End of my first rotation as a registrar
Dear Friend,
It’s hard to believe, but I’ve just completed six months in my first rotation as an oncology registrar. Somehow, it feels like the time has flown by, yet in many ways, it also feels like a lifetime of experiences has been packed into these months.
Looking back, it’s been intense. I’ve had on-calls, taken referrals from across the region, and made management plans for acutely unwell cancer patients. I’ve navigated new drugs, complex regimens, and emerging therapies. I’ve sat two exams that tested not just knowledge but stamina, and I’ve travelled to Barcelona for a preceptorship — a truly eye-opening educational experience. I’ve even learned a completely new skill in radiotherapy, which is a world of knowledge in itself. What I’ve loved most about all this is the variety the job offers. Every day is different; every patient brings a new challenge, a new story, and a new lesson.
That said, it hasn’t all been smooth sailing. Life outside the hospital has been just as challenging. I moved house, which alone would have been enough to throw anyone off balance. I was hospitalised during my very first week as a registrar, a humbling reminder that even doctors aren’t immune to illness. On top of that, I’ve been balancing a master’s degree, with essays and coursework piling up alongside clinical duties. And, of course, there’s the ever-present British weather, grey and dreary for large chunks of the last six months, which does little for morale.
It hasn’t always been comfortable, but reflecting now, I realise how much growth comes from stretching beyond your comfort zone. Every challenge, every late night, every patient encounter has been part of shaping how I think.
Next rotation is lung cancer
Looking forward, I’m moving onto lung cancer. This promises to be a very different experience. Compared to breast and prostate cancer, the patient demographic is distinct, and there’s often a clear causative factor — smoking. The drugs, protocols, and treatment pathways are different, and there’s a steep learning curve ahead. And yet, I’m looking forward to it. Partly because it’s new, partly because the variety keeps me engaged, and partly because I enjoy the process of learning and adapting.
I think that’s the bigger point I want to share this week. It’s easy to get caught up in the day-to-day pressures, head down in work, exams, and clinical decisions. But it’s important to pause, reflect, and acknowledge progress. Six months of intense clinical practice, learning, and personal challenges has taught me that even when things feel overwhelming, growth is happening.
That’s why I’m taking a week off to recharge before the next rotation begins. Not just to rest my body, but to reset mentally, to appreciate the progress so far, and to prepare for the challenges ahead. Hopefully the sun will cooperate, too — a small but welcome bonus.
Sometimes, we need to slow down to see how far we’ve come. For me, this week of reflection has reinforced that growth often happens quietly, between the chaos and the routine. And that taking the time to pause isn’t a luxury — it’s a necessity for the next stage of the journey.
Drug of the week
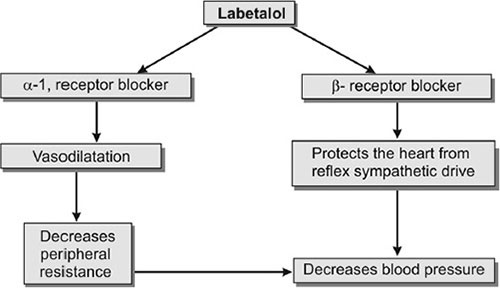
Labetalol
This is a drug which blocks β1-, β2-, and α1-adrenergic receptors.
That lowers heart rate and contractility. It also causes peripheral vasodilation.
Unlike pure beta-blockers, the added α1 blockade reduces systemic vascular resistance. Blood pressure falls without significant reflex tachycardia.
It is useful when controlled blood-pressure reduction is needed. It is used in chronic hypertension, hypertensive emergencies, and pregnancy.
Common side effects include postural hypotension, fatigue, and dizziness. Bradycardia and bronchospasm can occur. It may also mask hypoglycaemia in diabetes.
Its advantage is versatility. Its drawback is beta-blockade-related limitations, especially in asthma.
A Brain Teaser
A newborn is delivered at term following an uncomplicated pregnancy. He is feeding well and appears clinically normal. As part of routine postnatal care, a heel-prick blood sample was taken on day 5.
Two days later, the parents are contacted urgently because one of the screening results is abnormal. The baby is asymptomatic, but further testing confirms a markedly elevated phenylalanine level.
What is the most likely diagnosis?
A: Congenital hypothyroidism
B: Cystic fibrosis
C: Phenylketonuria
D: Galactosaemia
E: Sickle cell disease
Answers
The answer is C – phenylketonuria.
Phenylketonuria is an autosomal recessive disorder caused by deficiency of phenylalanine hydroxylase. This leads to accumulation of phenylalanine, reduced conversion to tyrosine and toxic effects on the developing brain.
Newborns with PKU are completely asymptomatic at birth.
That’s why the heel-prick (newborn blood spot) test exists. Without screening and early dietary restriction:
- Progressive intellectual disability
- Seizures
- Musty/mousy odour
- Eczema
- Microcephaly
An elevated phenylalanine level on newborn screening in a well baby is classic for PKU.
Why the other answers are wrong
A — Congenital hypothyroidism
Congenital hypothyroidism is also screened for on the heel-prick test.
However, it presents with elevated TSH and low T4
B — Cystic fibrosis
Cystic fibrosis is screened using immunoreactive trypsinogen (IRT).
Typical early features are meconium ileus, recurrent chest infections and failure to thrive
D — Galactosaemia
Galactosemia presents shortly after milk feeding begins. Symptoms include vomiting, jaundice, hepatomegaly, hypoglycaemia. The abnormality would involve galactose metabolism, not phenylalanine.
E — Sickle cell disease
Sickle cell disease is detected via haemoglobin electrophoresis.
Affected babies are usually well initially, but the abnormality involves haemoglobin variants — not amino acid levels.



