Should we cancel the junior doctor strike?
Dear Friend,
Hope you’ve had a week that hasn’t been too chaotic — I know how that feels around here.
This week, all conversations seem to be circling the resident doctors’ strike. Except now there’s a twist.
At the eleventh hour, the government has put a new offer to the BMA — a last-ditch bid to call off the strikes planned for December 2025.
And over the last few days that offer has been dissected, debated, and nervously refreshed more times than anyone can count.
So what’s actually on the table?
The offer — in plain terms
No movement on pay. There’s still no increase, no back pay, and no multi-year funded pay deal.
The government promises 4,000 new NHS jobs over the next three years — no breakdown by specialty, just a headline figure.
650 LED jobs would be converted into training posts.
Royal College exam fees would be covered in the future.
UK graduate prioritisation would be introduced via emergency legislation for the 2026 application cycle.
If you vote YES
The impending strikes will be called off.
There will be a formal referendum.
A yes vote will not cancel the re-ballot or end the disputes.
If you vote No
The impending strikes will go ahead
There will be ongoing negotiations
On paper, it’s something. It’s something the BMA can put to its members. And that’s where we are now — the result of that vote is due on Monday.

The case for calling off the strike
Let’s be honest — the timing is ugly.
The NHS is in the grip of one of the worst flu seasons in years. A&E departments are creaking. Staff are exhausted. Wards are full.
Walking into a planned strike now feels to many like kicking a hospital when it’s already down.
If calling off the strike means keeping beds staffed, ambulances off divert, and pressure off colleagues on the floor this winter — that’s a powerful argument. Especially when you hear from doctors who worry that another wave of absences could tip a fragile system into collapse.
But…
The problems with the offer
There’s real reason many doctors are hesitant.
Pay:
Nothing on real-terms restoration. No backdating. No multi-year deal. Not even Foundation Programme Review (FPR) levels. After years of erosion, that matters.
UK graduate prioritisation:
It’s being presented as a win… but the detail is absent.
How will it work for international medical graduates (IMGs)?
What about the promised two years’ experience before entry?
All we know is that legislation will be introduced — and Parliament can amend what it likes.
New jobs:
4,000 sounds big. But no clarity where they’ll be, when they’ll start, or how long they’ll last.
And if they’re temporary or poorly defined, they won’t solve the workforce crisis — they’ll just dress it up.
650 LEDs to training posts:
Again, no explanation of mechanism. Local processes with vague criteria risk exploitation and could inadvertently lower training standards.
In other words: the offer has promise on paper, but very little concrete detail.
So where does that leave us?
Come Monday, NHS resident doctors in England will have a choice:
Say Yes and pause strike action in hopes this offer delivers.
Say No and keep the pressure on — but risk a winter of industrial action in an already fragile system.
No one’s taking this decision lightly.
There are worries about patient safety. There are worries about fairness. There’s frustration about another year of being asked to choose between standing firm for the profession and stepping back for the system’s sake.
If you’re voting this weekend — I’m with you in spirit.
And if you’re watching this from the side, unsure what the result will mean for your rota, your patients, or your career — you’re not alone.
We’ll all know the outcome on Monday.
