is prohibited until they have seen a specialist.
Key tests
MRI scan of brain is usually normal
Carotid doppler to look for carotid stenosis and angiography if stenosis seen
As for stroke, lipid profile, ECG (and 72-hour tape if no AF seen)
Management
Patients should be seen within 24 hours and offered aspirin 300 mg
Antiplatelet – clopidogrel lifelong
Statin to lower of cholesterol
Blood pressure management
Lifestyle factors
ABCD2 Score
Risk Factors | Points | |
Age | ≥60 | 1 |
Blood Pressure | Systolic ≥140mm Hg OR Diastolic ≥90mm Hg | 1 |
Clinical Features | Unilateral weakness with or without speech impairment | 2 |
Duration | TIA duration ≥60 mins | 2 |
Diabetes | 1 | |
Total Score between 0-7 | ||
Haemorrhagic Strokes
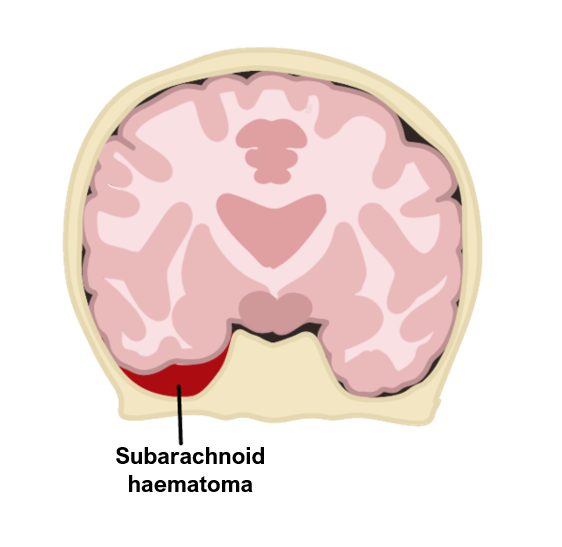
Subarachnoid haemorrhage (SAH)
This is a bleed into the subarachnoid space.
It damages the brain through tissue hypoxia and raised intracranial pressure.
It can be spontaneous or secondary to trauma to the head e.g., road traffic accident
Risk factors
Hypertension, smoking
Arteriovenous malformation
Berry aneurysms (associated with polycystic kidneys)
Marfan syndrome
Symptoms
Sudden onset severe headache (like a thunderclap, in occipital region)
Vomiting, seizures, reduced consciousness
Meningism – photophobia and neck stiffness
Cheyne-Stokes breathing – deeper, then shallower with apnoea, occurs in cycles
Kernig’s sign (takes 6 hours to develop), defined as an inability to extend the knee when patient is supine and the hip/knee is flexed. This is caused by irritation to the motor nerves passing through the inflamed meninges under tension.
Complications
Rebleeding
Hyponatreamia (due to SIADH)
Hydrocephalus
Arterial vasospasm – cerebral arteries constrict causing secondary brain ischaemia
Key tests
1st line is non-contrast CT
Lumbar puncture if CT is negative, performed at least 12 hours after headache onset to look for xanthochromia (RBC breakdown in CSF)
If positive, angiography can be performed to identify surgical target
Management
Refer to neurosurgery – options include endovascular coiling/clipping
Give nimodipine to prevent artery vasospasm and reverse anticoagulation
Intracerebral Haemorrhage (ICH)
This is a bleed within the brain tissue or ventricles.
It is associated with a Charcot-Bouchard microaneurysm of the striate vessels.
The main risk factor is hypertension, which can be secondary to factors like hyperaldosteronism, smoking and diabetes.
Symptoms
Similar to SAH, e.g., headache, nausea, vomiting, low consciousness
Localising symptoms depending on area affected, e.g., hemiplegia
Key tests
Same as SAH (CT head is first line)
Management
Rapid correction of blood pressure (range 140–160 mm Hg) and clotting
Refer to neurosurgery – may require surgery (e.g., craniotomy or burr hole) if reduced conscious level and/or brain herniation present
Intracranial Venous Thrombosis
This is thrombosis of the cerebral veins in the sinuses which leads to cerebral infarction.
This usually occurs within one of the dural venous sinuses which are responsible for the venous drainage of the brain.
Risk factors
Hypercoagulable states – pregnancy, malignancy, SLE
Head injury, dehydration
Symptoms
Can be sudden onset, with headache, nausea and vomiting
Seizures
Hemipgeia
Cranial nerve palsies
Key tests
CT head to exclude subarachnoid haemorrhage
Thrombophilia screen blood test
CT/MRI venogram is the diagnostic test
Management
Anticoagulation with heparin/LMWH then warfarin
If deterioration, may require endovascular thrombolysis


