Medical Ethics and Law
Medical Ethics and Law
This article goes through key ethical principles and medical laws to help you answer those challenging interview questions…
Introduction
This article is aimed at 6th form students who are looking to apply for medicine. This covers the key ethical principles and laws and how to apply them to help students in preparation for their medical interviews.
Ethics are principles that govern a person’s behaviour. You might have heard of the classic ethical dilemma- ‘You are watching a train about to kill 3 workers on a train track. Would you pull a lever to divert it, so it kills 1 person instead?’ Regardless of which option you choose, when a doctor is placed in an ethical dilemma it is important to have a framework for thinking about the arguments in support of and against the different options and come to a justified conclusion for yourself. Therefore, rather than learning all the endless ethical scenarios, this article will take you through the key ethical principles that can be applied to any scenario. Additionally, we will cover some fundamental aspects of medical law and then we will apply it to a few key cases.
Ethical Theory
The ethical theory we cover in this article is principlism, virtue ethics, deontology and consequentialism. Principlism is the most important theory to draw upon in interviews, however it is also good to be aware of the other ethical theories that preceded principlism.
Principlism – Four Principles of Medical Ethics
The most important ethical theory related to medicine is principlism. This was developed as a practical approach to ethical decision making. Rather than engaging in abstract debate about the idealistic approach, principlism is purported to offer a method of dealing with real-world ethical dilemmas.
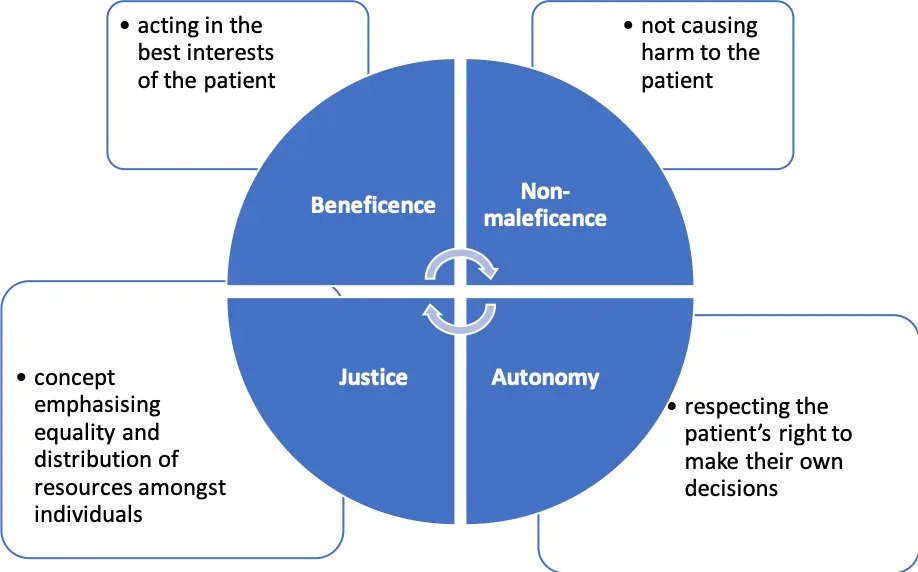
In a free society this autonomy is considered one of the most important principles. Doctors must always gain informed consent- where people must be fully informed before you ask for their consent for any procedure. You can only breach this principle in rare scenarios where patients are not deemed to have capacity (see medico-legal section).
*Tip: to stand out for any question that asks you about the value of a treatment you can mention QALYs- Quality Adjusted Life Years. This is a measure that NICE use to allocate resources and assess whether a treatment is beneficial for the cost that it incurs the NHS. A QALY measures the number of years of life that a treatment adds to a patient adjusted for the quality of health in those years. Therefore, a QALY of 1 is a year of life in perfect health or perhaps it is 2 years of life in 50% health etc. NICE then measures the cost per QALY. In general a for cost-per QALY of £20,000- £30,000 is considered acceptable.
General considerations of Principlism
In ethical scenarios often one principle will be at odds with another. For example:
Beneficence vs non-maleficence – Often acting in the best interests of patients causes harm to them.
Every treatment has side effects, there are risks in surgery, drugs have side effects, procedures can be painful such that in reality the practice of non-maleficence seems impossible. Therefore, doctors often have to balance beneficence with non-maleficence and ask do the benefits of an intervention outweigh the risks? They must then relay this information to patients so they can make an informed decision about what to do.
Beneficence vs autonomy – Sometimes patients may decide against a treatment despite us deeming that it is in their best interests.
