UK graduate prioritisation
Dear Friend,
I hope you’re settling into 2026 well. This week, I want to unpack the Medical Training (Prioritisation) Bill — new legislation that’s stirring debate across UK medical training. It’s been making headlines and sparking heated discussion in corridors and WhatsApp groups alike, so this week I want to walk through what it is, why it’s being introduced, how it could affect doctors at different stages, and what the real pros and cons are.
What Is the Bill?
Put simply, this is emergency legislation introduced by the UK Government to prioritise certain groups of applicants for medical training posts — including the Foundation Programme and specialty training — in a way that gives UK medical graduates and other specified groups first access to available posts. It’s framed as a UK‑wide bill, developed with input from the devolved governments, and aims to reshape how doctors move from undergraduate training into postgraduate training.
Under current proposals:
Foundation programme offers in 2026 would be allocated first to UK graduates and those from a handful of European medical schools with reciprocal agreements.
Specialty training prioritisation would also favour UK graduates, Irish graduates, those who have completed (or are completing) UK training, and some doctors with specific immigration statuses.
International medical graduates (IMGs) can still apply — nothing in the legislation bans them — but they won’t be prioritised unless they fall into one of the specified priority groups
Why Now?
The Government’s justification for the Bill stems from a perceived mismatch between the number of UK‑trained doctors and the number of postgraduate training posts available.
Since visa restrictions were lifted in 2020, applications from doctors trained overseas have surged. In the 2025 recruitment cycle, there were thousands more overseas applicants than UK graduates competing for the same posts. Government analysis suggests that this rising competition has contributed to lower success rates for UK graduates, creating a bottleneck in career progression and workforce planning.

Pros of the Bill
There are some reasons it appeals to many clinicians:
Career progression security for UK graduates: By prioritising UK trainees, the system aims to reduce the risk of UK doctors finishing medical school but failing to secure a training number. That can end careers prematurely or push doctors out of training entirely.
Workforce planning: Better alignment between undergraduate output and postgraduate training could, in theory, create a smoother pipeline of doctors progressing through the NHS workforce, reducing reliance on unpredictable international labour markets.
Return on investment: Training a doctor in the UK is expensive. Prioritising UK graduates aims to ensure that investment feeds back directly into NHS care provision.
Cons and Concerns
Some of the downsides and open questions are significant:
International doctors’ contribution: IMGs make up a large and vital proportion of the medical workforce. Prioritisation could disadvantage doctors who have trained overseas but are committed to UK practice — especially those who have already invested years of service.
Equity and diversity: Because the demographic profile of UK and international graduates differs, prioritisation has the potential to affect workforce diversity — something the government’s own analysis acknowledges.
Does prioritisation fix the problem? Critics argue that prioritisation doesn’t solve the underlying shortage of training posts — it just redistributes them. If there aren’t enough posts overall, competition will remain intense even within the prioritised group.
Implementation nuances: The Bill’s actual impact depends on regulations that define “significant NHS experience” and how prioritisation stages are structured. That detail matters greatly for IMGs who have already been training or working in the NHS
What Happens Next?
Right now, this is a Bill — not yet law. It must pass through both Houses of Parliament, be debated, possibly amended, and receive Royal Assent before it can take effect. Only after that will implementation timelines and regulations be finalised.
As ever, if this affects you directly — be it in an ongoing application or a future career plan — the details matter. I’ll keep you updated as the Bill progresses and as implementation guidance becomes clearer.
Drug of the week
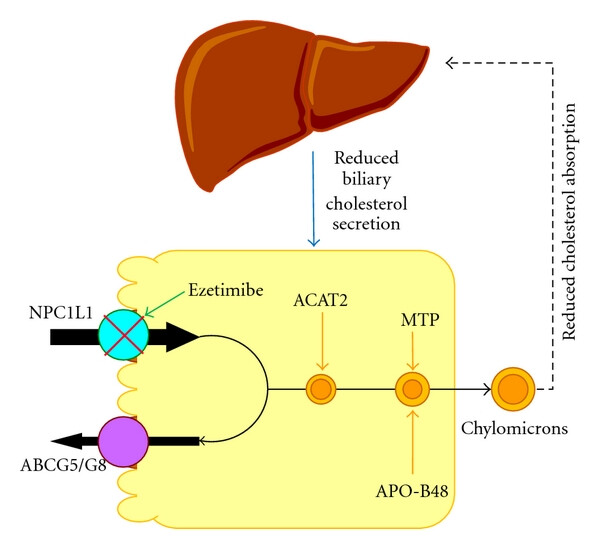
Ezetimibe
Ezetimibe is a cholesterol-lowering agent that targets intestinal absorption.
It’s used mainly to reduce LDL-cholesterol — often alongside a statin or in patients who can’t tolerate high-dose statins.
It blocks the NPC1L1 transporter in the small intestine, preventing dietary and biliary cholesterol from entering the bloodstream.
Because less cholesterol is absorbed, the liver increases LDL uptake — lowering circulating LDL levels.
On its own, it cuts LDL by roughly 15–20%; added to a statin, the reduction is greater.
Ezetimibe’s strength is its simplicity and tolerability — it’s a useful add-on when statins alone don’t hit targets. Its drawback is modest effect size compared with high-intensity statin therapy or other lipid-modifying drugs, so it’s not usually a first-line choice for high-risk patients without statins.
A Brain Teaser
A 64-year-old woman is brought to the emergency department after suddenly developing severe headache and double vision.
She has a history of poorly controlled hypertension and type 2 diabetes. On examination, her right eye is deviated down and out with ptosis. The right pupil is dilated and poorly reactive to light.
There is no limb weakness or sensory loss.
What is the most likely cause of her presentation?
A: Cavernous sinus thrombosis
B: Diabetic third nerve palsy
C: Intracranial aneurysm
D: Multiple sclerosis
E: Pituitary apoplexy
Answers
The answer is C – intracranial aneurysm.
This patient has an acute, painful third nerve palsy with pupillary involvement. The “down and out” eye position and ptosis indicate oculomotor nerve dysfunction, while a dilated, unreactive pupil strongly suggests compression of the superficial parasympathetic fibres of CN III.
The most classic cause of this presentation is a posterior communicating artery aneurysm, which can compress the oculomotor nerve and cause sudden onset diplopia and headache. This is a neurological emergency.



