Is UK graduate prioritisation fair?
Dear Friend,
I hope you’ve had a good week. This week, I want to look at the real-world impact of the UK’s emergency medical training prioritisation legislation, which is now clearly affecting recruitment outcomes. We’ve moved from discussion to reality — offers are being made, and for some, not made.
What Is the Bill?
In simple terms, this legislation allows recruitment bodies to prioritise certain groups of applicants when allocating training posts. It doesn’t prevent anyone from applying.
But it changes the order in which candidates are considered, meaning some groups are offered posts before others are reviewed.
Why Was It Introduced?
The main driver is the mismatch between applicant numbers and available training posts. Applications — particularly from international medical graduates — have risen significantly in recent years, while training posts have not increased at the same rate.
This has created a bottleneck, particularly affecting UK graduates trying to progress into training.
Who Was Prioritised in 2026?
In this recruitment cycle, prioritisation broadly worked in tiers.
Higher priority was given to:
- UK medical school graduates
- Graduates from the Republic of Ireland
- Doctors who have completed, or are currently in, UK Foundation training
- Applicants with established UK residency rights (e.g. settled status or indefinite leave to remain)
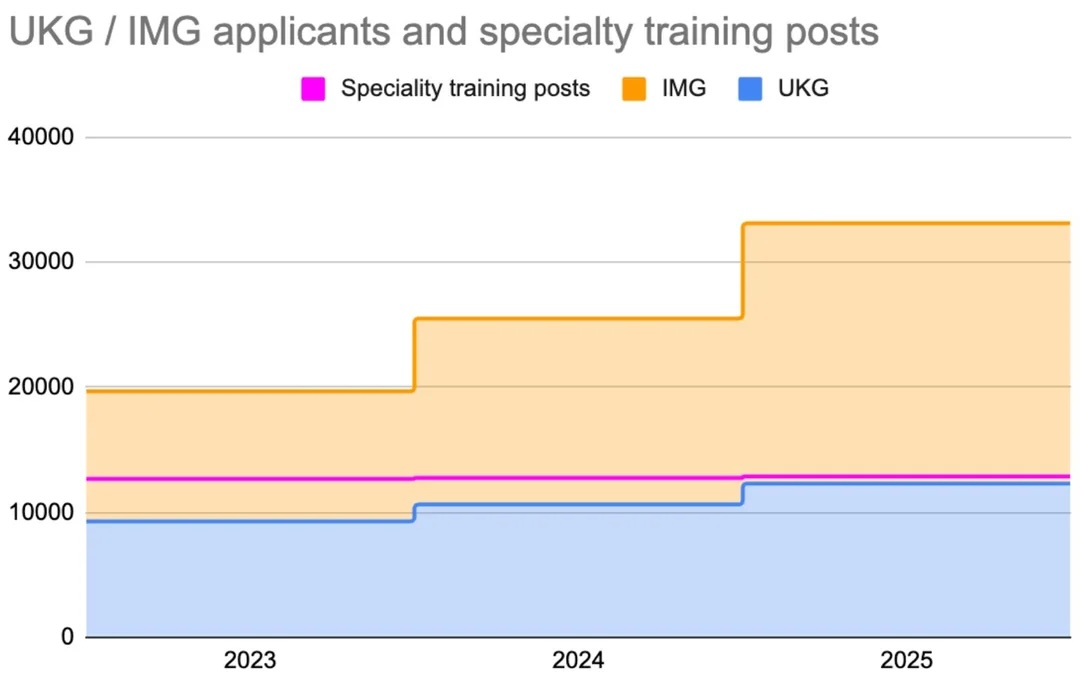
What Are We Seeing in Practice?
Over the past week, I’ve seen many LinkedIn posts from doctors celebrating securing the jobs they applied for — a huge milestone. At the same time, I’ve also seen international graduates, including some ranked in the top 100 for IMT, who have not received offers. That contrast highlights the shift: ranking alone is no longer the deciding factor.
What Options Are Left?
For those without offers, the path is uncertain. Some will stay and reapply, building further NHS experience. Others may take non-training roles to strengthen their portfolio. And for some, there is the question of whether to return home or look elsewhere. It’s also unclear whether future cycles will be any easier if post numbers remain limited — particularly if prioritisation becomes stricter.
What Changes for 2027?
The 2027 cycle is expected to formalise and tighten this prioritisation approach.
Current proposals suggest:
- A clearer, more rigid definition of priority groups, reducing flexibility in how applicants are reclassified
- Greater emphasis on completion of UK training pathways (e.g. Foundation Programme) rather than NHS experience alone
- Less scope for NHS experience by itself to move applicants into higher priority tiers
- More consistent national application of prioritisation rules across specialties
In practice, this may mean that simply gaining NHS experience in a non-training role is less likely to significantly change an applicant’s priority status compared to 2026.
Final Thoughts
There are arguments on both sides. Some will see this as necessary to support UK graduates and workforce planning. Others will see it as disadvantaging doctors who have already contributed to the NHS.
Both perspectives exist. To be honest, I currently do not know which side of the fence I sit on. All I can say it good luck to everyone applying.
