Oncology preceptorship
Dear Friend,
This week, I had the opportunity to step out of my usual routine and travel to Barcelona for a preceptorship in bladder cancer. It was a two-day educational programme, fully funded — flights, accommodation, and food included — and focused on understanding both the current landscape and future direction of bladder cancer diagnosis and management.
What does a preceptorship actually mean?
A preceptorship is a structured educational experience, usually aimed at clinicians with a specific interest in a field. Rather than being a large conference, it’s typically small, focused, and interactive. The emphasis is on learning directly from experts, discussing real-world cases, and understanding how evidence translates into day-to-day practice.
In this case, the programme involved listening to international speakers, reviewing emerging data, and exploring how new diagnostics and therapies are shaping bladder cancer care.

Why are these common in oncology?
Oncology is a fast-moving specialty, and keeping up with evolving evidence is a constant challenge. Because of that, there are a number of educational opportunities like this, often supported or endorsed by professional bodies such as ESMO (the European Society for Medical Oncology).
These societies play an important role in setting standards, sharing best practice, and creating spaces where clinicians can learn outside of their usual healthcare systems.
The real value of these events
Beyond the formal teaching, one of the biggest benefits is networking. Sitting in a room with clinicians from different countries, healthcare systems, and training backgrounds gives you a broader perspective. You realise quite quickly that the same condition can be approached in subtly — and sometimes significantly — different ways depending on resources, guidelines, and patient populations.
It’s a reminder that medicine isn’t practised in a vacuum, and that there’s always something to learn from how others do things.
And a chance to see somewhere new
There’s also a human side to these trips. Being in a different city, even briefly, helps break the rhythm of clinical life. I managed to get out in Barcelona and finally see the Sagrada Família — something I’d somehow missed on previous visits. Stepping away from the hospital and into a place like that was a reminder of how valuable it is to occasionally pause and look outward.
Overall, the week was a privilege — educationally, professionally, and personally. Experiences like this don’t just update your knowledge; they broaden how you think about medicine, training, and the kind of clinician you want to be.
Drug of the week
Lercanidipine
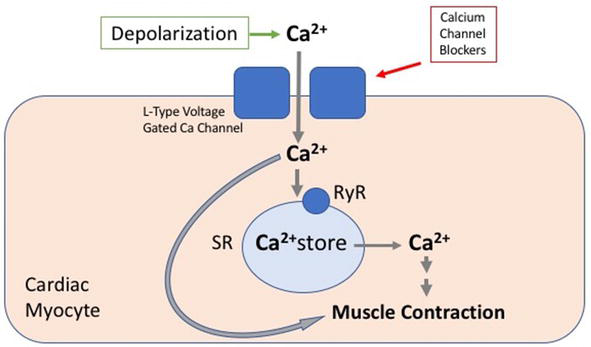
It blocks L-type calcium channels in vascular smooth muscle, leading to vasodilation and reduced peripheral resistance.
Compared with older dihydropyridines, it’s more lipophilic and longer-acting. That gives smoother blood-pressure control and less reflex tachycardia.
Common side effects include headache, flushing, dizziness, and ankle oedema.
Its advantage is better tolerability for some patients; its drawback is that oedema still limits use, and it has no role beyond blood-pressure control.
A Brain Teaser
A 68-year-old man presents to his GP with painless visible haematuria.
He has a 40-pack-year smoking history and worked in the dye industry for many years. He has no dysuria or urinary frequency. Physical examination is unremarkable.
Urinalysis confirms haematuria but is negative for infection.
What is the most likely underlying diagnosis?
A: Renal cell carcinoma
B: Transitional cell carcinoma of the bladder
C: Prostate cancer
D: Squamous cell carcinoma of the bladder
E: Acute glomerulonephritis
Answers
The answer is B – TCC of the bladder.
Painless visible haematuria in an older patient is bladder cancer until proven otherwise. The most common type of bladder cancer in the UK and other high-income countries is transitional cell carcinoma (also called urothelial carcinoma). Major risk factors include cigarette smoking and exposure to aromatic amines used in industries such as dye manufacturing. Patients often present with intermittent painless haematuria, with no signs of infection.
Why the other options are wrong
A: Renal cell carcinoma
Can cause haematuria but more commonly presents with flank pain, a renal mass, or systemic symptoms. Occupational dye exposure points more strongly toward bladder cancer.
C: Prostate cancer
Rarely presents with visible haematuria. More typical features include urinary obstruction, bone pain, or incidental PSA elevation.
D: Squamous cell carcinoma of the bladder
Associated with chronic inflammation (e.g. long-term catheterisation or schistosomiasis). Less common in the UK.
E: Acute glomerulonephritis
Usually presents with microscopic haematuria, proteinuria, hypertension, and oedema rather than isolated painless visible haematuria.



