Shortness of Breath
Try out this rheumatology case and test your clinical knowledge. The answers are at the bottom.
Questions
A 74-year-old woman presents to A&E with a 3-month history of persistent shortness of breath. She mentions that she used to be able to comfortably walk a mile to the shops but has now become even more breathless.
PMHx:
Rheumatoid Arthritis
Observations:
SpO2: 92%
Temperature: 36.9
BP: 117/82
HR: 73
RR: 24
Examination:
HS 1+2+0
Fine crepitations in bilateral upper zones
Some initial bloods are taken:
| Test | Result | Reference Range |
| Hb | 128 | 120 – 155 g/l |
| MCV | 89 | 82-100 |
| WCC | 11.7 | 4-11 x 109/l |
| Plts | 338 | 150 – 400 x 109/l |
| Anti-citrullinated cyclic peptide | 89 | < 20 EU/ml |
| Rheumatoid factor | 32 | < 20 IU/ml |
Q1: Which joints are classically affected in rheumatoid arthritis (Bonus – what simple examination maneuver is likely to support this diagnosis?)
An initial CXR is requested:
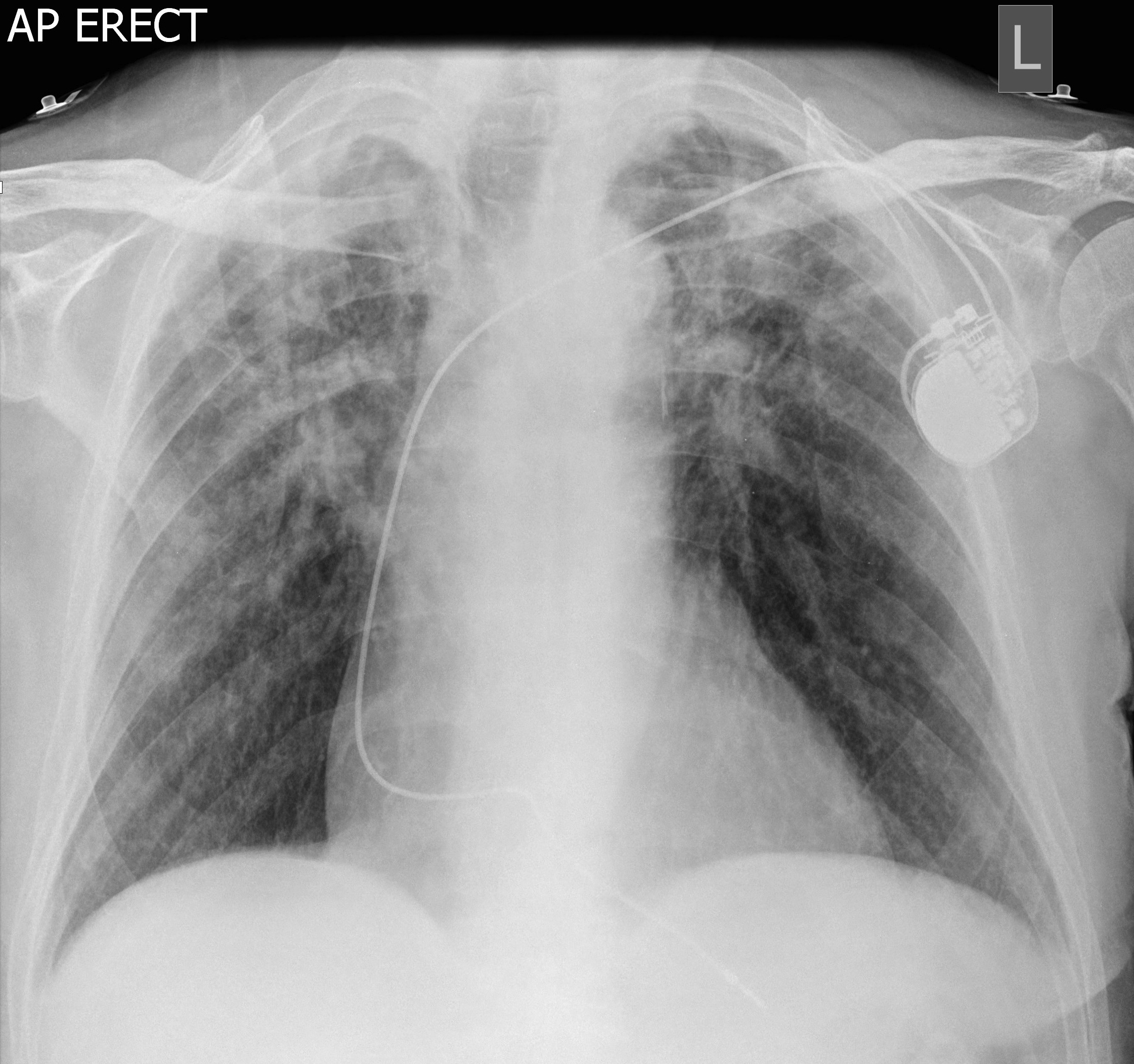
Q2: Interpret the CXR.
Q3: What are the different causes of upper and lower zone fibrosis?
Q4: What further investigations would support the likely diagnosis?
Answers
Reveal the Answers
RA classically symmetrically affects small joints including the AC joint and the small joints in the hand/foot – the MCP/MTP and PIP joints. This is in contrast to OA, which classically asymmetrically affects large axial joints e.g. hip/knee and the CMC and DIP joints in the hand.
RA Hand Signs | OA Hand Signs |
Swan-neck deformity (hyperextension of PIP and flexion of DIP) | Heberden node (DIP) |
Boutonniere deformity (flexion of PIP and hyperextension of DIP) | Bouchard Node (PIP) |
Z-thumb deformity (hyperextension of IP joints and flexion of MCP joint | |
| Ulnar deviation of fingers and wrist | |
Rheumatoid nodules (Extensor surfaces) |
