Becoming a vegetarian
Dear Friend,
Last week, I travelled to India for a dear friend’s wedding—a trip I always look forward to, but also one I’ve approached with some trepidation. For years, India has been synonymous with one thing for me: food poisoning. It’s almost become a rite of passage, unfortunately. And after a recent hospital admission with severe gastroenteritis, I was determined not to repeat that experience.
So, this time, I made a deliberate choice. For the entire week, I ate strictly vegetarian—no chicken, no fish, not even a crumb. It felt like a small act of self-care, a way of trying to protect my gut and see if a gentler diet might help.
The first few days were harder than I anticipated. I missed the taste and texture of meat more than I expected. It’s funny how much we get used to certain flavours, and how deeply they can become part of our daily comfort. Eating vegetarian felt unfamiliar and sometimes bland. I found myself thinking about those familiar meaty dishes I usually enjoy, especially after a long day.
But as the days went on, something shifted. By the end of the week, I genuinely didn’t mind at all. In fact, I noticed a real difference. My digestion felt lighter and smoother, and the bloating I often experience seemed to have eased significantly. I felt calmer, more settled in my body.

This experience made me reflect on what science tells us about vegetarian diets. There’s good evidence that eating more plants—fruits, vegetables, legumes, whole grains—can improve digestion, reduce inflammation, and lower the risk of chronic diseases like heart disease and diabetes. Plants are naturally rich in fibre, antioxidants, vitamins, and minerals that support overall health.
On the other hand, vegetarian diets require some thoughtful planning. Without meat, it’s important to be mindful of nutrients like vitamin B12, iron, omega-3 fatty acids, and complete proteins. But with a bit of effort, these gaps can be filled through supplements or plant-based sources.
I don’t see this as an all-or-nothing shift. Instead, I’m planning to reduce my meat intake—especially red meat—and aim for a more balanced diet overall. This week showed me that small changes can be surprisingly manageable and rewarding. It’s about nurturing my body and being kinder to myself.
Have you ever tried going vegetarian for a stretch? How did it feel? I’d love to hear your experiences or tips.
Drug of the week
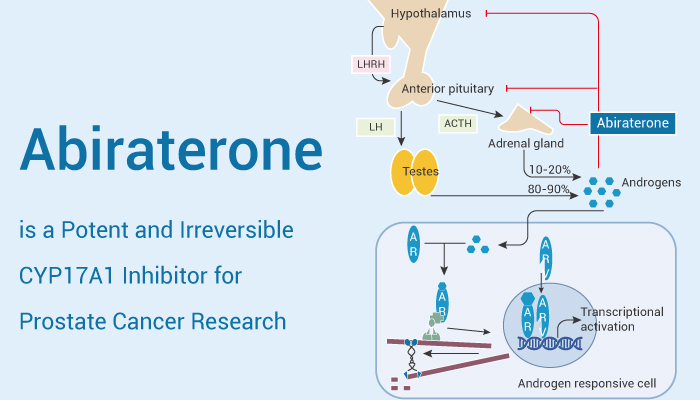
Abiraterone
Abiraterone is a drug used to treat prostate cancer.
It is given with androgen deprivation therapy and low-dose steroids.
Abiraterone blocks CYP17, an enzyme needed to make androgens.
This lowers testosterone from the testes, adrenal glands, and tumour.
By cutting androgen levels further, it slows cancer growth.
It improves survival in metastatic prostate cancer.
However, blocking CYP17 causes side effects.
It raises mineralocorticoids, leading to high blood pressure, low potassium, and fluid retention.
That’s why it must be given with steroids like prednisolone.
A Brain Teaser
A 68-year-old man presents to his GP with gradually worsening right knee pain over the past 2 years. The pain is worse with walking and climbing stairs and improves with rest. Morning stiffness lasts around 10 minutes. He denies joint swelling, redness, or systemic symptoms.
Past medical history includes obesity and hypertension.
On examination, there is bony enlargement of the right knee with crepitus on movement. Range of motion is reduced, but there is no warmth or effusion.
Plain radiography of the knee shows joint space narrowing and osteophyte formation.
What is the most appropriate first-line management?
A: Intra-articular corticosteroid injection
B: Total knee replacement
C: Regular paracetamol and topical NSAIDs
D: Oral methotrexate
E: Long-term oral NSAIDs
Answers
The answer is C – regular paracetamol and topical NSAIDs.
This is classic osteoarthritis.
Key features pointing to OA:
Gradual onset over years
Mechanical pain (worse with use, better with rest)
Short-lived morning stiffness (<30 minutes)
No systemic features
Bony enlargement and crepitus
X-ray showing joint space narrowing and osteophytes
Why the others are wrong:
A: Intra-articular corticosteroid injection
Useful for flares or persistent symptoms
Not first-line
B: Total knee replacement
Reserved for severe disease refractory to conservative management
Not initial treatment
D: Oral methotrexate
Used in inflammatory arthritis (e.g. rheumatoid arthritis)
OA is non-inflammatory
E: Long-term oral NSAIDs
Effective but not first-line due to GI, renal, and cardiovascular risk
Consider only if topical treatments fail



