Back to: Renal-Urinary Systems
Control of Potassium
We need to regulate potassium as it determines the resting membrane potential.
– As the relative permeabilities of sodium and calcium are very low, K+ is the main determinant.
– Normal extracellular [K+] = 4mM
– Intracellular [K+] = 125mM
– As the extracellular space much smaller than intracellular 16:24 litres, changes in [K+] extracellular affect Em greatly.
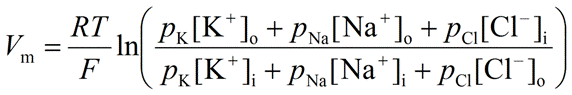
Why K+ changes
The Potassium concentration can change for many reasons:
– Changes in intake –> average of 100mM K+ eaten per day, but starvation may decrease this
– Inability to absorb it –> inflammation of the bowel
– Excessive loss –> this can occur in vomiting/diarrhea
The K+ may also change in the body due to intracellular-extracellular shifts:
Extracellular:
– Dehydration –> increase in plasma osmolality causes cell shrinkage, so cells lose K+ in response
– Acidosis –> in acidosis, protons move into the cell where they are buffered by proteins, so K+ ions move outwards to compensate.
Intracellular:
– Hyperhydration
– Adrenaline –> this activates the Na/K-ATPase, which shifts potassium into cells
– Insulin –> activates the Na/K-ATPase and increases Na+ entry via the Na-glucose transporter.
Regulation of Potassium
The [potassium] can be regulated by controlling both internal balance and the external balance.
Internal:
There are specific feedforward responses to eating and exercise:
– When eating, insulin stimulates the Na/K-ATPase to drive potassium into cells.
– Adrenaline increases activity of the pump shifting K+ into cells, to stop becoming hyperkalaemic in exercise.
External:
– Long term K+ homeostasis requires the kidneys.
– However, potassium is freely filtered by the kidneys and reabsorption is unregulated
– Regulation of potassium is controlled by the principal cells in the late DCT which control secretion.
The sodium pump in basal membrane creates a sodium gradient
– Sodium then diffuses into the cell via ENaC channels from the lumen in order to balance the gradient.
– To balance the charge, potassium diffuses out via ROMK channels, and so it is excreted in the urine
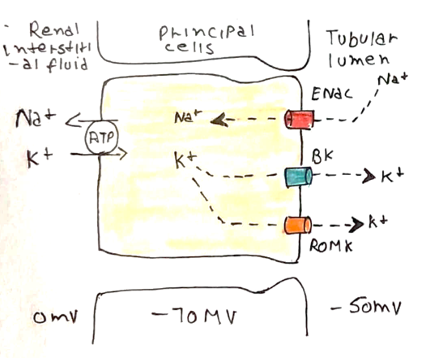
Control of K+ secretion is increased in 3 main ways:
i) High plasma [K+] – enhances transport into principal cells
ii) Aldosterone – stimulates synthesis of ROMK + ENaC channels and sodium pump density, increasing secretion
iii) High tubular flow rate – removes K+ in tubule allowing more secretion.
Consequences of High and Low potassium
Hypokalemia:
This hyperpolarizes the cell and reduces the excitability of nerve and muscle
– Leads to muscular weakness –> muscular paralysis + cardiac arrhythmias + lethargy.
– T waves disappear as cells repolarize slower and are replaced by U waves
Hyperkalaemia:
This is often due to renal failure where GFR drops below 20% to prevent excretion.
– Depolarizes cells bringing them closer to threshold, giving hyperexcitability
– Leads to cramps, spasms, diarrhea and increasing chances of cardiac arrhythmias (ventricular fibrillation)
– T wave gets larger as cells repolarize faster.