The metacarpal/tarsal squeeze test is a simple test which involves squeezing the MCP joints – a positive test elicits pain and is indicative of RA
The CXR shows bilateral reticular-nodular patterning in both upper zones consistent with bilateral upper zone fibrosis. Also present – pacemaker (single lead)
Upper Zone – CHARTS | Lower Zone – BRAINS |
Coal Worker’s pneumonocosis (and any other pneumonocosis) | Bronchiectasis |
Hypersensitivity Pneumonitis | Rheumatoid arthritis |
Ankylosing spondylosis | Asbestosis |
Radiation fibrosis | Idiopathic pulmonary fibrosis |
Tuberculosis | Nitrofurantoin (and other drugs e.g. amiodarone, methotrexate, bleomycin) |
Sarcoidosis | Systemic Sclerosis |
Spirometry would be very useful, and would likely show a restrictive deficit (FEV1/FVC > 0.8 with a reduced TLC but increased RV)
A bronchio-alveolar lavage would also be helpful in ascertaining the cytology of any inflammatory cells in the lung – likely lymphocytic
The gold standard investigation would be a high-resolution CT Chest with contrast (viewed in the lung window) – this would likely show the presence of multiple rheumatoid pulmonary nodules and honeycombing in the upper lobe.
These findings would be consistent with a diagnosis of Caplan’s Syndrome – a form of pneumoconiosis associated with RA (NB – it is less likely to be simply RA-induced fibrosis due to presence of predominantly upper zone fibrosis)
To get more information about the conditions mentioned in this case including diagnosis and management, have a look at our free haematology notes on In2Med. Written by medical students, we have pitched them just at the right level to help you ace your exams.
Sources
Image 1: Case courtesy of Dr Ian Bickle, Radiopaedia.org. From the case rID: 50303
University of Cambridge
About The Author
Disclaimer



