Back to: Endocrinology
The Pancreas and Insulin
The normal blood glucose in the body is 4-6mM and is controlled by pancreatic hormones insulin and glucagon.
– It is important to control these as certain organs like the brain can only use glucose as a respiratory substrate.
– Normally glucose –> broken down by glycolysis –> enters Krebs cycle –> oxidative phosphorylation.
Some cells can also metabolize fat. This produces reduced FAD/NAD which enter oxidative phosphorylation.
But some organs like the brain cannot break down fat and instead use ketone bodies which are made in the liver.
These ketone bodies are an alternative fuel source – They are Acetone, Acetoacetate and B-hydroxybutyrate.
– Acetyl CoA + Acetyl CoA –> Acetoacetyl CoA –> HMG-CoA –> Acetyl CoA + Acetoacetyl CoA
Insulin
This is a peptide hormone which is synthesized in the b-cells in the islets of Langerhans in the pancreas.
– When blood glucose increases, more glucose enters the cells through GLUT2 channels –> more glycolysis occurs –> increase in cell ATP
– ATP binds to KATP channels (which is attached to sulphonylurea receptor) closing them –> leads to cell depolarisation
– Voltage gated Ca2+ channels open –> increase in exocytosis of insulin.
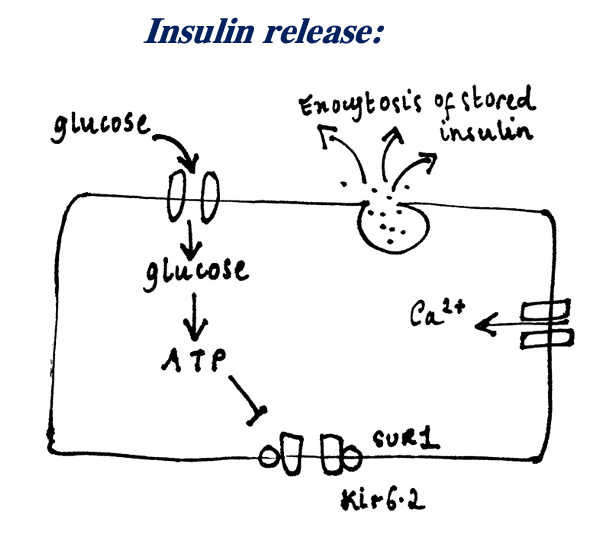
There are many factors which affect insulin release in the body:
i) Cephalic phase – parasympathetic stimulation (using Ach) of Beta-cells promotes anticipatory insulin release before consuming a meal
ii) Blood glucose – insulin levels rise if [glucose] > 5mM
iii) Incretins – GIP and GLP-1 are stomach hormones released in response to oral glucose. These stimulate insulin release and inhibit glucagon. These are broken down by enzyme dipeptidyl peptidase 4 (DPP-4)
iv) Sympathetic stimulation – it inhibits insulin release, allowing blood glucose to increase in exercise.
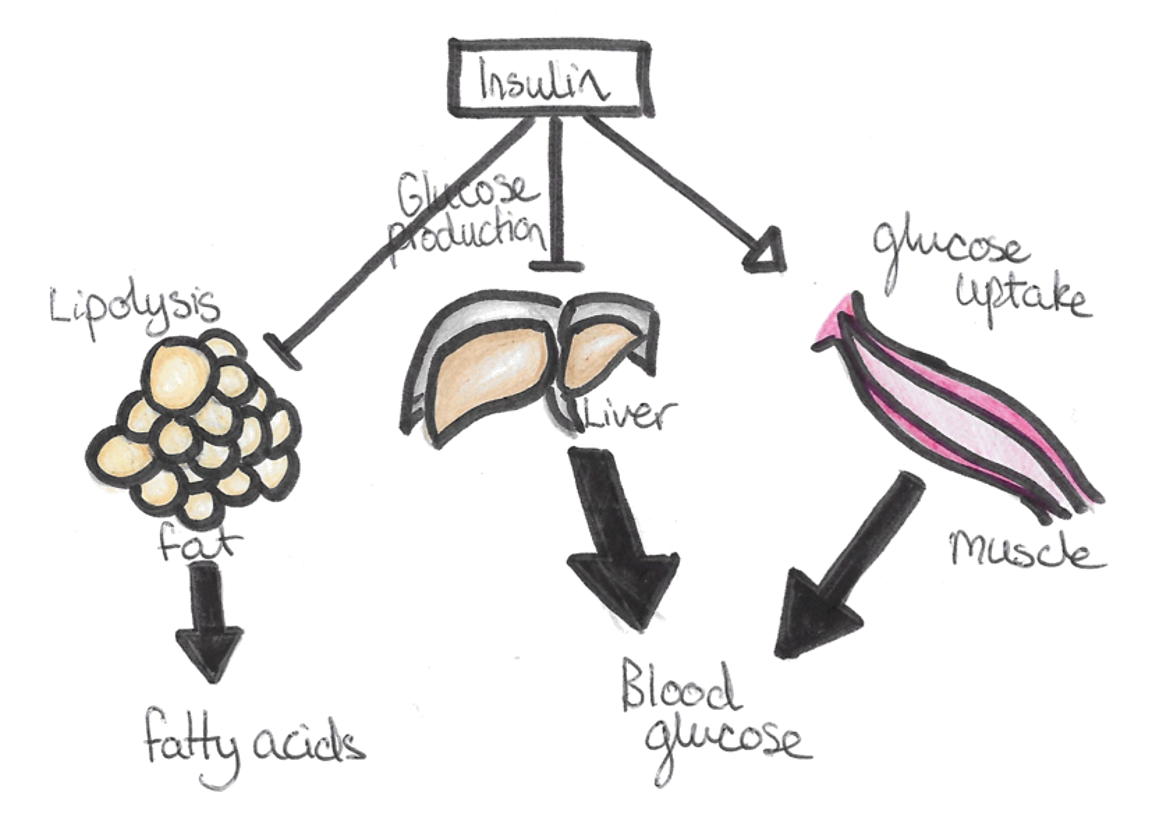
Insulin actions:
Insulin exerts its effect by binding to the insulin receptor – a tyrosine kinase linked receptor.
– Acts through messenger Akt2 which aims to reduce blood glucose and increase storage as glycogen and fat.
Muscle:
– Promotes glucose uptake by translocation of GLUT4 to membrane + glucose metabolism and glycogenesis
– Stimulates amino acid uptake and protein synthesis
Fat:
– Promotes glucose uptake and conversion to fat
– Inhibits fat breakdown and promotes fat uptake
Liver:
– Promotes glycogenesis and fat synthesis
– Inhibits gluconeogenesis and glycogen breakdown
Glucagon
On the other hand, glucagon is produced by the a-cells in the islets of Langerhans. It works to blood glucose and fatty acids, acting as the main catabolic hormone of the body
Release:
It is produced by the pancreas when concentration of insulin and glucose in the bloodstream falls too low.
– Stimulated by hypoglycaemia and adrenaline but inhibited by insulin and hyperglycaemia
Actions:
It promotes gluconeogenesis and glycogenolysis in the liver raising free blood glucose
– Decreases fatty acid synthesis + promotes lipolysis in liver and adipose for use by skeletal muscle.


