Difficulty Urinating
Try out this urology case and test your clinical knowledge. The answers are at the bottom.
Questions
A 67-year-old man presents to his GP with a 2-month history of difficulty urinating. He reports that he often dribbles at the end of urination, and it feels like he can never fully empty his bladder. He denies any haematuria or significant weight loss.
PMHx:
Hypertension
Observations:
SpO2: 99%
Temperature: 36.7
BP: 152/99
HR: 91
RR: 16
Examination:
Abdomen SNT
POC Bladder US: 500 ml pre-void, 298 mls post-void
Good anal tone
Enlarged prostate
Q1: How should the GP manage this patient initially?
The GP manages the patient appropriately and awaits the blood results (shown below):
| Test | Result | Reference Range |
| Hb | 89 | 120 – 155 g/l |
| MCV | 94 | 82-100 |
| WCC | 7.2 | 4-11 x 109/l |
| Plts | 293 | 150 – 400 x 109/l |
| Total PSA | 4.2 | < 2 ng/ml |
| Free PSA | 0.19 | N/A |
Q2: Comment on the blood results. How should the GP manage the patient now?
Q3: Which investigations are likely to be performed in secondary care?
The patient undergoes radical treatment and is given all clear. 5 years later he presents to A&E with a dragging right foot and numbness on the left side of his perineal area. An urgent MRI is performed:
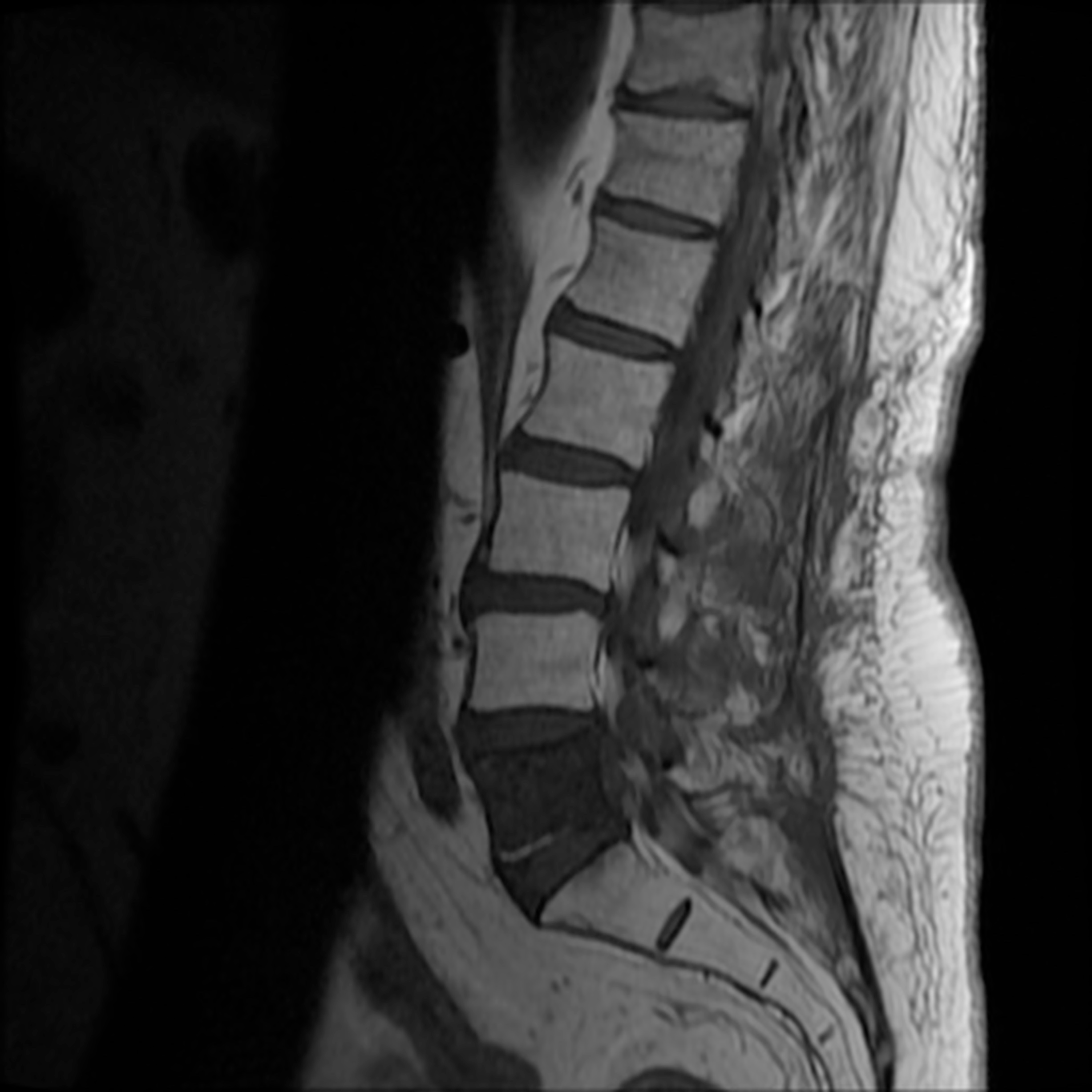
Q4: Comment on the MRI. What complication has developed?
Answers
Reveal the Answers
| Storage/ Irratative | Voiding / Obstructive |
| Frequency | Hesitancy |
| Urgency | Hesitant flow/ Weak stream |
| Dysuria | Straining |
| Nocturia | Dribbling |
| Urge incontinence | Incomplete emptying |
Regardless, the GP should perform urinalysis to exclude microscopic haematuria (which might indicate bladder/upper RT pathology/UTI/stones) and to check for hypertensive proteinuria. The most important test however would be to check the patient’s PSA levels, which will help to identify whether the issue is related to the prostate.
The elevated PSA highlights that the pathology is related to the prostate e.g. BPH, prostatitis, malignancy. However, the low free PSA and the normocytic anaemia is an indicator that the diagnosis is concerning for a malignancy. Furthermore, the CKS guidelines indicate that a free PSA > 3.0 ng/ml in patients from 50-69 must be investigated as a potential malignancy. The patient should be referred on a 2WW to urology.
The gold standard investigation in secondary care is a multiparametric pelvic MRI to assess the cancer itself but also lymph node, tissue and potential bladder wall involvement. This is often followed up with a trans perineal/transrectal ultrasound which takes guided ‘core’ biopsies of the sample (this approach is only possible as most cancers begin in the peripheral zone of the gland, which is closest to the intestines). A further CT of the abdomen and pelvis will help to stage the malignancy and highlight any extra-perineal disease
This is a Sagittal T1 (CSF is dark, cord difficult to see) MRI of the spine. The L5 vertebrae has an extensive sclerotic lesion (in a T1 spinal MRI, sclerotic lesions are dark). This is a classic finding of vertebral metastasis arising from a prostate adenocarcinoma, leading to secondary cauda equina and bilateral lower limb LMN and sensory neurological symptoms.
Sources
Image 1: Case courtesy of Dr Angel Donato, Radiopaedia.org. From the case rID: 59151
University of Cambridge
About The Author
Disclaimer