Doctors are moving away from the paternalistic approach to medicine which involves the ‘doctor knows best’ mindset. It is the duty of doctors to act in the best interests of patients by fully informing them of the costs and benefits of different treatments. They must then respect a patient’s autonomy to make a decision based on this information. Occasionally the two principles may be at odds with each other if the patient declines what we deem as best interests e.g Jehovah’s Witness denying a blood transfusion. As long as the patient is competent then autonomy trumps beneficence.
Beneficence vs justice – In the current NHS doctors want to do the absolute best for each patient but realise that it is not possible with limited resources such as money and time.
For example, you may want to give your patient their optimal treatment, however, this may be expensive and not covered by the NHS. A junior doctor working in A&E may find that it is in the best interests of the patient with abdominal pain to be seen quickly, however they have one patient in a cardiac arrest, and another having an acute asthma attack, therefore doctors must prioritise to act in the best interests of all patients.
Non-maleficence vs justice – In the process of prioritising and resource allocating, doctors risk directly harming patients.
Doctors have to prioritise resources so that they cause as little harm as possible for the highest number of people. The trade-off is that some people e.g. the person with abdominal pain, may still be harmed if not seen quickly enough. This is the unfortunate tale of the NHS where services are being put under more and more pressure.
Non-maleficence vs autonomy – It is important to know that patients must give consent for, but cannot demand treatments that would harm them.
Sometimes a patient may demand a treatment that could be harmful to their health e.g. antibiotics for a viral infection. In this situation you would directly cause harm by giving a treatment and with limited resources patients cannot demand treatments that they are not eligible for.
Other ethical theories to be aware of
In an interview situation if you are given an ethical dilemma, reason your thoughts on it using the 4 principles of medical ethics. You should also be aware of the ethical theories- virtue ethics, deontology and consequentialism. They offer idealistic approaches to different situations.
Virtue Ethics
- This is the ethics where it is the character of the person that is important rather than the actions or consequences of the individual.
- Beauchamp and Childress (founders of principlism) have considered five virtues that every medical student and doctor should have: trustworthiness, integrity, discernment, compassion, and conscientiousness. It is not focused on the outcome of an action or on developing hard and fast rules for anything.
Deontology
- Deontology focusses on actions in themselves which are either right or wrong regardless of the consequence.
- This focusses on hard and fast rules (thou shalt- and thou shalt not). This includes things such as respecting autonomy, dignity and rights.
Consequentialism
- This is where the consequences of any given action determine whether what you have done is good or evil.
- Utilitarianism is where an outcome is optimal where there is the greatest happiness for the greatest number of people. This could require a minority suffering for the greater good of many.
Medical Law
Important issues to consider in medical law is consent & capacity, right to confidentiality as well as laws relating to abortion and euthanasia.
Consent and Capacity
Definition of informed consent: Consent is the agreement to do something after being informed about what it entails. Consent must be given by patients whether it is a physical examination, blood test or surgery. Consent may be non-verbal (e.g. holding out their arm for a blood test), verbal (e.g. consent for physical examination) or written down (e.g. before surgery).
Laws about consent: doctors must gain consent from patients before any procedure and should not do anything against patients’ wishes.
Therefore, informed consent should always be sought where possible. There are a few exceptions that do not require consent by law:
- If a patient does not have capacity…
- Doctors should assume that everyone has capacity unless there is evidence otherwise.
- If we suspect that the patient does not have capacity because they have an impairment of the brain or mind then we may proceed to do an assessment for capacity: The patient should be able to understand their decision, retain information about the decision, weigh up the pros and cons and communicate their decision.
- If a patient cannot do these things then a doctor should take all the necessary steps to help a patient reach capacity e.g. by explaining things in more simple terms.
- If the patient still lacks capacity then the doctor may act against the patients’ wishes under the Mental Capacity Act (2005), if it is in their best interest and acting in a way that is least restrictive to the person’s rights and freedom.
- Age…
- In children under 16, their capacity must be assessed (not presumed competent) but can consent to treatment without parental knowledge if deemed competent via the “Gillick Test”.
- To pass the Gillick test the child under 16 must have sufficient intelligence to fully understand what is involved in the proposed treatment, including its purpose, nature, likely effects and risks, chances of success and availability of other options.
- Like adults, 16-17-year-olds are presumed to be competent and can give consent. On the other hand, if 17 or under then refusal for treatment can be overridden by parental consent.
