McClelland’s Human Motivation Theory
Dear Friend,
This week, I’ve been thinking a lot about motivation — what drives us, how we learn, and how we get the most out of ourselves and others. It reminded me of McClelland’s Human Motivation Theory, a framework I first came across years ago but that feels increasingly relevant, especially in medicine.
What is McClelland’s Theory?
David McClelland, a psychologist working in the mid-20th century, proposed that people are primarily motivated by three key needs:
Achievement (nAch) – the drive to excel, solve problems, and accomplish challenging tasks
Affiliation (nAff) – the desire for social connections, relationships, and a sense of belonging.
Power (nPow) – the wish to influence, lead, or make an impact on others.
McClelland developed this theory by observing adults in work and social settings. He noticed patterns in behaviour and achievement, and conducted research using projective tests and interviews to identify which of these needs predominated in different individuals. Over decades, evidence has supported the idea that our dominant motivational needs influence how we work, learn, and interact with others.
Why does this matter for medical students?
Medicine is a challenging field. Understanding what drives us can help us learn more effectively. For example:
If you’re achievement-motivated, you may thrive in environments with clear goals, frequent feedback, and opportunities to tackle complex problems.
If affiliation drives you, learning in collaborative settings — group tutorials, study partnerships, or supportive ward teams — may keep you engaged.
If power motivates you, you might enjoy leadership opportunities, taking responsibility for projects, or mentoring junior colleagues.
Reflecting on your motivational profile helps you identify the environments where you learn best and understand why some situations feel energising while others feel draining.
And what about leading a team?
As you move through your career, medicine isn’t just about personal learning — it’s about working with, and sometimes leading, teams. McClelland’s framework can help here too:
Recognise that different team members are motivated by different needs.
Achievement-driven individuals might excel when given challenging tasks.
Affiliation-driven colleagues thrive in collaborative, supportive environments.
Power-driven team members can be given leadership roles or responsibilities to channel their drive positively.
Using this insight as a doctor isn’t just “management theory” — it’s practical patient care. Teams that are motivated, engaged, and aligned perform better, make fewer errors, and ultimately improve patient outcomes.
Why reflection matters
Understanding motivation is not just about managing others. It’s about understanding yourself. Medicine is a long journey, and knowing what truly drives you can make the difference between surviving your training and thriving through it.
Next time you feel frustrated with a rotation, a study group, or a team, ask yourself: Which need is being met here? Which need isn’t? Sometimes a small change — a new challenge, a supportive colleague, a leadership opportunity — is all that’s needed to feel engaged again.
Drug of the week
Etoposide
Etoposide is a cytotoxic chemotherapy drug. It’s used in small cell lung cancer, testicular cancer, and some lymphomas.
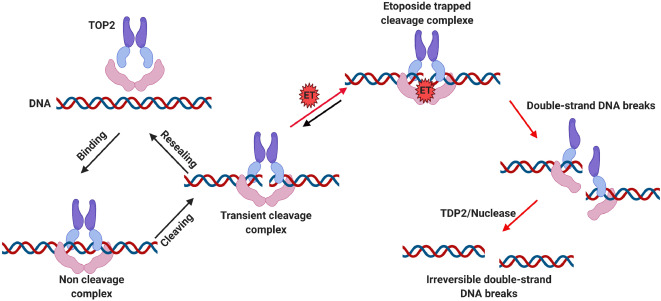
It inhibits topoisomerase II, and enzyme which helps unwind DNA during replication.
By blocking it, etoposide causes double-strand DNA breaks. Cells cannot progress through the S and G2 phases. Rapidly dividing cells are most affected.
It’s often combined with cisplatin in regimens like EP.
The main side effect is myelosuppression, especially neutropenia. Other common effects include nausea, alopecia, and mucositis.
A rare but serious long-term risk is therapy-related acute leukaemia.
Its strength is its effectiveness in chemo-sensitive tumours. Its limitation is bone marrow toxicity, which often limits dosing.
A Brain Teaser
A 52-year-old woman presents with a 6-month history of joint pain and stiffness, mainly affecting her hands and wrists. She reports morning stiffness lasting over an hour. On examination, there is swelling and tenderness of the MCP and PIP joints.
Laboratory tests are ordered to help confirm the diagnosis.
Which of the following is the most specific test for diagnosing rheumatoid arthritis?
A: Erythrocyte sedimentation rate (ESR)
B: C-reactive protein (CRP)
C: Rheumatoid factor (RF)
D: Anti-cyclic citrullinated peptide (anti-CCP) antibodies
E: Antinuclear antibody (ANA)
Answers
The answer is D – anti-CCP antibodies.
Anti-CCP antibodies are highly specific for rheumatoid arthritis (RA).
They can be positive early in the disease, sometimes before clinical symptoms appear.
Their presence also predicts more severe, erosive disease.
Why the other options are less specific
A: ESR – Non-specific marker of inflammation; elevated in many conditions.
B: CRP – Also a non-specific inflammatory marker.
C: Rheumatoid factor (RF) – Less specific; can be positive in other autoimmune diseases or infections.
E: ANA – Associated with systemic lupus erythematosus, not RA.



