The other 8 hours…
Dear Friend,
I hope you’ve had a good week. This week I found myself thinking about something that sits slightly outside medicine, but probably shapes my day more than anything inside it.
Arnold Bennett called it “the other 8 hours” in his book How to Live on 24 Hours a Day. It’s a simple idea. A day is 24 hours. Eight are for sleep. Eight are for work. That leaves eight hours that are, in theory, yours. It’s one of those ideas that sounds almost naive until you try to live it.
How the 8 hours look in my head
If I think about my own routine, those hours tend to fall into a loose structure rather than a fixed plan.
Some of it is the gym. Not every day, but enough that it feels like a regular anchor in the week. Something physical that breaks up the mental side of work.
Some of it is cooking. Usually simple meals after a long day. It’s rarely elaborate — more a transition than anything else, a way of marking the shift out of work mode.
And then there’s the rest of it. Downtime. TV, scrolling, sitting without doing much in particular. Nothing especially intentional, just recovery in whatever form it takes.
On paper, it feels like balance.
How it actually looks
The issue is that the “8 hours” assumes a clean separation between work and everything else.
In reality, I’m probably working closer to 10 hours most days once you include clinics, study, admin, and the small things that spill over into the evening. Even when I’m not actively working, there’s often a background layer of thinking about work that doesn’t fully switch off.
Once you factor that in, those 8 hours shrink to something closer to 6.
And they don’t arrive fresh. They arrive after a long day.
What changes when time shrinks
This is the part I didn’t fully appreciate until recently.
Those remaining hours aren’t neutral. They’re shaped by what came before them.
The gym becomes less about pushing progress and more about maintaining routine. Cooking becomes functional rather than enjoyable most of the time. Even rest can feel slightly passive — not restorative in the idealised sense, but just recovery from the day.
So the time is there, but the quality of it changes.
And that gap between “time available” and “energy available” is where most of the tension sits.
What this means for medical students
I think this becomes especially relevant during medical school, where the workload doesn’t always respect boundaries.
It’s easy to underestimate how much time the course actually takes, especially when you include revision, placement, and the mental load of constantly keeping up.
So the first practical point is simple: be honest about time. Not in a theoretical sense, but in a weekly sense. If your day is closer to 9–10 hours of study and work, plan around that reality rather than an idealised version of it.
The second is to protect small anchors rather than trying to optimise everything. For most people, that might be exercise, meals, or a fixed period of proper rest. Not everything needs to be maximised — some things just need to stay consistent.
And the third is to accept that “free time” after a heavy day won’t always feel like free time. Sometimes it will just feel like recovery. That doesn’t mean it’s wasted — it’s part of the system working as it should.
Final thoughts
Arnold Bennett’s idea still holds up, but not in the literal way it’s often presented.
It’s not really about finding 8 hidden hours in the day.
It’s about recognising that the time you actually have after work is smaller, more fragmented, and lower energy than it looks on paper — and planning your life around that version of reality instead of the ideal one.
Drug of the week
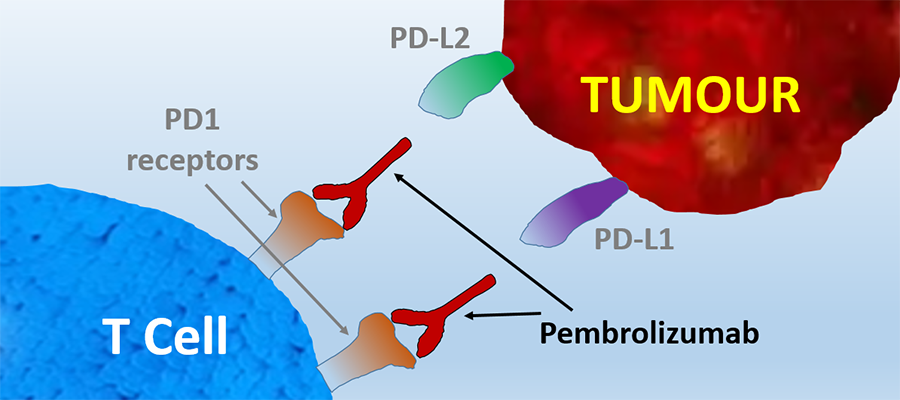
Pembrolizumab
Pembrolizumab is a monoclonal antibody and immune checkpoint inhibitor used in a range of cancers including melanoma and non-small cell lung cancer.
It works by blocking the PD-1 receptor on T cells, preventing tumour-induced immune suppression and enhancing anti-tumour activity.
It is often used as monotherapy or with chemotherapy, guided by factors such as PD-L1 expression.
Common side effects include fatigue, rash, and diarrhoea.
Immune-related adverse events can occur and may affect multiple organs, including the lungs, liver, and endocrine system.
These may require immunosuppressive treatment.
Pembrolizumab can cause severe toxicity and requires careful monitoring.
A Brain Teaser
A 29-year-old woman, G1P0, attends the antenatal clinic at 30 weeks’ gestation. She reports reduced fetal movements over the past 24 hours.
Her pregnancy has been uncomplicated so far. She has no significant past medical history and takes only routine antenatal vitamins.
On examination, her fundal height measures 28 cm. Her blood pressure is 118/72 mmHg. Urinalysis is normal.
What is the most appropriate next step in management?
A. Reassure and advise monitoring at home
B. Arrange an urgent ultrasound scan
C. Perform cardiotocography (CTG)
D. Induce labour
E. Start oral corticosteroids
Answers
Answer is C – Perform cardiotocography (CTG)
Reduced fetal movements after 28 weeks’ gestation should be assessed promptly with cardiotocography to evaluate fetal wellbeing. CTG provides immediate information about fetal heart rate patterns and can identify signs of distress.
Ultrasound may be required subsequently, particularly if there are concerns about fetal growth or amniotic fluid volume, but CTG is the first-line investigation.
Reassurance alone is inappropriate given the presenting symptom.
Induction of labour is not indicated without evidence of fetal compromise.
Corticosteroids are used when preterm delivery is anticipated, which is not currently the case.