- Emergency situations…
- Another scenario where you need not gain consent may be in emergency situations where a patient is unconscious or obtaining consent would delay life-saving treatment.
Confidentiality
Confidentiality is the principle of respecting a patient’s right to privacy by not sharing their medical or personal details with anybody not involved in the care of the patient without their consent. This is a vital principle to uphold as the patient-doctor relationship is heavily built on trust.
On the other hand, doctors must break confidentiality in certain cases:
- Safe-guarding children
- Safe-guarding vulnerable adults
- The potential of harm to oneself or others
- Inability to safely operate a motor vehicle necessitates contacting the DVLA if the patient does not themselves
- Concerns of terrorism necessities notifying the police
- Doctors must notify the government of certain infectious diseases eg. HIV, TB, measles etc.
Abortion Law
Termination of pregnancy was decriminalised in 1967 in England, Scotland and Wales (not Northern Ireland).
- It states that termination of pregnancy is allowed under 24 weeks if continuance of the pregnancy would involve risk to the life of the pregnant woman, greater than if the pregnancy were terminated.
- In reality anyone under 24 weeks gestation is given an abortion if they request it as continuing to full-term is always considered riskier to the mother’s life than having an abortion. You must have permission from two medical practitioners.
- After 24 weeks abortion may be given if the mother is at risk of death or serious injury or if the child is at risk of being severe physical or mental abnormalities.
Euthanasia Law
Euthanasia is the act of deliberately ending a person’s life to relieve suffering which is illegal under UK law. Active euthanasia is deliberately intervening to end someone’s life whereas passive euthanasia refers to causing someone’s death by withdrawing or withholding treatment with the intent to shorten life.
In the UK, it is legal to withdraw life-saving treatment if it is in the person’s best interests and this is not considered passive euthanasia as the primary aim is not to shorten the person’s life but make them suffer less. Therefore, withdrawing treatment or giving treatment that inadvertently also shortens the life of a person can be a part of good palliative care (making sure the patient is comfortable) and is not euthanasia.
Euthanasia Law
- Dr Moor gave patients large doses morphine. This may have been with the intent to shorten the life of his patients, however in 1999, he was found not guilty of euthanasia as he could argue that the morphine was primarily to ease pain and not to kill.
- Additionally, Tony Bland who was in a persistent vegetative state after the Hillsborough disaster, had his feeding tube withdrawn but this was not considered murder as the tube was not considered to be the patient’s best interests.
- On the other hand, Dr Cox was charged with attempted murder in 1992 for administering a potassium chloride injection (stops the heart) to a patient with rheumatoid arthritis suffering from intense pain. Despite the patient having pleaded with the doctor to end her life and the sons thanking him, he was charged with attempted murder as potassium chloride does not have any analgesic effects so he could not claim he was using the doctrine of double effect. i.e the KCl injection had only one effect and that was to kill.
Example Cases
Now we come onto dealing with scenarios in the medical interview.
Avoid the pitfall of starting your answer with a strong opinion one way or the other. A better course of action is to first discuss arguments both for and against, before coming up with a balanced conclusion that appreciates the nuances of the scenario. This should be done, where possible, within the framework of the four pillars of medical ethics, including relevant laws and specific pros and cons of the scenario.
We will go through how you can structure your answer with some example questions:
Do you agree with abortion?
- For this scenario you will want to start by acknowledging that it is a complex issue with arguments on both sides.
- Then you may refer to the current abortion law in the UK. I.e it is legal under 24 weeks and after that time the laws become stricter such that there must be risk of severe disability of the child or risk to the life of the mother. In law the foetus does not have human rights till birth.
- Represent different views.
Pro-choice
- Women’s rights to be able to do what she wants with her own body
Pro-life
- Foetus is considered a human since conception and abortion is equivalent to murder.
Gradualist
- Late abortions as worse than early abortions.
- 24 weeks is the earliest point at which the foetus is considered to be viable and able to survive outside the womb and as such this is reflected in law.
- Finish with a conclusion such as: Overall, I agree with the gradualist view that the rights of the woman should be respected but that abortion should be avoided and carried out as early as possible.
Should euthanasia be legalised?
- To really stand out when answering this question, first demonstrate knowledge of UK law.
- Represent some of the views for and against before coming to a conclusion.
For euthanasia
Beneficence:
- Doctors have a duty to relieve suffering
- Compassionate
Autonomy:
- Doctors should respect a patient’s wish to die with dignity
- Patient is the only person who knows when life becomes too difficult to bear.
Justice:
- Frees up medical costs to help others.