Drug of the week
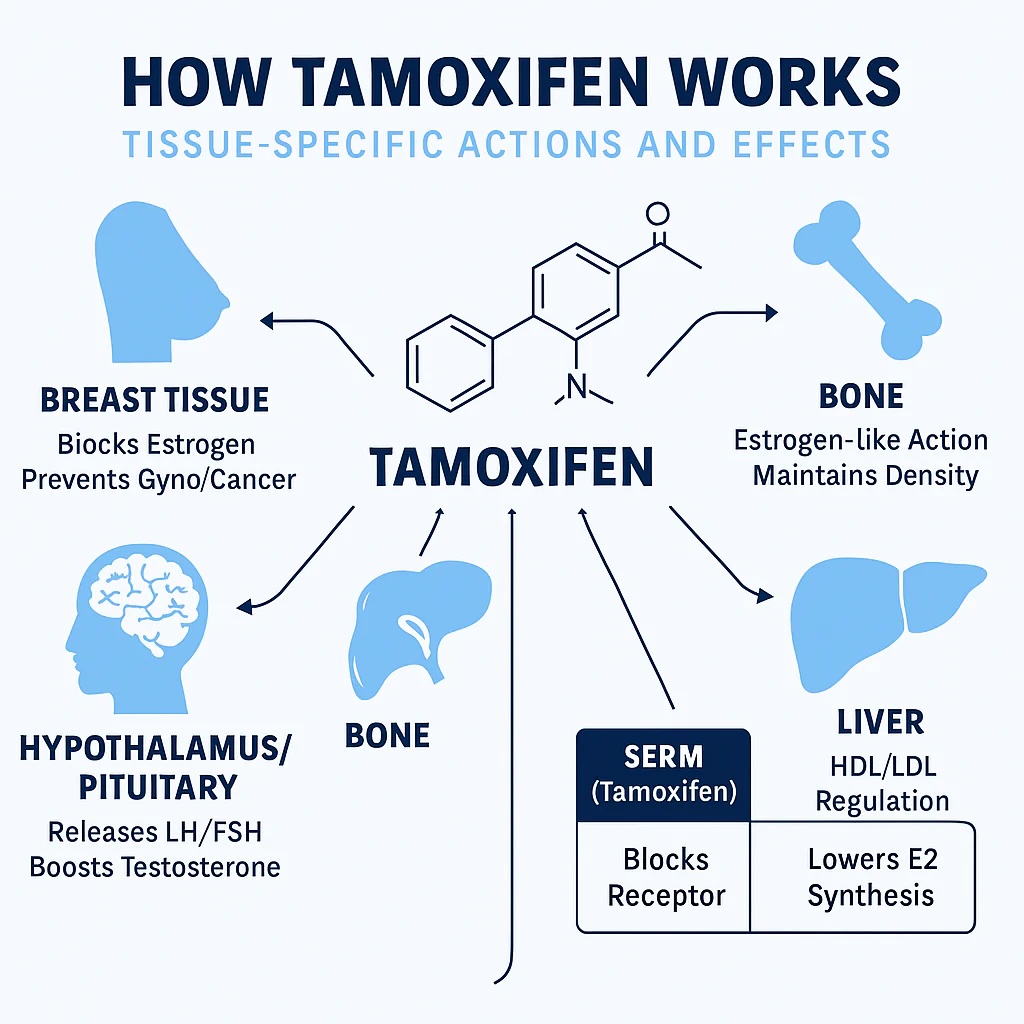
Tamoxifen
Tamoxifen is a selective oestrogen receptor modulator which is used in oestrogen receptor-positive breast cancer.
It works by competitively binding to oestrogen receptors in breast tissue, where it acts as an antagonist and reduces oestrogen-driven tumour growth.
In other tissues, such as bone and the endometrium, it has partial agonist effects.
It is commonly used as adjuvant endocrine therapy following surgery and may also be used for breast cancer prevention in high-risk patients.
Common side effects include hot flushes, nausea, menstrual irregularities, and vaginal discharge.
Venous thromboembolism can occur, particularly in patients with additional risk factors.
There is also an increased risk of endometrial hyperplasia and endometrial cancer due to its oestrogenic effects on the uterus.
A Brain Teaser
A 24-year-old woman presents to her GP describing a pattern of behaviours that she says are “taking over” her life. Over the past year, she has developed an intense fear of contamination, particularly from surfaces in public places, which has led her to wash her hands repeatedly throughout the day, often for several minutes at a time, until they feel “just right.”
She is aware that these fears are excessive and says she feels embarrassed discussing them, but she cannot resist the urge to perform these rituals, as doing so temporarily relieves her anxiety. Recently, the frequency of her handwashing has increased to the point that she is late for work most days and has begun avoiding social situations altogether.
She has no past psychiatric history, takes no medications, and is otherwise physically well.
What is the most appropriate first-line management?
A. Reassurance and review in 4 weeks
B. Start diazepam as needed
C. Refer for cognitive behavioural therapy with exposure and response prevention
D. Start low-dose haloperidol
E. Admit for inpatient psychiatric care
Answers
The answer is C – Refer for CBT
This is textbook OCD:
- Obsessions → contamination fears
- Compulsions → repetitive handwashing
- Insight preserved → “I know this is excessive”
- Functional impairment → work + social life affected
First-line = CBT with exposure and response prevention (ERP)
Where people slip:
- B (diazepam): treats anxiety symptomatically, not the disorder
- D (haloperidol): wrong mechanism, wrong indication
- A (reassurance): she’s already deteriorating
- E (admission): too extreme unless severe risk



