Signing up to a nutritionist
Dear Friend,
Hope you all had a Merry Christmas. This is my last newsletter of this year, and it was hard to decide what to talk about. I could go over things I have learnt this year, or my new job, or recent life updates – but I suppose I should end 2025 looking ahead to the New Year rather than dwell on things in the past. One of my main targets of the New Year is to lead a much healthier lifestyle, whether that be physically or psychologically. And that’s why I decided to sign up to a nutritionist.
Over the last few months, ever since I was admitted to hospital, I’ve been noticing a troubling pattern: repeated infections and colds. It’s been frustrating and exhausting. Is it mental stress wearing me down? Or is it something physical? The honest answer is probably a bit of both.
But one thing people kept suggesting to me was my diet.
In medicine, we don’t often focus enough on nutrition beyond the basics. We routinely count calories—especially in oncology or chronic disease – but that’s not the whole picture. Calories tell us how much energy we’re consuming, but not what that energy is made of, or how the ingredients affect our immune system, gut health, or overall resilience.
For example, emerging research shows that micronutrients like vitamin D, zinc, and selenium play critical roles in immune function. A 2020 review in Nutrients highlighted how deficiencies in these can increase susceptibility to infections – and yet, these aren’t routinely checked in standard medical care unless there’s a clear deficiency or malnutrition. The food we eat affects not just our weight, but our body’s ability to repair and defend itself.
And for me, things went beyond immunity. At the age of 28, it’s not normal to feel extremely bloated after a spicy meal, a large meal, or even a glass of wine. Sometimes the bloating comes for no obvious reason. It reached the point where I was genuinely afraid to enjoy social occasions like Christmas or New Year’s Eve, worried that one wrong bite would flare up my gut and send me into days of discomfort.
That’s why this week I finally took the step to see a nutritionist.
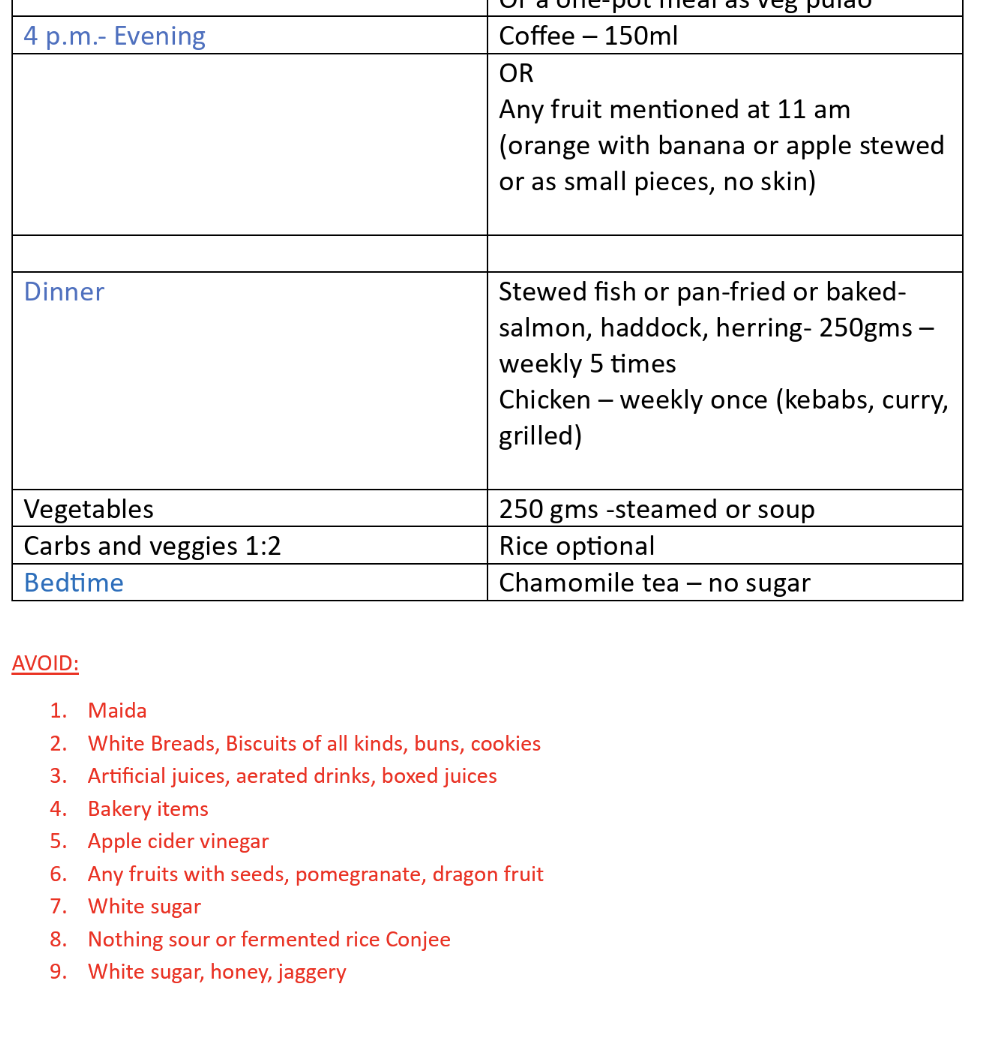
My Diet Plan
My first session was eye-opening. The plan she designed for me seems simple on paper but feels revolutionary in practice. One surprising takeaway: she wants me to eat more, not less. That goes against the usual narrative of calorie restriction for weight control. Instead, the emphasis is on quality and balance – more vegetables and fruits, less red meat, and a real focus on hydration. Studies have shown that a diet rich in plant-based foods can reduce inflammation and improve gut microbiota diversity, both crucial for digestive health and immunity.