Against Euthanasia
Non-maleficence:
- Duty not to kill
- We can use good palliative care as an alternative way to relieve patients’ suffering without intent to kill.
Autonomy:
- Euthanasia may become non-voluntary e.g. If legalised disabled/elderly may feel a burden and that it is their duty to ask to be euthanised.
Other points:
- Legalisation implies that some lives are not worth living.
- Slippery slope: may not be used just for the terminally ill.
- Example conclusion:therefore, this is a complex issue with valid arguments on both sides, however due to the slippery slope and potential for non-voluntary euthanasia I agree with the current UK law and we should optimise palliative care to act in the patient’s best interests.
Q1) A patient refuses treatment for a life-threatening condition. What are the ethical issues to consider?
In this question the interviewers have specifically asked you about the ethical issues you may want to consider and so it is the perfect opportunity to use the 4 principles of medical ethics as a framework for your answer.
Example:
- The key ethical issues to consider in this case is the patient’s autonomy, non-maleficence and beneficence.
- Patients are assumed to have capacity and so we must respect this patient’s autonomy, however we also have a duty not to cause harm to our patients and therefore obeying their wishes may be directly harmful.
- To mitigate against this, we may wish to delve deeper into the reasons why the patient is refusing treatment and if we are happy that they understand their decision then perhaps it is autonomy that must be respected first and foremost.
Q2) A patient refuses treatment for a life-threatening condition. What will you do as a doctor?
This question is a bit trickier and relies on one recognising that respecting the patient’s autonomy is of utmost importance and we can deny treatment only if they do not have capacity. Therefore, to tackle this question you may want to go through these steps:
- In any scenario where you are the doctor in a situation faced with a patient, the first step is always to explore a patient’s concerns. Before jumping to any conclusions, you need to take a step back and find out why they are refusing treatment for a life-threatening condition.
- This can then let you assess capacity – whether they understand their decision and the consequences of it.
- If it is clear that they do not understand the consequences of refusing treatment then you want to help the patient reach capacity.
- Do this by explaining the consequences of their decision.
- If the patient can understand the consequences, weigh up their decision, retain and communicate their decision then they have capacity and respect their wishes.
- On the other hand, if you have taken the necessary steps to help the patient reach capacity and they are still deemed not competent then act in the patient’s best interests, against their wishes.
- You should aim to give them the treatment which is least restrictive of their rights and freedom.
N.B if the patient was 17 or under then we may be able to override refusal with parental consent.
Q3) A patient is diagnosed with HIV and does not wish to tell their partner. What are the ethical issues to consider?
This scenario requires a consideration of the autonomy, non-maleficence, as well as confidentiality.
- Whilst we have to respect a patient’s right to make their own decisions (autonomy), we have to make sure their decision is informed. We should assess whether the patient understands the implications of their decision and why they do not want to tell their partner in the first instance.
- Secondly, we also have to consider confidentiality which should be respected where-ever possible to uphold the patient-doctor relationship. Exceptions to this are where other people could be harmed due to non-disclosure.
- Therefore, you have to weigh up benefits of not harming the other patient versus the damage done to trust by breaking confidentiality with this patient.
- In any cases where you are unsure it is always safe to say that whilst these are my thoughts it would be helpful to refer to the GMC’s ethical guidelines in cases like these.
Q4) What are the pros and cons of bariatric surgery?
Bariatric surgery is a treatment used for obese people to help them lose weight by making their stomach size smaller. It can reduce obesity and improve conditions such as diabetes and high blood pressure thereby having a beneficial effect on life expectancy.
- Consider the pros and cons taking first the principle of justice and then beneficence.
Pros
Justice:
- The surgery may improve quality of life and life expectancy so may be a good allocation of resources.
Beneficence:
- Doctors have a duty to act in the best interests of patients and for those with intractable obesity this may be the last option they have to lose weight.
Alternatives:
- Alternative options may have been exhausted or not acceptable to the patient.
Cons
Justice:
- The surgery is costly and has an opportunity cost. You have to consider justice and quantify whether the surgery is the best allocation of resources? What is the cost per QALY?
Beneficence:
- It could be argued it is not in the patient’s best interest as there are complications with any procedure and perhaps more conservative measures such as exercise and diet should be considered first.
Consider alternatives:
- Diet and exercise.
- Come to a conclusion: e.g. I would judge the intervention as acceptable based on the cost per QALY, alternatives available and the level of benefit versus harm it does to the patient.

University of Cambridge
About The Author