Drug of the week
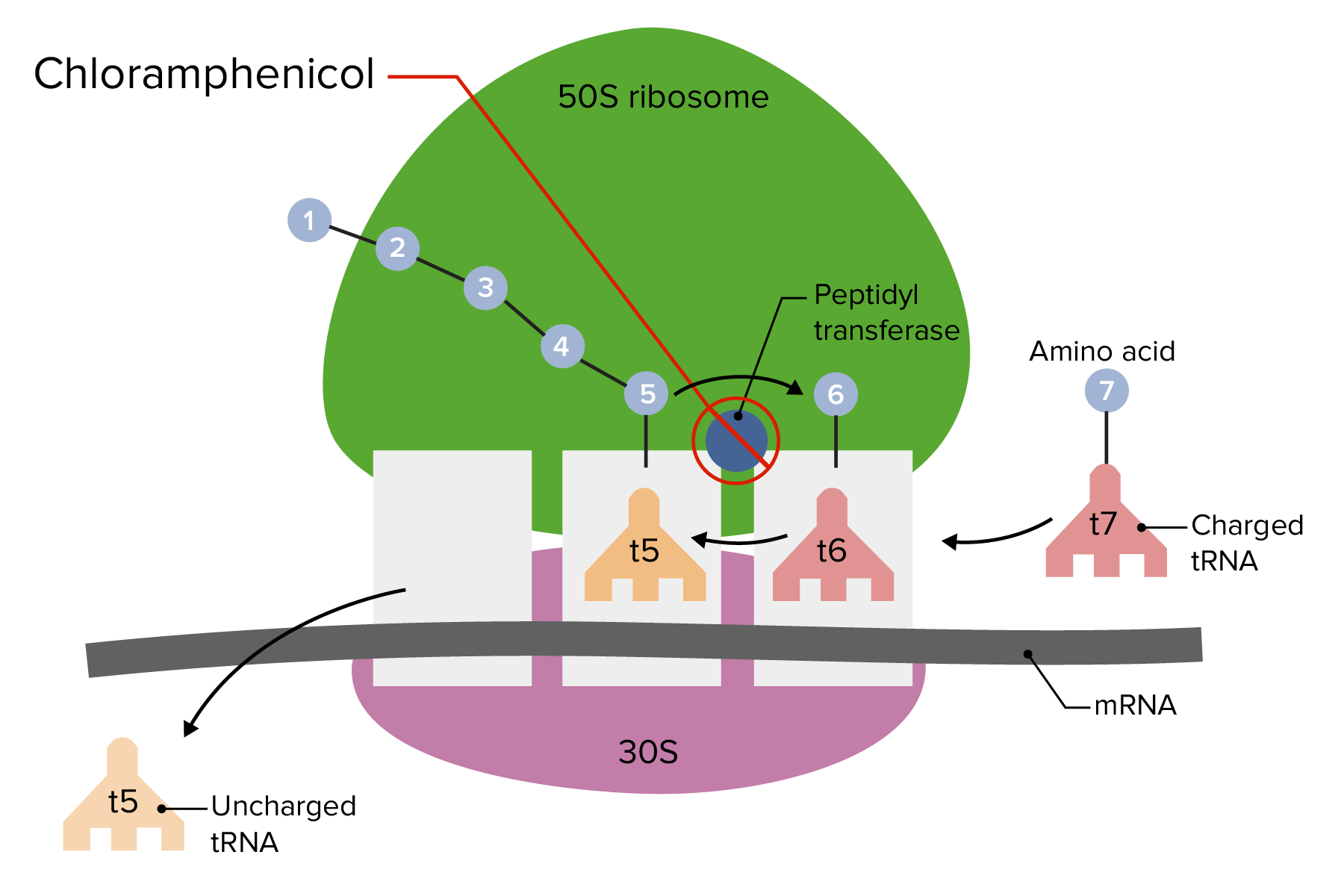
Chloramphenicol
Chloramphenicol is a broad-spectrum antibiotic reserved for serious infections when safer options won’t work.
It blocks bacterial protein synthesis by binding the 50S ribosome and stopping peptide formation.
It penetrates tissues well—including the CNS—making it useful for select life-threatening infections.
It can be given orally, IV, or as eye drops/ointment, though systemic use is limited.
Common side effects include GI upset and reversible bone-marrow suppression.
Its biggest risk is idiosyncratic aplastic anemia, which is rare but often fatal.
High doses can also cause dose-related marrow toxicity and “gray baby syndrome” in neonates.
It inhibits CYP450 enzymes, so drug interactions are common.
Because of these risks, chloramphenicol is used only when absolutely necessary.
A Brain Teaser
A 70-year-old woman was brought to the emergency department after suffering a fall. On examination, her right hip was externally rotated and shortened. She had a past medical history of deep vein thrombosis in her left leg 30 years ago. The initial hip X-ray showed an extracapsular intertrochanteric fracture of the proximal femur.
What is the most appropriate treatment?
A: Total hip replacement
B: Hemiarthroplasty
C: Non-surgical therapy
D: Intramedullary nail
E: Dynamic hip screw
Answers
The answer is E – dynamic hip screw.
Total hip replacement and hemiarthroplasty may be considered if the fracture is intracapsular. Non-surgical therapy is inappropriate as this requires her to be bedbound, which puts her at risk of another DVT. Intramedullary nail is typically used for other extracapsular hip fracture types (reverse oblique, transverse, or subtrochanteric type) and femoral shaft fracture.