She also gave me a list of “red flag” foods to avoid – many of which happen to be my favourites. Processed meats, excessive alcohol, and highly spicy dishes all made the cut. It’s a reminder that what we crave isn’t always what’s best for our bodies.
I’ll be tracking my progress closely. The plan includes monitoring symptoms, energy levels, and overall wellbeing week by week. If I can start 2026 feeling healthier, more energised, and less at the mercy of my gut, that will be a real win.
I’m hoping this journey will not only help me physically but also shift how I think about nutrition. Because in medicine, we’re experts at managing disease, but sometimes we forget the basics – like how food fuels the healing process itself.
I’ll keep you posted on how it goes.
Have a great year ahead and thank you for your support over the last 12 months.
Drug of the week
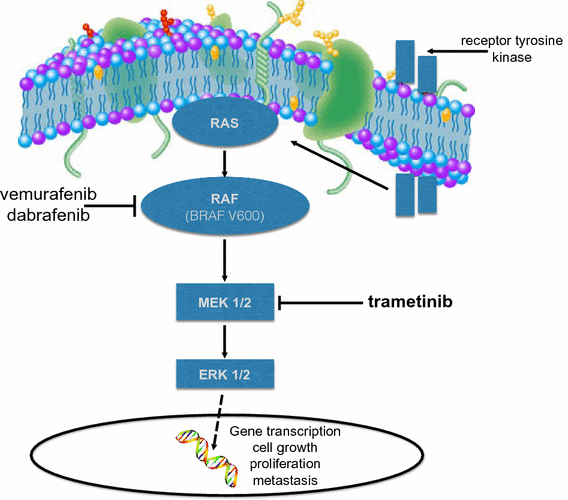
Dabrafenib
Dabrafenib is a targeted therapy for cancers driven by BRAF V600 mutations — most famously melanoma, but also lung and thyroid cancers.
It’s a BRAF inhibitor, designed to shut down a constitutively active kinase in the MAPK pathway.
In BRAF-mutant cells, the pathway is stuck in the “on” position, which leads to uncontrolled cell division.
Common side effects include fever (often recurrent), fatigue, arthralgia, rash, and hyperglycemia.
Pyrexia is the signature toxicity—and the one that most often disrupts treatment.
A Brain Teaser
A patient is furious about an aspect of their care you provided. Before you’ve had a chance to discuss the situation they demand you full name and GMC reference number.
What should you do?
A: Withhold this information until you’ve had a chance to discuss the issue
B: Give them both details
C: Refuse to speak to them until she has calmed down
D: Withhold the information until you know what they intent to do with it
E: Instead give them information regarding your practice’s complaints procedure
Answers
The answer is B – give them both details.
The GMC states ‘If someone you have contact with in your professional role asks for your registered name and/or GMC reference number, you must give this information to them’
You cannot withhold this information.
GMC ethical guidance: Treat patients and colleagues fairly and without discrimination. Paragraph 64



